Science
He reported a possible H5N1 outbreak in dairy cows. It took officials weeks to respond

The virus has — so far — caused only minimal illness among humans, yet has spread rapidly among birds, sea mammals and other species with devastating effect.
Although U.S. health officers have repeatedly assured Americans that H5N1 bird flu poses little risk to their well-being, some experts have become increasingly critical of what they see as the government’s failure to aggressively monitor the spread of virus among cattle and other farm animals. The virus has been reported in 145 dairy herds across 12 states, but critics say this is likely an underestimate.
They point to stories they have heard anecdotally from physicians and veterinarians in farming communities about mystery illnesses and cover-ups. And they point to perplexing “hits” of H5N1 in municipal wastewater far from any infected dairy herds.
“I think our government officials are are not doing the thorough investigation they should be doing,” said Rick Bright, a virologist and the former head of the U.S. Biomedical Advanced Research and Development Authority. “I think they are continually minimizing this outbreak and this virus.”
The worry among some experts is that H5N1-infected farm animals could serve as “mixing vessels” for new viral strains that could more easily infect people. They point to research released this week showing that the virus has receptors for both birds and humans. And they note that up to 75% of human infectious diseases are derived from pathogens that originated from animals.
Now, amid this heated debate over viral monitoring, a raw milk dairy farmer and longtime critic of the Food and Drug Administration has accused the government of ignoring his tip about a suspected H5N1 outbreak among a herd of dairy cows in early May.
Cows leave a dairy barn after milking.
(Tomas Ovalle/For The Times)
Although it remains unclear whether an outbreak actually occurred, neither federal nor state officials investigated the matter for weeks. Only after inquiries by The Times did officials announce Tuesday that they would look into the report.
The delayed response, some experts say, suggests a disturbing lack of oversight on the part of government officials.
“I think that once everybody decided it wasn’t going to kill people and pasteurized milk and herds could get over it, then all that was left was to take these stopgap measures — voluntary reporting, voluntary testing, testing when going across state lines — that don’t look anything like a really serious effort to go ahead and stamp it out,” said Michael Payne, a researcher and outreach coordinator at the Western Institute for Food Safety and Security at UC Davis.
The outbreak claim comes from Mark McAfee, owner of Raw Farms, a raw milk dairy producer with herds in Fresno and Hanford. On June 17, McAfee — who is also the president of the Raw Milk Institute, an advocacy group — emailed the FDA’s acting director, Donald Prater, to say that he’d been told a raw milk dairy herd had been infected and that people had probably consumed the contaminated milk.
According to McAfee’s email, which was shared with The Times, a subset of a farmer’s cows were suffering yellowish, runny diarrhea; low milk production; thick, yellowish colostrum; and general weakness. The farmer told McAfee he had separated the sick cows — about 10% of his herd — and discontinued milking them.

Mark McAfee walks by cows feeding at his raw milk dairy.
(Tomas Ovalle/For The Times)
“The farmer reported that for certain, humans had consumed the raw milk at some level,” McAfee wrote to Prater, adding that the farmer’s veterinarian “told the farmer to not report anything to anyone” because the virus would pass and “he did not want the FDA to swoop in and cause a media frenzy.”
McAfee said he fields lots of questions and calls from raw milk farmers around the nation. Because he’s president and founder of the Raw Milk Institute — and the largest producer of raw milk in the country — his advice and counsel is often sought by smaller dairy farmers.
Within 90 minutes of sending the email, Prater responded that he appreciated the time McAfee had taken to write the note and “for sharing these perspectives.” He then added that he and his agency would “take note of the points you raised and come back to you if we have any questions.”
According to McAfee, the FDA did not follow up with him. The state of New Mexico, where McAfee says the herd was infected, was made aware of the tip only last week, after the Times inquired.
The U.S. Department of Agriculture and the Centers for Disease Control and Prevention would not comment for the record on the matter, referring questions to the state.
Critics say whether the outbreak occurred or not, the lack of an immediate, or even timely, response underscores the absence of urgency and leadership in the face of a potential health threat.
“If you turn your back on this virus, you’re kind of inviting it in to bite you in the ass,” said Bill Hanage, associate professor of epidemiology and co-director of the Center for Communicable Disease Dynamics at Harvard University’s T.H. Chan School of Public Health.
Bright, the virologist, said the delay was a problem.
1
2

3

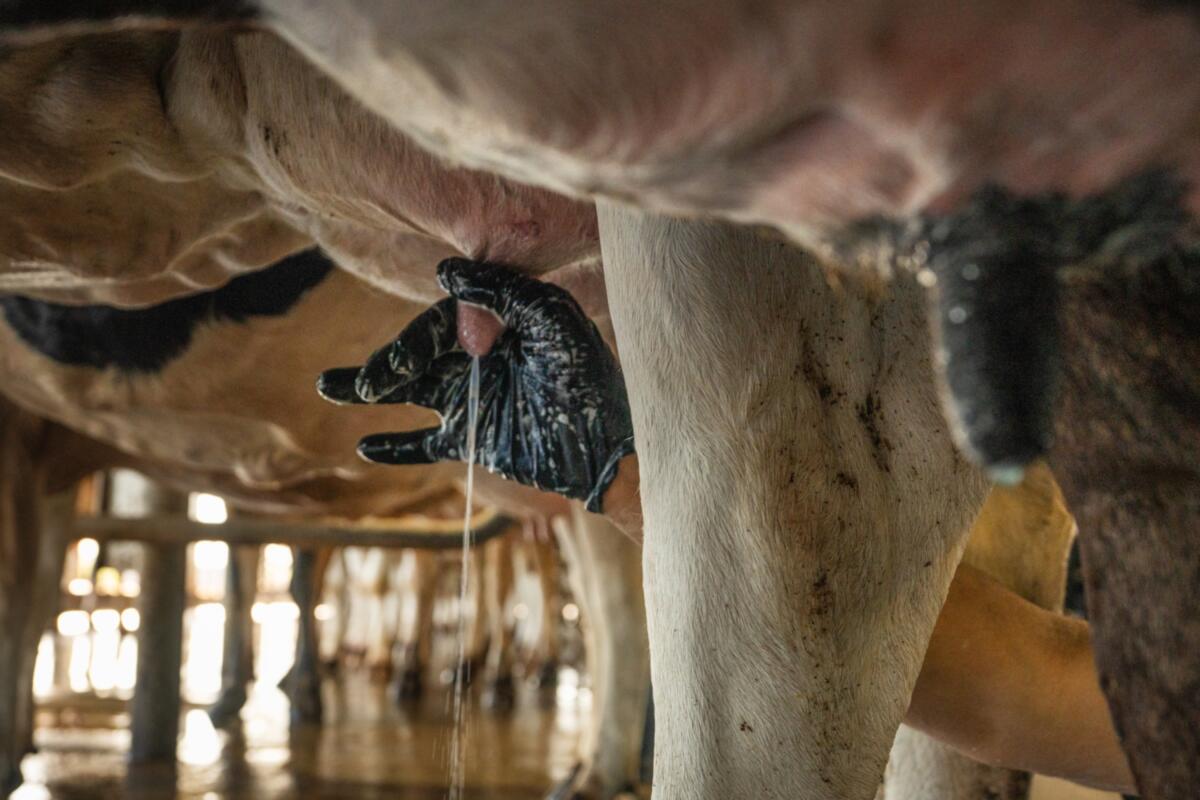
1. Carlos Rodriguez squeezes a cows teat to check the quality of the milk coming out of it. 2. Alvaro Hernandez hangs a milking cluster high to avoid contamination after a cow has been milked. 3. Mark McAfee checks bacteria levels in his raw milk every day and spends over $300,000 on testing. (Tomas Ovalle/For The Times)
“This is the stuff that drives me crazy,” Bright said. “I always tell people, it’s not necessarily the data that we have in front of us that’s most concerning. It is what’s being hid from us that’s most concerning.”
Farmers do not have to let government officials test their cattle, he said, which makes it hard to verify weeks after the fact whether an outbreak had occurred. If a dairy farmer allowed it, researchers could check for H5N1 antibodies in the blood.
“I really don’t think they want to know,” he said of the U.S. government, and the FDA in particular.
To be sure, the FDA and McAfee’s Raw Milk Institute have had a long, contentious history.
“To be quite frank, your source, Raw Milk Institute, are known advocates for repeatedly amplifying what they say is a lack of evidence that drinking raw milk with H5N1 is bad for you,” said Janell Goodwin, an FDA spokeswoman.
Indeed, McAfee said he reported the outbreak because he believed it showed that unpasteurized, yet infected raw milk was not a threat.
“No one got sick from that outbreak,” he insisted.

Mark McAfee, a raw milk dairy farmer and longtime critic of the FDA, has accused officials of ignoring his tip about a possible H5N1 outbreak among dairy cows.
(Tomas Ovalle/For The Times)
But epidemiologists The Times spoke with expressed skepticism on this point, suggesting that maybe nobody had “reported” being sick, noting that many dairy workers are migrants who may not relish a government visit. And they pointed to experimental and observational studies of barn cats that consumed H5N1 contaminated raw milk and “had about a 50% mortality rate and really unpleasant symptoms,” said Hanage, the Harvard professor.
Drinking raw milk is “something that is a risk that we would rather people didn’t take just for their own sake,” he said.
McAfee noted that he has received a certificate of good standing by California’s Department of Food and Agriculture for voluntarily testing his cows’ milk for H5N1. A spokesman for the agency confirmed that as of July 1, the farm’s milk was clear of the virus.

Science
Santa Monica Mountains’ last steelhead trout survived the Palisades fire — and even had babies

Scientists feared the Santa Monica Mountains’ last remaining steelhead trout were dead, smothered by debris flows unleashed by the Palisades fire.
But the endangered fish surprised them: A team of biologists recently spotted 30 of the rare trout — and 21 babies — in Topanga Creek.
“There was a lot of happy dancing in the creek,” said Rosi Dagit, principal conservation biologist for the Resource Conservation District of the Santa Monica Mountains, which works with public and private landowners to conserve natural resources.
That’s because the steelhead here are endangered, at both the state and federal levels. Once, they swam in most streams of the Santa Monicas, but their numbers plummeted amid overfishing and coastal development. Increasingly frequent wildfire has further stressed their habitat. Topanga Creek, a biodiversity hot spot, is home to their last known population in the mountains that stretch from the Hollywood Hills to Point Mugu in Ventura County.
The trout that were spotted, including this one, are part of a distinct Southern California population that’s listed as endangered at the state and federal levels.
(RCDSMM Stream Team)
The California Department of Fish and Wildlife spearheaded a complex mission to rescue trout threatened by the Palisades fire that sparked in January 2025.
Time was of the essence. The fire hadn’t yet been fully contained. But rain was on the way, which would sweep massive amounts of sediment from the denuded hillsides into the water. Fish are often killed this way.
Crews stunned the fish with electricity, scooped them up in buckets, trucked them to a hatchery and ultimately moved them to Arroyo Hondo Creek in Santa Barbara County.
Within days, Topanga Creek was choked with mud. Some assumed the fish left behind were goners.
But in March, the conservation district’s team found four. The following month, when water conditions were clearer, they saw more.
“These fish continue to amaze me,” said Kyle Evans, environmental program manager for the state Department of Fish and Wildlife, who had seen the damage to the creek. “I had seen populations get wiped out in similar situations. So when I heard, I was thrilled.”
Evans surmises the fish that survived were in an area of the creek where less charred material and sediment were swept in.
“These fish likely hunkered down, were hiding under some rocks or places to try to get away from the main concentration of flow,” he said. “And luckily they weren’t buried.”
The ones that were spotted were fairly small, around 6 to 14 inches. Rainbow trout and steelhead trout are the same species, but with different lifestyles. If the fish remain in freshwater, they’ll be considered rainbows. However, they can migrate to the ocean and become steelhead, where they typically grow larger before returning to their natal waters to spawn.
Topanga Creek hasn’t fully recovered from the damage it sustained, but scientists say it’s looking better. Surveys last year were “so depressing,” Dagit said, with very few animals, and stretches that were essentially transformed into flat roads from all the sediment buildup. Some of the riparian canopy burned right down to the creek.
Then came 32 inches of rain over the last nine months, scouring out and moving sediment, creating deeper pools. Dagit said they recently found newt egg masses for the first time in years, as well as a few adult newts and many frogs. Plants that provide cover are starting to recover.
She provided photos comparing certain pools last year and this year, some dramatically transformed. In September 2025, the Shrine Pool could have been an overgrown hiking trail. This April, it was filled with shallow water.

The Shrine Pool in September 2025, left, and the same location in April 2026, right, with RCDSMM’s Isaac Yelchin donning a wetsuit.
(RCDSMM Stream Team)
Topanga Creek is home to another endangered fish, the small but hardy northern tidewater goby, often described as cute. Not long before the trout operation, Dagit led a rescue of hundreds of these fish too. Many were repatriated to the lagoon at the mouth of the creek in a moving ceremony last June.
There’s still the matter of what to do with the trout that were moved to Santa Barbara County last year. Evans would like to bring them home to the Santa Monicas at some point, but isn’t sure if it will happen. On one hand, they could bolster the small, genetically isolated surviving population. On the other, they might inadvertently bring in a disease or bacteria. There is some time to decide. Evans estimates the creek still needs to recover for two to three more years.
For now, the fish are functioning fine in their adopted creek. Experts worried the trauma wrought by the move would disrupt their spawning process, but they had babies that spring. This year, they spawned again.
Science
Pacifica pier cracks, another coastal casualty as seas continue to rise

The Pacifica Municipal Pier was shut down and taped off Thursday after city workers noticed cracks running through the landmark structure and concrete chunks falling into the ocean.
It’s just one of many coastal California structures that have recently crumbled under pressure from a rising and relentless ocean.
Officials from the small, beach city south of San Francisco said the pier was closed due to “cracking, separation, and displacement of the concrete walkway and structural elements.”
It will stay closed while structural engineers asses its safety.
Photos taken by city employees show a wide crack that runs from top to bottom and across the structure as well. Other photos show a large horizontal crack under the foundation of a small restaurant on the pier, the Chit Chat Cafe.
The cafe was also shut down.
This is not the first time the 53-year-old pier has shown signs of stress. In 2021, part of it was shut down after handrails along the edge collapsed. And in 2023, after a series of storms pummeled the Central California coast, damaging parts of the pier, the structure was partially closed for more than year.
Those same storms caused extensive damage in Aptos and Capitola, 70 miles south, where piers and waterfront infrastructure were swept away or damaged.
In 2024, a 150- to 180- foot section of the Santa Cruz wharf was ripped off by powerful waves.
At least 10 of the state’s dozens of coastal public piers were closed for part or all of 2024 due to structural damage sustained in winter storms since 2022. At least five others have longer-term upgrades planned to address structural issues.
“These things are costly to maintain,” said Zach Plopper, senior environmental director at Surfrider. “They are a part of our California coastal culture in many ways, but we’re going to need to reckon with, one, the state that they’re in, and two, the continuous and worsening threats they’re going to experience,”
He said most of the piers were constructed in the early 1900s, and they weren’t built to withstand decades of rough seas, storms and rising sea level.
“With this incoming El Niño, which is forecasted to be significant, and this marine heat wave we’re in the midst of, we’re kind of in uncharted waters as far as what this winter could bring in terms of storms and swells to the California coast, and we’re likely going to see a lot more damage,” he said. “Not just piers, but roads and other coastal infrastructure up and down the state.”
There was no storm in Pacifica earlier this week, so no single event could be blamed for the destruction.
However, a 2025 report from an outside engineering firm, GHD, found that several sections of the pier were in “poor” or “serious” condition, and they recommended closure before anticipated storms or events that could “subject the piles to high winds, swells and large waves.”
The firm found several areas of the pier where concrete was missing and rebar was exposed and corroding.
“The pier has continued to experience high winds and large waves in a harsh marine environment,” the engineers wrote in the report, noting that continuous exposure to seawater or marine spray was “detrimental” to the structure.
A 2023 city report estimated it would cost $19 million to repair.
That same year, a state law was enacted to require local governments along the California coast to plan for sea level rise in the coming decades.
Sea level has risen some 8 inches, on average, along the coast in the past 150 years, Plopper said, and researchers anticipate another foot in the next 25 years.
“We’re going to see profound shifts on our coastline, none that we have ever experienced before, and building static structures on the coast just doesn’t work all that well,” he said. “We’re going to have to make some really hard decisions.”
Science
L.A. region begins the year with the smoggiest first 5 months in a decade

The first five months of 2026 in Southern California have been the smoggiest — with the highest number of unhealtful air days — in more than a decade, according to statewide air monitoring.
So far this year, the South Coast air basin, which includes Los Angeles, Orange, Riverside and San Bernardino counties, has seen 39 days when the concentration of lung-irritating ozone (commonly known as smog) exceeded the federal standard, according to preliminary state air quality data.
That’s even worse than the infamously hot and hazy 2017, when Greater Los Angeles had 36 unhealthful air days by June 4 and ultimately saw 145.
Many of the roughly 18 million people who live in the air basin have been subjected to unhealthful levels of ozone, a highly corrosive gas that triggers asthma attacks and a wide range of respiratory illnesses. This has taken many by surprise since successive days of smog more commonly happen in summer, when heat waves and intense sunlight convert man-made pollution into ozone.
“If we have this many violations by this time, this could be a really awful year for air quality,” said Adrian Martinez, director of Earthjustice’s Right to Zero campaign, an initiative calling for the transition away from fossil fuels. “We’re already the worst place in the country for summertime smog pollution. So it could be one of the worst years in one of the worst places in the country.”
The pollution has been especially severe in valleys. On April 18, an air monitor in Reseda in the San Fernando Valley measured the second highest spike in hourly ozone levels in the last decade.
Greater Los Angeles has seen more high-smog days so far in 2026 than any other year in the past decade.
(Courtesy of South Coast Air Quality Management District)
The South Coast Air Quality Management District says the high ozone levels are due to early heat waves. Officials said they were not aware of any increase in the pollutants — most of them from different kinds of exhaust — that lead to ozone formation.
Local temperatures have been well above normal, climbing into the mid-80s and high 90s between January and April, breaking several daily high temperature records, according to the National Weather Service.
March in particular was the warmest on record in California. Riverside had an unprecedented 13 days of temperatures above 90 degrees, the weather service said.
“It was really that heat wave — conditions we typically see in July or August, we saw them in March,” said Sarah Rees, deputy executive officer of the air district. “That put us ahead of the curve in terms of how much ozone we got.”
Air district officials urged residents to monitor pollution levels on the agency’s website and mobile app, and spend only limited time outdoors when smog levels are high.
“People generally know when there’s a wildfire, because you see the smoke and smell it,” said Scott Epstein, the air district’s manager of planning and rules. “Then, it’s like, I’ve got to take precautions. Ozone, you can’t really tell.”
Southern California has been particularly susceptible to smog formation because of its millions of gas-powered cars releasing tons of tailpipe emissions each day. The region’s sunshine acts as a catalyst for smog formation. Then the mountains trap this pollution over densely populated communities.
For nearly half a century, state and local air regulators have made rules designed to alleviate this pollution, enacting the nation’s first tailpipe emission standards in 1966 and requiring catalytic converters in 1975.
Smog-forming pollution has been dramatically reduced over the last two decades, but the region still does not meet federal air quality standards for ozone.
At an air district meeting Friday in Diamond Bar, the governing board held a moment of silence for William Burke, a former longtime chair. During his tenure, the agency enacted nearly 270 rules that are credited with reducing smog-forming pollution by hundreds of tons per day. Burke, who also founded the Los Angeles Marathon, died in May at 87.
“Those are just emission reductions,” air district Chair Michael Cacciotti said at the Friday meeting. “But what it doesn’t tell you is how many kids, families, seniors were prevented from going to the hospital from an asthma attack, didn’t get cancer or other respiratory problems.”
Several residents from the Inland Empire, which suffers some of the worst smog pollution, expressed their appreciation for the air district’s efforts. But they also stressed the need for more progress.
“I’m old enough to remember growing up in the ‘70s and ‘80s … and not being able to see the mountains for weeks and months at a time,” said Erik Morden, one of several residents who spoke at the meeting.” I know things have improved, and I want to thank all of you for all the hard work that you’re doing. But there’s a lot of invisible stuff that you don’t see, that’s still out there — a lot of particulates in the ozone and chemicals that are causing a lot of problems.”
Martinez, the Earthjustice attorney, said the abnormally early outbreak of smog should be a wake-up call to government regulators that there’s work to be done, including offering more incentives to help residents and businesses transition to zero-emission appliances.
“We shouldn’t over-complicate it. We’ve got a lot of heat, we’ve got a lot of pollution,” Martinez said. “Our contention is, this agency can’t control the weather. But the one thing it can control is the pollution.”
-

 Fitness2 minutes ago
Fitness2 minutes agoI Ran 5K Every Day for 28 Days – Here’s What it Did to My Body, My Fitness and My Strength
-

 Movie Reviews14 minutes ago
Movie Reviews14 minutes ago‘Office Romance’ movie review: Jennifer Lopez and Brett Goldstein fail to prop up this confused, dreary rom-com
-
World22 minutes ago
A government-commissioned study found drinking risks. US guidelines didn’t feature its findings
-

 Lifestyle1 hour ago
Lifestyle1 hour ago‘Office Romance’ stars J.Lo as a CEO with a bad case of Brett Goldstein : Pop Culture Happy Hour
-

 Technology1 hour ago
Technology1 hour agoApple dials down Liquid Glass, and the Mac looks way better for it
-

 World1 hour ago
World1 hour agoUS adversaries China, North Korea strengthening ties as Xi, Kim set to begin talks
-

 Politics1 hour ago
Politics1 hour agoTrump’s SAVE America Act shows signs of life in the Senate despite Republican revolt
-

 Health1 hour ago
Health1 hour agoWoman with advanced Alzheimer’s regained speech and memories after taking magic mushrooms