Science
'We've created medical refugees.' LGBTQ+ healthcare workers fight for gender-affirming care amid rise in anti-trans laws

Nico Olalia had just finished her initial nurse training in the Philippines when she realized her aspirations were growing bigger than her home archipelago.
“There are a lot of trans Filipinos, but they’re always known in the beauty industry, and they’re very seldom found in the professional side,” Olalia said.
So she moved back to the United States, where she was born, for better career prospects. Today, she is a clinical nurse at Cedars-Sinai, one of the largest hospitals in Southern California, where she assists new hires and cares for patients in the neurology division.
Olalia feels like it’s a dream come true; her peers and patients respect her and welcome her contributions. It’s a hope shared by a small but growing number of trans and nonbinary healthcare workers in the U.S.
Yearly surveys of first-year medical students by the Assn. of American Medical Colleges show that the percentage identifying as transgender and gender nonconforming doubled from 0.7% in 2020 to 1.4% in 2023.
These numbers align with the growing LGBTQ+ population in the United States. Today, younger generations are more likely to identify as LGBTQ+ than generations before. A national survey this year found that 28% of Gen Z respondents identified as lesbian, gay, bisexual, transgender or queer.
But that rise in LGBTQ+-identified youths and trans healthcare workers has coincided with escalating restrictions on gender-affirming care.
Between 2022 and 2023, anti-trans legislation proposed across statehouses tripled, with a majority of the bills proposing restrictions on gender-affirming care. According to the Movement Advancement Project, at least half of the states exclude transgender-related healthcare for youths from their Medicaid programs, while only 22 explicitly cover it.
U.S. Assistant Secretary for Health Rachel Levine, center, is shown at a transgender health event in Miami with Tatiana Williams, left, of Transinclusive Group and Arianna Inurritegui-Lint of Arianna’s Center.
(Wilfredo Lee / Associated Press)
“We’ve created medical refugees who have to leave their state to get that care,” said U.S. Assistant Secretary for Health Rachel Levine, the first transgender person confirmed by the Senate to a high government post.
“Transgender medicine can be suicide prevention care. It’s been shown in many studies that it improves the quality of life and can save lives for youth and adults,” said Levine, a pediatrician specializing in adolescent care.
When Levine was doing her medical residency at Mount Sinai Hospital in New York City during the 1980s AIDS crisis, she saw friends and co-workers succumb to the epidemic — an experience that rings eerily familiar to the discrimination she sees transgender people facing today, she said.
One study from 2023 showed that 70% of transgender and gender nonconforming patients faced at least one negative interaction with a healthcare provider, ranging from an “unsolicited harmful opinion about gender identity to physical attacks and abuse.” It was only in 2019 that the World Health Organization removed gender dysphoria from its list of mental health illnesses.
Alex Keuroghlian, a clinical psychologist at Harvard Medical School, directs training programs through the National LGBTQIA+ Health Education Center that educate healthcare providers across the country on gender-affirming care. They’ve noticed a double standard when it comes to the doubts that people raise against transgender healthcare.
“Given how well resourced anti-trans political groups are, it can really distort the public discourse and make it harder to advance evidence-based, clinically sound practices,” Keuroghlian said of the rampant misinformation they’ve seen online.

Mack Allen, an 18-year-old transgender high school student from Leavenworth, Kan., stands with other young advocates of LGBTQ+ rights after a rally at the state capitol in Topeka, Kan.
(John Hanna / Associated Press)
An uptick in the number of transgender-identifying youths seeking gender-affirming care sparked a theory that “social contagion” was influencing teens to experience “rapid-onset gender dysphoria.” Some practitioners oppose this framing, and research published by the American Academy of Pediatrics has disproved it. Both the American Psychiatric Assn. and the American Pediatric Assn. support gender-affirming care for adolescents.
The news on the legal front hasn’t been all bad for trans healthcare providers; last month, a federal court judge struck down Florida’s law restricting gender-affirming care for minors and adults. However, the practice of categorizing gender in a binary medical system continues.
That’s problematic, said Mauricio Dankers, the intensive care unit director at HCA Florida Aventura Hospital, because the medical erasure of trans people can prevent a proper diagnoses. When doctors have to make split-second decisions in the ICU, he said, failing to recognize a transgender person could prevent them from receiving lifesaving care.
“If I don’t know that a transgender woman may have gone through laryngoplasty to change the tone of her voice, I’m going to go and put the breathing tube [and] I may run into trouble,” Dankers offered as an example. Chest binding used by some transgender people to appear more masculine can also lead to pneumonia if done improperly, he said.

Violet Rin, a transgender woman in Florida, gives herself estrogen injections once a week.
(Francine Orr/Los Angeles Times)
Dankers, a gay immigrant who left Peru for the more tolerant New York City, worries that the politicization of transgender healthcare will put a target on LGBTQ+ healthcare providers.
These restrictions “are going to change how the LGBTQ+ trainee thinks about their career,” Dankers said. He said they might think, “I’m not going to a place where they don’t want me by law.”
After Texas banned gender-affirming care for teens, a pediatric endocrinologist closed her practice and moved out of the state because she feared violence from armed protesters. And this year, a Texas man was sentenced to three months in prison for threatening a Boston physician serving transgender patients.
Fear and violence have had a ripple effect even on states that have enshrined transgender healthcare into law.
Baltimore Safe Haven, a nonprofit that provides transitional housing service focused especially on Black trans women, received an increase of 7,000 calls last year after Gov. Wes Moore signed an executive order protecting gender-affirming medical care in Maryland, according to the Baltimore Sun. Most of the callers lived out of state.
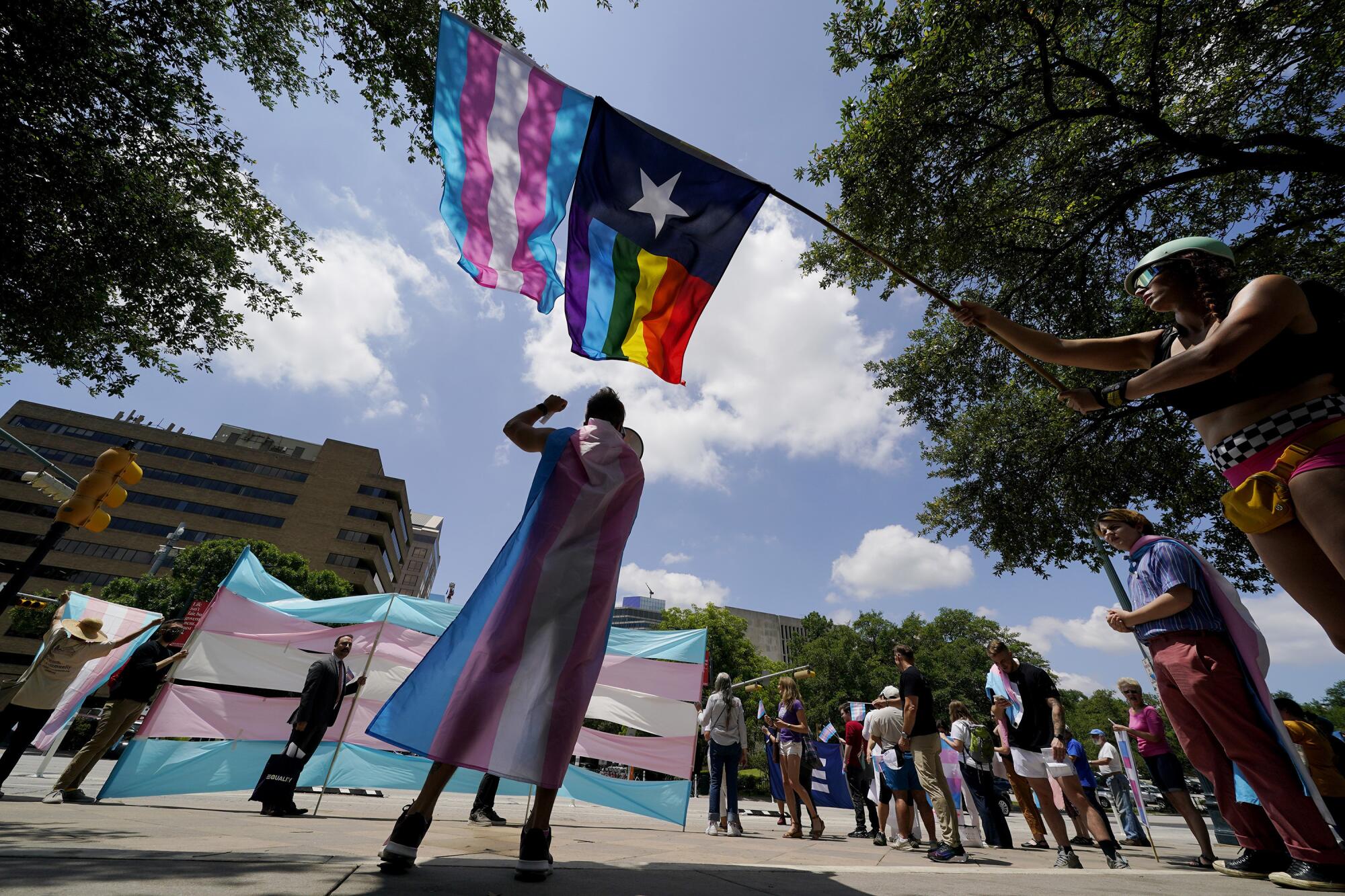
Demonstrators gather on the steps to the state capitol to speak against transgender-related bills being considered in the Texas Legislature.
(Eric Gay / Associated Press)
“I can’t even see my own doctor,” said Jules Gill-Peterson, a transgender woman and associate professor at Johns Hopkins University in Baltimore who studies the history of transgender medicine. Anecdotally, she’s heard of doctors’ caseloads tripling with the slew of requests they receive from new transgender patients.
“It’s only going to put greater pressure on [the] system as people migrate from states where it’s illegal to transition medically to states where it’s not,” Gill-Peterson said.
LGBTQ+ healthcare workers are on the defensive, said Kate Steinle, a queer nurse and chief clinical officer at Folx, a nationwide healthcare provider that serves transgender and queer patients.
“Our general counsel wakes up in the morning and is looking at every single possible legislation that could affect our care,” Steinle said. Folx lobbies the government to ensure that its patients have access to gender-affirming care, but Steinle said fighting anti-trans legislation can sometimes feel like “a game of whack-a-mole” — as one goes down, another takes its place.
Anti-trans legislation is largely symbolic because most of these bills fail, said D Dangaran, a lawyer and director of gender justice at Rights Behind Bars. According to the Trans Legislation Tracker, of the 617 bills introduced, 44 have passed, 348 failed and the rest are pending.
But the fate of transgender healthcare could shift dramatically depending on the outcome of the presidential election in November.
“A Trump presidency will signal to the states another possibility to move forward on all fronts with anti-trans legislation,” Dangaran said. Former President Trump has promised to end gender-affirming care for minors if he wins, and Dangaran anticipates that he would sign “executive orders that are antithetical to protecting trans rights.”

Glenda Starke wears a transgender flag as a counterprotest during a rally in favor of a bill to ban gender-affirming care at the Missouri Capitol in Jefferson City, Mo.
(Charlie Riedel / Associated Press)
Keuroghlian worries that many career government employees in the Department of Health and Human Services could be ousted by political appointees as part of Trump’s ambition to reshape the federal workforce. “There is a lot of important healthcare and research funded by the federal government,” he said.
All of this could reverse the progress that the Biden administration has done to advance gender-affirming care across the country.
“There hasn’t been any president that has more explicitly supported access to gender-affirming care,” said Elana Redfield, the federal policy director at the Williams Institute at UCLA School of Law.
Last week, the Supreme Court agreed to consider the Biden administration’s challenge to Tennessee’s ban on gender-affirming care for teens. The administration argues that the ban violates the 14th amendment’s equal protection clause. A ruling is expected next year that could cement or further erode transgender rights.
Redfield warns that “people who are multiply marginalized are also most affected by these laws,” particularly people of color who live in the Deep South. Beyond the legal restrictions to care, they face problems affording the cost of procedures such as gender-affirming surgery and traveling to where care is available, she said.
Nor can lower-income transgender people afford Folx, a private subscription service that charges $39.99 a month on top of any out-of-pocket costs and co-pays levied by an insurer.
“Trans people have a lot to tell us about just how bad U.S. healthcare can get,” Gill-Peterson said. “Trans healthcare is not really that different than the rest of healthcare.”

People attend a rally as part of a Transgender Day of Visibility on March 31, 2023, by the U.S. Capitol in Washington.
(Jacquelyn Martin / Associated Press)
Increasing the representation of transgender people in a healthcare system where “profit is placed over people” won’t solve those fundamental inequities, she said. Even if doctors support their transgender patients, Gill-Peterson said, they are still bound by law to follow state regulations and insurers’ dictates.
On the other hand, studies have linked positive health outcomes in LGBTQ+ patients and patients of color to having a healthcare provider who shares their background. That’s one reason University of Michigan medical student Gaines Blasdel, a trans man, wants to become a urologist who can provide gender-affirming surgery to transgender patients such as himself.
Blasdel said gender-affirming care can be an abstract social justice issue to his cisgender classmates, but it isn’t to him. “I’ve been embedded [in medicine] and I’m going to be, no matter how hard it is.”
Jona Tanguay, a physician assistant and medical lead in the medical substance use disorder programs at Whitman-Walker Health in Washington, D.C., said it’s important not to discredit the incremental but meaningful progress in the representation and quality of care offered to transgender people.
“Progress isn’t always linear,” they said. Tanguay, who is nonbinary, is also the president of GLMA, formerly known as the Gay and Lesbian Medical Assn. They already see the curriculum expanding and the number of out transgender healthcare providers growing steadily. “Every generation after is going to be more self-aware than they used to be about health disparities.”

Nico Olalia, a transgender woman, moved back to the United States from the Philippines for better career opportunities as a nurse.
(Jireh Deng / Los Angeles Times)
Olalia said her story demonstrates that trans people can practice medicine just as well as their cisgender colleagues. Because she’s also enrolled full time in a nursing doctoral program, her days start at 4:30 a.m., when she wakes up to prepare for her 10- to 12-hour shifts. Her efforts at Cedars-Sinai earned her a prestigious $10,000 no-strings-attached grant from the Simms/Mann Institute & Foundation.
“I do hope that I can have more power to inspire transgender women,” Olalia said. “I want those who are walking behind me to … have that opportunity to go beyond what they’re told to do or what society deems them to be.”

Science
Pacifica pier cracks, another coastal casualty as seas continue to rise

The Pacifica Municipal Pier was shut down and taped off Thursday after city workers noticed cracks running through the landmark structure and concrete chunks falling into the ocean.
It’s just one of many coastal California structures that have recently crumbled under pressure from a rising and relentless ocean.
Officials from the small, beach city south of San Francisco said the pier was closed due to “cracking, separation, and displacement of the concrete walkway and structural elements.”
It will stay closed while structural engineers asses its safety.
Photos taken by city employees show a wide crack that runs from top to bottom and across the structure as well. Other photos show a large horizontal crack under the foundation of a small restaurant on the pier, the Chit Chat Cafe.
The cafe was also shut down.
This is not the first time the 53-year-old pier has shown signs of stress. In 2021, part of it was shut down after handrails along the edge collapsed. And in 2023, after a series of storms pummeled the Central California coast, damaging parts of the pier, the structure was partially closed for more than year.
Those same storms caused extensive damage in Aptos and Capitola, 70 miles south, where piers and waterfront infrastructure were swept away or damaged.
In 2024, a 150- to 180- foot section of the Santa Cruz wharf was ripped off by powerful waves.
At least 10 of the state’s dozens of coastal public piers were closed for part or all of 2024 due to structural damage sustained in winter storms since 2022. At least five others have longer-term upgrades planned to address structural issues.
“These things are costly to maintain,” said Zach Plopper, senior environmental director at Surfrider. “They are a part of our California coastal culture in many ways, but we’re going to need to reckon with, one, the state that they’re in, and two, the continuous and worsening threats they’re going to experience,”
He said most of the piers were constructed in the early 1900s, and they weren’t built to withstand decades of rough seas, storms and rising sea level.
“With this incoming El Niño, which is forecasted to be significant, and this marine heat wave we’re in the midst of, we’re kind of in uncharted waters as far as what this winter could bring in terms of storms and swells to the California coast, and we’re likely going to see a lot more damage,” he said. “Not just piers, but roads and other coastal infrastructure up and down the state.”
There was no storm in Pacifica earlier this week, so no single event could be blamed for the destruction.
However, a 2025 report from an outside engineering firm, GHD, found that several sections of the pier were in “poor” or “serious” condition, and they recommended closure before anticipated storms or events that could “subject the piles to high winds, swells and large waves.”
The firm found several areas of the pier where concrete was missing and rebar was exposed and corroding.
“The pier has continued to experience high winds and large waves in a harsh marine environment,” the engineers wrote in the report, noting that continuous exposure to seawater or marine spray was “detrimental” to the structure.
A 2023 city report estimated it would cost $19 million to repair.
That same year, a state law was enacted to require local governments along the California coast to plan for sea level rise in the coming decades.
Sea level has risen some 8 inches, on average, along the coast in the past 150 years, Plopper said, and researchers anticipate another foot in the next 25 years.
“We’re going to see profound shifts on our coastline, none that we have ever experienced before, and building static structures on the coast just doesn’t work all that well,” he said. “We’re going to have to make some really hard decisions.”
Science
L.A. region begins the year with the smoggiest first 5 months in a decade

The first five months of 2026 in Southern California have been the smoggiest — with the highest number of unhealtful air days — in more than a decade, according to statewide air monitoring.
So far this year, the South Coast air basin, which includes Los Angeles, Orange, Riverside and San Bernardino counties, has seen 39 days when the concentration of lung-irritating ozone (commonly known as smog) exceeded the federal standard, according to preliminary state air quality data.
That’s even worse than the infamously hot and hazy 2017, when Greater Los Angeles had 36 unhealthful air days by June 4 and ultimately saw 145.
Many of the roughly 18 million people who live in the air basin have been subjected to unhealthful levels of ozone, a highly corrosive gas that triggers asthma attacks and a wide range of respiratory illnesses. This has taken many by surprise since successive days of smog more commonly happen in summer, when heat waves and intense sunlight convert man-made pollution into ozone.
“If we have this many violations by this time, this could be a really awful year for air quality,” said Adrian Martinez, director of Earthjustice’s Right to Zero campaign, an initiative calling for the transition away from fossil fuels. “We’re already the worst place in the country for summertime smog pollution. So it could be one of the worst years in one of the worst places in the country.”
The pollution has been especially severe in valleys. On April 18, an air monitor in Reseda in the San Fernando Valley measured the second highest spike in hourly ozone levels in the last decade.
Greater Los Angeles has seen more high-smog days so far in 2026 than any other year in the past decade.
(Courtesy of South Coast Air Quality Management District)
The South Coast Air Quality Management District says the high ozone levels are due to early heat waves. Officials said they were not aware of any increase in the pollutants — most of them from different kinds of exhaust — that lead to ozone formation.
Local temperatures have been well above normal, climbing into the mid-80s and high 90s between January and April, breaking several daily high temperature records, according to the National Weather Service.
March in particular was the warmest on record in California. Riverside had an unprecedented 13 days of temperatures above 90 degrees, the weather service said.
“It was really that heat wave — conditions we typically see in July or August, we saw them in March,” said Sarah Rees, deputy executive officer of the air district. “That put us ahead of the curve in terms of how much ozone we got.”
Air district officials urged residents to monitor pollution levels on the agency’s website and mobile app, and spend only limited time outdoors when smog levels are high.
“People generally know when there’s a wildfire, because you see the smoke and smell it,” said Scott Epstein, the air district’s manager of planning and rules. “Then, it’s like, I’ve got to take precautions. Ozone, you can’t really tell.”
Southern California has been particularly susceptible to smog formation because of its millions of gas-powered cars releasing tons of tailpipe emissions each day. The region’s sunshine acts as a catalyst for smog formation. Then the mountains trap this pollution over densely populated communities.
For nearly half a century, state and local air regulators have made rules designed to alleviate this pollution, enacting the nation’s first tailpipe emission standards in 1966 and requiring catalytic converters in 1975.
Smog-forming pollution has been dramatically reduced over the last two decades, but the region still does not meet federal air quality standards for ozone.
At an air district meeting Friday in Diamond Bar, the governing board held a moment of silence for William Burke, a former longtime chair. During his tenure, the agency enacted nearly 270 rules that are credited with reducing smog-forming pollution by hundreds of tons per day. Burke, who also founded the Los Angeles Marathon, died in May at 87.
“Those are just emission reductions,” air district Chair Michael Cacciotti said at the Friday meeting. “But what it doesn’t tell you is how many kids, families, seniors were prevented from going to the hospital from an asthma attack, didn’t get cancer or other respiratory problems.”
Several residents from the Inland Empire, which suffers some of the worst smog pollution, expressed their appreciation for the air district’s efforts. But they also stressed the need for more progress.
“I’m old enough to remember growing up in the ‘70s and ‘80s … and not being able to see the mountains for weeks and months at a time,” said Erik Morden, one of several residents who spoke at the meeting.” I know things have improved, and I want to thank all of you for all the hard work that you’re doing. But there’s a lot of invisible stuff that you don’t see, that’s still out there — a lot of particulates in the ozone and chemicals that are causing a lot of problems.”
Martinez, the Earthjustice attorney, said the abnormally early outbreak of smog should be a wake-up call to government regulators that there’s work to be done, including offering more incentives to help residents and businesses transition to zero-emission appliances.
“We shouldn’t over-complicate it. We’ve got a lot of heat, we’ve got a lot of pollution,” Martinez said. “Our contention is, this agency can’t control the weather. But the one thing it can control is the pollution.”
Science
A flesh-eating worm from the 1960s is re-invading the U.S. Are CA cattle at risk?

Federal agricultural inspectors detected a case of New World screwworm larvae — maggots that burrow into the flesh of living animals and sometimes humans — on a 3-week-old calf in south Texas, near the U.S.-Mexico border. Officials anticipated the arrival of screwworm in the United States and say they’re prepared to contain it.
New World screwworm, also known as Cochliomyia hominivorax, is starkly different from the average maggot that feeds on decaying organic matter such as garbage, rotting food or dead animals, said Tom Talbot, veterinarian and member of the California Cattlemen’s Assn.
That’s because a screwworm larva “attacks living flesh,” Talbot said.
On Thursday, the U.S. Department of Agriculture confirmed the detection of New World screwworm in the umbilical area of a bovine in Zavala County, Texas, more than 60 miles from the northern Mexico border.
As of Friday morning, there have been no additional cases of infected animals reported.
Screwworm is endemic in South America and parts of the Caribbean, according to the Centers for Disease Control and Prevention. However, the parasitic fly has been steadily moving north from Central America to Mexico since 2023.
The USDA says it has actively monitored the fly’s movement. Last month, the USDA was aware of more than 200 active screwworm infestation cases in the border states of Nuevo León and Tamaulipas, according to Mexico’s Secretary of Agriculture and Rural Development dashboard. There are currently more than 2,000 active cases throughout Mexico.
It was believed that the New World screwworm would enter the U.S. in 2025, “however, thanks to the hard work across the entire Trump administration and our industry, state, and local partners, we were able to buy time for this moment,” said Dudley Hoskins, undersecretary for Marketing and Regulatory Programs for the USDA, in a statement.
The potential economic impact of New World screwworm on the cattle industry due to import restrictions, reduced productivity and animal loss is substantial, said Sally DeNotta, director of the University of Florida’s Equine Performance Laboratory.
Last year, 175 key agricultural organizations signed a letter urging additional federal funding for screwworm-control measures, emphasizing USDA estimates that a New World screwworm outbreak in the U.S. could cost producers $4.3 billion annually and cause economic losses of more than $10.6 billion across the southern United States.
“While the fly does not survive at temperatures at or below freezing, infected animals could carry the parasite northward and spread infection during the summer months, and the temperate climate of Southern California could certainly support year-round New World screwworm populations,” DeNotta said.
Talbot said from the federal to the local level, everyone in the ranching community has been talking about the arrival of screwworm and how to combat it.
“My expectation is that there will be a minimal number of cases of [New World screwworm] in California,” he said.
That’s because there are several stations on the border in Southern California, he said, that are collecting data, monitoring for any incidents of the parasitic fly and trapping them.
Talbot says he’s confident that the proactive measures on behalf of the federal government will mitigate the screwworm’s reach and therefore not impact the beef supply locally or nationally.
How screwworm infection spreads
Female screwworm flies are attracted to the smell of wounds — that can be as small as a tick bite — and body openings such as the nose, eyes, ears and mouth where they can lay eggs, according to the CDC.
A female screwworm fly can lay 200 to 300 eggs at a time and may lay up to 3,000 eggs during her 10 to 30-day lifespan.
When the eggs hatch into maggots, the maggots eat live tissue, causing a worsening, often painful and foul-smelling wound, according to the CDC.
Screwworm has hit the United States before
There was a screwworm outbreak in the southwestern region of the United States in 1965 that prompted Mexican and U.S. livestock producers to sign a declaration to establish a joint program for the eradication of the screwworm from the states on either side of the Mexico-U.S. border, according to the National Agricultural Library.
By 1966, the United States had eradicated screwworms, but livestock remained vulnerable to reinfestation from screwworms migrating from Mexico.
Eradication was possible through the sterile insect technique, which uses gamma radiation to irradiate screwworm pupae and create sterile male flies.
The U.S. Department of Agriculture’s Animal and Plant Health Inspection Service maintains a screwworm pupae sterilization facility in North America and is currently building a new center in southern Texas.
When produced and released in large numbers, sterile male flies mate with wild female flies, which then lay unfertilized eggs, according to the USDA.
“Since female screwworm flies normally mate only once, the population progressively reduces and is, ultimately, eradicated,” according to USDA officials.
Last year, the Trump administration cut thousands of grants and programs from the U.S. Agency for International Development, which includes U.S.-funded animal disease monitoring projects operated by the United Nations Food and Agriculture Organization, Argi-Pulse Communications reported. Among the slashed programs were some dedicated to monitoring and containing New World screwworm in Central America.
Today, screwworm infestations aren’t a regular occurrence in the U.S., but cases have occurred in travelers returning from areas where the flies are present, according to the CDC.
Can infected animals be treated?
Infected wounds are cleaned and debrided to remove any screwworm larvae, after which the animal is treated with an approved insecticide, DeNotta said.
Last month, the U.S. Food and Drug Administration issued an emergency use authorization for several insecticides known to be effective against screwworm.
There are approved systemic and topical options for a variety of species, including cattle, horses, small ruminants, cats and dogs, DeNotta said.
“Multiple days of treatment are often required, and antibiotics and analgesics may also be administered to treat secondary infection and control pain,” she said.
If left untreated, the tissue destruction caused by flesh-eating larvae can be extensive and severe, often resulting in debilitation and eventual death of the host, DeNotta said.
“Animals that survive may suffer weight loss, poor growth and reduced productivity as a result of pain and discomfort,” she said.
Screwworm can infect humans
Human infection is rare, DeNotta said, but it can happen.
Humans are at risk of being infected by screwworms if they travel to an area where the flies are present, such as South America and the Caribbean, according to the CDC.
CDC officials said your risk of screwworm infection increases when you:
- Spend a lot of time outdoors during the day, especially if sleeping or unable to keep the flies at bay.
- Have any open wounds. A small break in the skin, including from a scratch, insect bite or recent surgery, may attract screwworm flies.
- Have a medical condition that causes bleeding or open sores, such as from skin or sinus cancer, or from treatments that can create breaks in the skin.
- Live, work or spend an extended amount of time with or near, livestock or other warm-blooded animals in areas where screwworm flies are present.
The symptoms humans experience when infected by screwworm
The following are symptoms of screwworm according to the CDC:
- Feeling maggots move or seeing maggots within a skin wound, sore or body opening.
- Painful skin wounds or sores that worsen within a few days.
- Foul-smelling odor from the site of the infestation.
- Bleeding from open sores.
Bacteria can also infect wounds where screwworm maggots are present and may cause an infection that can lead to symptoms like fever or chills.
To treat a screwworm infection, DeNotta said, people undergo the same combination of wound debridement and insecticides used in animals.
-

 Sports1 minute ago
Sports1 minute agoVictor Wembanyama puts hand on Jalen Brunson’s head, pushes him down as refs look the other way in Game 3
-

 Technology6 minutes ago
Technology6 minutes agoRobot pets with AI could soon live with you
-

 Business14 minutes ago
Business14 minutes agoMusicians shortchanged by AI deals with labels, lawsuit alleges
-

 Entertainment16 minutes ago
Entertainment16 minutes agoOf course, Supergirl can have pierced ears. James Gunn explains it again for those who forgot ‘Superman’
-

 Lifestyle21 minutes ago
Lifestyle21 minutes agoL.A. Affairs: I’m a black woman. He’s a white guy with a pickup truck. Here’s what happened
-
Politics29 minutes ago
Disability rights advocates protest Newsom’s proposed cuts to in-home support services
-

 Sports37 minutes ago
Sports37 minutes ago‘It would be a fun year.’ Rams all for Aaron Donald returning to pair with Myles Garrett
-

 World47 minutes ago
World47 minutes agoUN questions legality of Israeli forced evacuation orders in Lebanon
