Science
Opinion: Surgeons give patients too many opioids. A few simple steps could curb excess prescribing
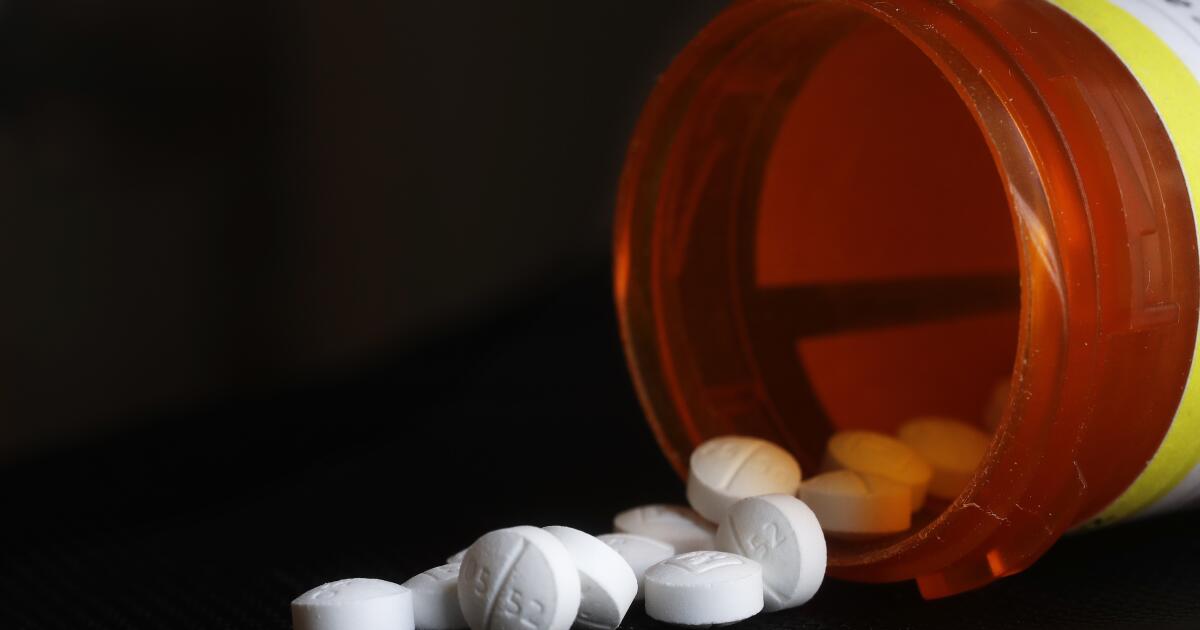
America’s opioid epidemic is as bad as it has ever been. Although the sharp increase in opioid overdose deaths over the last decade is largely attributed to the rise in fentanyl distributed through drug cartels, a startling number can be traced to prescriptions. In fact, the Centers for Disease Control and Prevention estimates that 45 people died each day in 2021 from a prescription opioid overdose — about one-fifth of all opioid-related deaths.
Some efforts to curb opioid prescribing have shown promise, including prescription drug monitoring programs, promotion of alternative analgesics, provider education and informing prescribing physicians when their patients die from opioid overdoses. But there is one medical specialty for which opioids are still a crucial part of most patients’ treatment plan: surgery. Nearly every patient discharged after surgery leaves the hospital in significant pain, which is why surgeons prescribe more opioids than almost any other specialty.
Most patients, however, do not use all the opioids they are prescribed after an operation. That leaves excess pills in circulation and helps fuel the epidemic. If we could get surgeons to prescribe only the number of pills patients need for their own use, this could greatly reduce the number of excess pills available for diversion and misuse, among patients, their families and members of their communities. This, in turn, could reduce addiction and overdoses.
Minimizing how often a surgery patient ends up with extra opioids would not solve the crisis, but it’s part of the solution — and it’s achievable.
Changing prescribers’ behavior is hard. They get set in their ways, moored by a strong belief that what they are doing is best for their patients. Moreover, they strenuously resist attempts to constrain their freedom to decide what is best. Our research team looked to behavioral science for ways to nudge providers to prescribe in accordance with best practices, while leaving them with full autonomy to choose what they think would be best.
Conventional strategies for curbing excessive opioid prescribing assume that surgeons are rational actors who, whenever they are informed about patient needs and incentivized to attend to them, will act to maximize the welfare of patients. If that were the case, simply educating doctors about the dangers of overprescribing might be sufficient.
However, numerous studies from experimental psychology and behavioral economics have shown that people are highly selective in the information they focus on and more socially minded than traditional models of rational self-interest would predict.
Such insights from behavioral science provide promising avenues for curtailing excessive opioid prescribing by surgeons. For instance, one group of researchers found that setting the default opioid quantity in the electronic health record system to match the amount patients actually use substantially reduces the amount of opioids prescribed. Apparently, busy surgeons tended to go with the flow when prescribing — presumably because the default number of pills became a salient reference point, was easiest to enter and suggested a norm of correct behavior.
Surgeons, like other humans, are social animals who are strongly motivated to adhere to the norms of good behavior endorsed by their peers. We capitalized on this for our recent study, a randomized trial to test two simple interventions across 19 hospitals in Northern California for a year.
In one version, the emails informed surgeons that they had prescribed more pills than other surgeons in their health system had been prescribing for the same procedure. This message highlighted “descriptive” norms of actual behavior. In a second, simpler version, whenever a surgeon prescribed opioid amounts that exceeded recommended quantities for the procedure they had performed, we sent the doctor an email notification informing them. This intervention highlighted “injunctive” norms of ideal behavior.
Surprisingly, both social norm interventions had the exact same impact on prescribing. Subsequent patients were about 25% less likely to receive an opioid prescription that exceeded the recommended amount. This resulted in about 42,000 fewer pills in the community for the 26,000 patients who were part of the intervention group.
Imagine how many fewer pills would be prescribed if this were scaled up nationwide, given that there are more than 50 million inpatient surgical procedures performed each year in the U.S. Surely this would lead to millions, if not tens of millions, fewer opioid pills circulating in the U.S. each year.
Inexpensive solutions grounded in evidence on human behavior can be powerful tools in our campaign against opioid addiction. Sometimes just a light touch — a tweak to the default settings in the electronic health system or an automated email to surgeons — can have an outsize effect on prescribing decisions with life-or-death consequences.
Zachary Wagner is a health economist at USC and Rand. Craig R. Fox is a professor of psychology and medicine at UCLA and chair of the Behavioral Decision Making Area at the UCLA Anderson School of Management.

Science
Video: NASA Announces Artemis III Crew

new video loaded: NASA Announces Artemis III Crew
transcript
transcript
NASA Announces Artemis III Crew
NASA announced the crew of Artemis III mission, which will fly to low-Earth orbit to test rendezvous and docking maneuvers with one or two lunar landers.
-
“I am excited to welcome you as the next crew in the Artemis journey to successfully return to the moon — this time to stay.” “I’m honored by the role that I’ve been given. I’m also very humbled by the task in front of us. But first and foremost, I’m grateful.” “So with that, the Artemis II crew, comrade, hands you the baton. You got the controls.” “As you know, we had a significant anomaly at our Launch Complex 36A on May 28. We’ve redoubled our efforts and are moving forward.”
By Alisa Shodiyev Kaff
June 9, 2026
Science
Santa Monica Mountains’ last steelhead trout survived the Palisades fire — and even had babies

Scientists feared the Santa Monica Mountains’ last remaining steelhead trout were dead, smothered by debris flows unleashed by the Palisades fire.
But the endangered fish surprised them: A team of biologists recently spotted 30 of the rare trout — and 21 babies — in Topanga Creek.
“There was a lot of happy dancing in the creek,” said Rosi Dagit, principal conservation biologist for the Resource Conservation District of the Santa Monica Mountains, which works with public and private landowners to conserve natural resources.
That’s because the steelhead here are endangered, at both the state and federal levels. Once, they swam in most streams of the Santa Monicas, but their numbers plummeted amid overfishing and coastal development. Increasingly frequent wildfire has further stressed their habitat. Topanga Creek, a biodiversity hot spot, is home to their last known population in the mountains that stretch from the Hollywood Hills to Point Mugu in Ventura County.
The trout that were spotted, including this one, are part of a distinct Southern California population that’s listed as endangered at the state and federal levels.
(RCDSMM Stream Team)
The California Department of Fish and Wildlife spearheaded a complex mission to rescue trout threatened by the Palisades fire that sparked in January 2025.
Time was of the essence. The fire hadn’t yet been fully contained. But rain was on the way, which would sweep massive amounts of sediment from the denuded hillsides into the water. Fish are often killed this way.
Crews stunned the fish with electricity, scooped them up in buckets, trucked them to a hatchery and ultimately moved them to Arroyo Hondo Creek in Santa Barbara County.
Within days, Topanga Creek was choked with mud. Some assumed the fish left behind were goners.
But in March, the conservation district’s team found four. The following month, when water conditions were clearer, they saw more.
“These fish continue to amaze me,” said Kyle Evans, environmental program manager for the state Department of Fish and Wildlife, who had seen the damage to the creek. “I had seen populations get wiped out in similar situations. So when I heard, I was thrilled.”
Evans surmises the fish that survived were in an area of the creek where less charred material and sediment were swept in.
“These fish likely hunkered down, were hiding under some rocks or places to try to get away from the main concentration of flow,” he said. “And luckily they weren’t buried.”
The ones that were spotted were fairly small, around 6 to 14 inches. Rainbow trout and steelhead trout are the same species, but with different lifestyles. If the fish remain in freshwater, they’ll be considered rainbows. However, they can migrate to the ocean and become steelhead, where they typically grow larger before returning to their natal waters to spawn.
Topanga Creek hasn’t fully recovered from the damage it sustained, but scientists say it’s looking better. Surveys last year were “so depressing,” Dagit said, with very few animals, and stretches that were essentially transformed into flat roads from all the sediment buildup. Some of the riparian canopy burned right down to the creek.
Then came 32 inches of rain over the last nine months, scouring out and moving sediment, creating deeper pools. Dagit said they recently found newt egg masses for the first time in years, as well as a few adult newts and many frogs. Plants that provide cover are starting to recover.
She provided photos comparing certain pools last year and this year, some dramatically transformed. In September 2025, the Shrine Pool could have been an overgrown hiking trail. This April, it was filled with shallow water.

The Shrine Pool in September 2025, left, and the same location in April 2026, right, with RCDSMM’s Isaac Yelchin donning a wetsuit.
(RCDSMM Stream Team)
Topanga Creek is home to another endangered fish, the small but hardy northern tidewater goby, often described as cute. Not long before the trout operation, Dagit led a rescue of hundreds of these fish too. Many were repatriated to the lagoon at the mouth of the creek in a moving ceremony last June.
There’s still the matter of what to do with the trout that were moved to Santa Barbara County last year. Evans would like to bring them home to the Santa Monicas at some point, but isn’t sure if it will happen. On one hand, they could bolster the small, genetically isolated surviving population. On the other, they might inadvertently bring in a disease or bacteria. There is some time to decide. Evans estimates the creek still needs to recover for two to three more years.
For now, the fish are functioning fine in their adopted creek. Experts worried the trauma wrought by the move would disrupt their spawning process, but they had babies that spring. This year, they spawned again.
Science
Pacifica pier cracks, another coastal casualty as seas continue to rise

The Pacifica Municipal Pier was shut down and taped off Thursday after city workers noticed cracks running through the landmark structure and concrete chunks falling into the ocean.
It’s just one of many coastal California structures that have recently crumbled under pressure from a rising and relentless ocean.
Officials from the small, beach city south of San Francisco said the pier was closed due to “cracking, separation, and displacement of the concrete walkway and structural elements.”
It will stay closed while structural engineers asses its safety.
Photos taken by city employees show a wide crack that runs from top to bottom and across the structure as well. Other photos show a large horizontal crack under the foundation of a small restaurant on the pier, the Chit Chat Cafe.
The cafe was also shut down.
This is not the first time the 53-year-old pier has shown signs of stress. In 2021, part of it was shut down after handrails along the edge collapsed. And in 2023, after a series of storms pummeled the Central California coast, damaging parts of the pier, the structure was partially closed for more than year.
Those same storms caused extensive damage in Aptos and Capitola, 70 miles south, where piers and waterfront infrastructure were swept away or damaged.
In 2024, a 150- to 180- foot section of the Santa Cruz wharf was ripped off by powerful waves.
At least 10 of the state’s dozens of coastal public piers were closed for part or all of 2024 due to structural damage sustained in winter storms since 2022. At least five others have longer-term upgrades planned to address structural issues.
“These things are costly to maintain,” said Zach Plopper, senior environmental director at Surfrider. “They are a part of our California coastal culture in many ways, but we’re going to need to reckon with, one, the state that they’re in, and two, the continuous and worsening threats they’re going to experience,”
He said most of the piers were constructed in the early 1900s, and they weren’t built to withstand decades of rough seas, storms and rising sea level.
“With this incoming El Niño, which is forecasted to be significant, and this marine heat wave we’re in the midst of, we’re kind of in uncharted waters as far as what this winter could bring in terms of storms and swells to the California coast, and we’re likely going to see a lot more damage,” he said. “Not just piers, but roads and other coastal infrastructure up and down the state.”
There was no storm in Pacifica earlier this week, so no single event could be blamed for the destruction.
However, a 2025 report from an outside engineering firm, GHD, found that several sections of the pier were in “poor” or “serious” condition, and they recommended closure before anticipated storms or events that could “subject the piles to high winds, swells and large waves.”
The firm found several areas of the pier where concrete was missing and rebar was exposed and corroding.
“The pier has continued to experience high winds and large waves in a harsh marine environment,” the engineers wrote in the report, noting that continuous exposure to seawater or marine spray was “detrimental” to the structure.
A 2023 city report estimated it would cost $19 million to repair.
That same year, a state law was enacted to require local governments along the California coast to plan for sea level rise in the coming decades.
Sea level has risen some 8 inches, on average, along the coast in the past 150 years, Plopper said, and researchers anticipate another foot in the next 25 years.
“We’re going to see profound shifts on our coastline, none that we have ever experienced before, and building static structures on the coast just doesn’t work all that well,” he said. “We’re going to have to make some really hard decisions.”
-

 Technology6 minutes ago
Technology6 minutes agoAndroid fake call detection warns you about scams
-

 Business9 minutes ago
Business9 minutes agoPrimm is a spooky shell of its former self. But the gambling oasis may have found a savior
-

 Entertainment14 minutes ago
Entertainment14 minutes agoHiker who died in Runyon Canyon ID’d as Hollywood screenwriter, pal of Caitlyn Jenner
-

 Politics24 minutes ago
Politics24 minutes agoSupporters of L.A. County healthcare sales tax declare victory
-

 Sports36 minutes ago
Sports36 minutes agoUSC freshman linebacker Talanoa Ili joins lawsuit seeking to upend new NIL system
-

 World44 minutes ago
World44 minutes agoWho has the most and fewest judges in the EU?
-

 News1 hour ago
News1 hour agoIn Nevada, Trump’s policies are making things tough for Republican Gov. Joe Lombardo
-

 New York2 hours ago
New York2 hours agoThis Parking Spot Is Free. Should It Be?