Science
COVID and bird flu are rising. Here's how to keep yourself safe
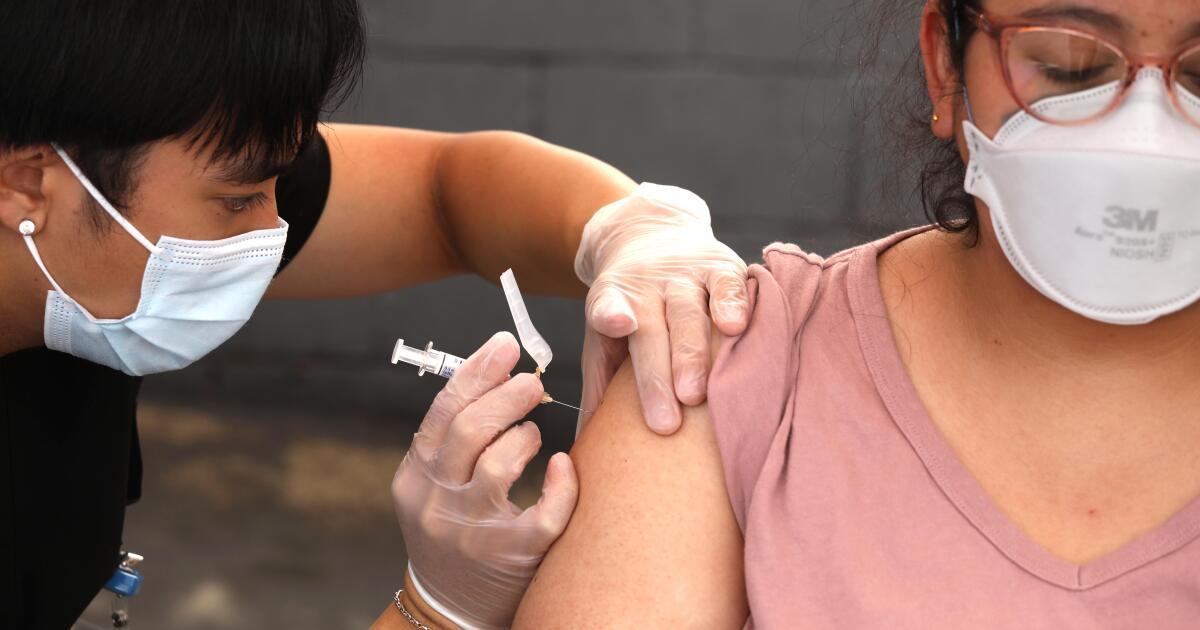
With California’s COVID surge at very high levels, doctors are urging people who are experiencing respiratory symptoms to test themselves or see a medical professional who can check on their illness.
This is the worst COVID summer infection spike in California since 2022, according to wastewater data. There are a number of possible culprits for the surge. A series of punishing heat waves and smoke from devastating wildfires have kept many Californians indoors, where the disease can more easily spread. Most adults are also well removed from their last brush with the coronavirus, or their last vaccine dose — meaning they’re more vulnerable to infection.
But changes in the virus have also widened the scope of the surge.
Of particular concern is the rise of a hyperinfectious subvariant known as KP.3.1.1, which is so contagious that even people who have eluded infection throughout the pandemic are getting sick.
“This is a very large surge that we are seeing currently. This is starting to rival, really, what we saw this past winter,” said Dr. Elizabeth Hudson, regional chief of infectious diseases at Kaiser Permanente Southern California.
Coronavirus levels in Los Angeles County wastewater are continuing to rise, according to the most recently available data. And viral levels in California wastewater are at “very high” levels as defined by the U.S. Centers for Disease Control and Prevention.
Coronavirus levels in the state’s wastewater were down 3% when comparing the week that ended Aug. 10 with the prior week, a possible indication that levels are cresting — although it’s also possible that coronavirus levels will increase again. Seasonal viral levels in sewage are expected to peak at some point, but it won’t be clear until a few weeks of consistent declines are observed.
Here are some things that experts say you can do to keep yourself safe:
Get tested
Doctors are urging people dealing with respiratory illness symptoms — including healthcare providers — to seek testing.
Dr. Abraar Karan, an infectious diseases expert and epidemiologist at Stanford University, said confirmation of a COVID-19 diagnosis would help a patient get a Paxlovid prescription to help treat the illness, while confirmation of another illness, like the flu, could help a patient get a drug more targeted toward that ailment.
An initial negative test does not mean you don’t have COVID; doctors suggest testing for as long as five days after the onset of symptoms to determine whether a test turns positive.
More consistent testing at medical facilities also could help detection of unusual strains that epidemiologists want to track, such as bird flu.
Bird flu has attracted attention recently because of outbreaks in poultry and dairy cows, and there have been several recent human cases among dairy and poultry workers in the U.S., according to the CDC.
The rise of bird flu
Recent human cases of H5N1 bird flu have resulted in primarily mild symptoms, including conjunctivitis, also known as pink eye, Karan said.
But one reason doctors are closely monitoring the situation is that, in the decades in which we’ve been aware of bird flu infecting humans, some H5N1 strains have resulted in significant mortality rates.
According to the CDC, human infections with H5N1 virus, which have been reported in 23 countries since 1997, have resulted in severe pneumonia and death in about 50% of cases.
Now that we know bird flu has infected cows, and there’s cow-to-human transmission, that poses a potential problem.
“Cow udders have receptors in common with birds, and they also have receptors in common with humans, where these viruses bind,” Karan said.
“Now, with human flu season coming, you have the risk of what’s called viral reassortment, where a host can get infected with both bird flu and human flu at the same time, and those flus now start swapping genetic material,” Karan said. “This is kind of how swine flu happened [in 2009]. So this is where we’re really worried. It’s like a ticking time bomb of human flu season around the corner, and yet we still have this uncontrolled spread of bird flu in cows.”
Bird flu hasn’t resulted in sustained human-to-human transmission, nor caused a pandemic in humans, in recent times.
“But it’s one of those pathogens that’s high risk of mutating to a point of increasing transmissibility. And the pathogen has had high virulence based on historical cases. … It’s the risk of where it could go,” Karan said.
Tracking the spread
This illustrates why it can be important for patients to get tested. If a test shows that a person has the flu, subsequent screening — including genetic subtyping — could eventually determine whether it is bird flu. And that could help epidemiologists figure out how the bird flu may have spread and help doctors determine the best course of treatment.
Even if a case of bird flu results in mild symptoms, it’s important to diagnose it, Karan said, so the virus sample can be genetically analyzed and scientists can track where it jumped from animal to human, and potentially more aggressively treat the patient with antivirals.
“But imagine — that only happens if I even test that patient for flu at all,” Karan said.
Where bird flu stands in the U.S.
Since 2022, according to the CDC, there have been 14 reported human cases of H5 bird flu in the U.S., 13 of which have been reported since March 24. Of the 14, nine have been confirmed as H5N1.
Of the 14 cases of bird flu in humans, 10 followed exposure to poultry, and the remainder followed exposure to cows. All of the reported human cases have occurred in three states: Colorado, Michigan and Texas.
Nationally, there are 48 states with bird flu outbreaks in poultry and 13 with outbreaks in dairy cows.
Since 2022, more than 100 million birds in the U.S. have been reported to have been infected with bird flu, including commercial poultry, backyard or hobbyist flocks and wild aquatic birds; it’s the first detection of this type of flu virus in the U.S. since 2016.
Bird flu has been detected in wild birds in most counties of California, including all of Southern California and the San Francisco Bay Area, and most of the Central Valley.
Bird flu outbreaks — those involving commercial poultry facilities or backyard poultry and hobbyist bird flocks — in California have been reported in just one county in Southern California: San Diego County. Bird flu outbreaks have occurred in a number of counties in Northern and Central California, including Sacramento, Contra Costa, Fresno, San Francisco, San Joaquin, Stanislaus, Sonoma, Monterey, Placer, Merced and Marin counties.
As for bird flu infecting dairy cows, 13 states have reported outbreaks — Idaho, Wyoming, Colorado, New Mexico, Texas, Oklahoma, Kansas, South Dakota, Minnesota, Iowa, Michigan, Ohio and North Carolina. In the last month, outbreaks infecting dairy cows have affected five states: Idaho, Colorado, Texas, South Dakota and Michigan.
In May, there was a detection of bird flu in a live bird market in San Francisco, according to the California Department of Food and Agriculture. State officials urged people to separate poultry from wild birds if possible.
“Because of the recent case in California poultry production and epidemiologic evidence that this strain was introduced by wild birds, we ask that California producers move their birds indoors through December 2024,” the California Department of Food and Agriculture said in June.
Protecting family and friends
The CDC earlier this year eased COVID isolation guidance, given that the health impacts of COVID-19 are lower than they once were, thanks to the availability of vaccines, anti-COVID medicines and increased population immunity.
There are fewer people being hospitalized and dying, and fewer reports of complications such as multi-inflammatory syndrome in children.
Still, doctors say it remains prudent to take common-sense steps to avoid illness and spreading the disease to others, given that COVID still causes significant health burdens that remain worse than the flu. Nationally, since the start of October, more than 49,000 people have been reported to have died of COVID; by contrast, flu has resulted in at least 25,000 fatalities over the same time period, according to federal estimates, which will be updated later this year.
While the prevalence of long COVID has been going down, long COVID can still be a risk any time someone gets COVID.
Doctors are urging everyone to get up to date on vaccinations — particularly if patients are at higher risk of severe complications from COVID-19. An updated COVID-19 vaccination formula is expected to become available in a matter of week, and the CDC is urging everyone 6 months and older to get one dose of the updated vaccine.
In California, just 37% of seniors 65 and older have received the last updated COVID-19 vaccine that first became available in September.
It’s especially important that older people get at least one updated dose. Of the patients he has seen recently who had serious COVID, UC San Francisco infectious diseases specialist Dr. Peter Chin-Hong said none of them had gotten an updated vaccine in the last year.
Avoid sick people. Some who are infected might pass off their symptoms simply as a cold or allergies when it could be the start of a COVID-19 illness.
Test if you’re sick, and test repeatedly if your first test shows up as negative.
An initial negative test doesn’t mean you don’t have COVID; doctors suggest testing for as long as five days after the onset of symptoms to check whether a test turns positive.
Consider taking a rapid COVID test once a day for three to five consecutive days after the onset of cough-and-cold symptoms, Hudson said.
Doing so can help a person take measures to later isolate themselves and limit spread of the illness to others.
Masks are much less common these days but can still be a handy tool to prevent infection. Wearing a mask on a crowded flight or in a crowded indoor venue where people nearby are coughing can help reduce the risk of infection.
The best mask is one that is well-fitted and that you find comfortable wearing. The most protective are N95 respirators, followed by KN95 respirators and KF94s. Surgical masks offer more protection than cloth masks.
Have a plan to ask for Paxlovid if you become ill. Paxlovid is an antiviral drug that, when taken by people at risk for severe COVID-19 who have mild-to-moderate illness, reduces the risk of hospitalization and death.
And if you get Paxlovid, make sure to take the full five-day course of treatment. Don’t stop taking the drug halfway through the dose.
There are also other anti-COVID medications that are available, such as remdesivir, which is given intravenously, and molnupiravir, which is given orally, like Paxlovid.
- Stay away from others while sick
The CDC recommends people stay home and away from others until at least 24 hours after their respiratory viral symptoms are getting better overall and they have not had a fever without using fever-reducing medicine such as Tylenol or Advil. Previously, the CDC suggested people with COVID isolate for at least five days and take additional precautions for a few more days.
In terms of deciding when symptoms are getting better, what’s most important is “the overall sense of feeling better and the ability to resume activities,” the CDC says. A lingering cough by itself can last beyond when someone is contagious, the CDC said.
But the CDC also advises added precautions for five additional days to avoid infecting others, such as wearing a mask, opening windows to improve air circulation, washing hands often, keeping one’s distance from others and continuing to test. It’s possible for infected people to be contagious even after they feel better.
The Los Angeles County Department of Public Health suggests infected people who have symptoms get a negative test result before leaving isolation. The agency also suggests those who are infected — regardless of whether they have symptoms — wear a mask around others for 10 days after they start feeling sick or, if asymptomatic, their first positive test result. However, they can remove their mask sooner if they have two sequential negative tests at least one day apart.
The agency suggests staying away from the elderly and immunocompromised people for 10 days after you start to feel sick, or, if asymptomatic, after their first positive test result.
If patients recover and then get sick again, they may have COVID rebound and need to stay home and isolate from non-infected people in their household.

Science
Diablo Canyon clears last California permit hurdle to keep running

Central Coast Water authorities approved waste discharge permits for Diablo Canyon nuclear plant Thursday, making it nearly certain it will remain running through 2030, and potentially through 2045.
The Pacific Gas & Electric-owned plant was originally supposed to shut down in 2025, but lawmakers extended that deadline by five years in 2022, fearing power shortages if a plant that provides about 9 percent the state’s electricity were to shut off.
In December, Diablo Canyon received a key permit from the California Coastal Commission through an agreement that involved PG&E giving up about 12,000 acres of nearby land for conservation in exchange for the loss of marine life caused by the plant’s operations.
Today’s 6-0 vote by the Central Coast Regional Water Board approved PG&E’s plans to limit discharges of pollutants into the water and continue to run its “once-through cooling system.” The cooling technology flushes ocean water through the plant to absorb heat and discharges it, killing what the Coastal Commission estimated to be two billion fish each year.
The board also granted the plant a certification under the Clean Water Act, the last state regulatory hurdle the facility needed to clear before the federal Nuclear Regulatory Commission (NRC) is allowed to renew its permit through 2045.
The new regional water board permit made several changes since the last one was issued in 1990. One was a first-time limit on the chemical tributyltin-10, a toxic, internationally-banned compound added to paint to prevent organisms from growing on ship hulls.
Additional changes stemmed from a 2025 Supreme Court ruling that said if pollutant permits like this one impose specific water quality requirements, they must also specify how to meet them.
The plant’s biggest water quality impact is the heated water it discharges into the ocean, and that part of the permit remains unchanged. Radioactive waste from the plant is regulated not by the state but by the NRC.
California state law only allows the plant to remain open to 2030, but some lawmakers and regulators have already expressed interest in another extension given growing electricity demand and the plant’s role in providing carbon-free power to the grid.
Some board members raised concerns about granting a certification that would allow the NRC to reauthorize the plant’s permits through 2045.
“There’s every reason to think the California entities responsible for making the decision about continuing operation, namely the California [Independent System Operator] and the Energy Commission, all of them are sort of leaning toward continuing to operate this facility,” said boardmember Dominic Roques. “I’d like us to be consistent with state law at least, and imply that we are consistent with ending operation at five years.”
Other board members noted that regulators could revisit the permits in five years or sooner if state and federal laws changes, and the board ultimately approved the permit.
Science
Deadly bird flu found in California elephant seals for the first time

The H5N1 bird flu virus that devastated South American elephant seal populations has been confirmed in seals at California’s Año Nuevo State Park, researchers from UC Davis and UC Santa Cruz announced Wednesday.
The virus has ravaged wild, commercial and domestic animals across the globe and was found last week in seven weaned pups. The confirmation came from the U.S. Department of Agriculture’s National Veterinary Services Laboratory in Ames, Iowa.
“This is exceptionally rapid detection of an outbreak in free-ranging marine mammals,” said Professor Christine Johnson, director of the Institute for Pandemic Insights at UC Davis’ Weill School of Veterinary Medicine. “We have most likely identified the very first cases here because of coordinated teams that have been on high alert with active surveillance for this disease for some time.”
Since last week, when researchers began noticing neurological and respoiratory signs of the disease in some animals, 30 seals have died, said Roxanne Beltran, a professor of ecology and evolutionary biology at UC Santa Cruz. Twenty-nine were weaned pups and the other was an adult male. The team has so far confirmed the virus in only seven of the dead pups.
Infected animals often have tremors convulsions, seizures and muscle weakness, Johnson said.
Beltran said teams from UC Santa Cruz, UC Davis and California State Parks monitor the animals 260 days of the year, “including every day from December 15 to March 1” when the animals typically come ashore to breed, give birth and nurse.
The concerning behavior and deaths were first noticed Feb. 19.
“This is one of the most well-studied elephant seal colonies on the planet,” she said. “We know the seals so well that it’s very obvious to us when something is abnormal. And so my team was out that morning and we observed abnormal behaviors in seals and increased mortality that we had not seen the day before in those exact same locations. So we were very confident that we caught the beginning of this outbreak.”
In late 2022, the virus decimated southern elephant seal populations in South America and several sub-Antarctic Islands. At some colonies in Argentina, 97% of pups died, while on South Georgia Island, researchers reported a 47% decline in breeding females between 2022 and 2024. Researchers believe tens of thousands of animals died.
More than 30,000 sea lions in Peru and Chile died between 2022 and 2024. In Argentina, roughly 1,300 sea lions and fur seals perished.
At the time, researchers were not sure why northern Pacific populations were not infected, but suspected previous or milder strains of the virus conferred some immunity.
The virus is better known in the U.S. for sweeping through the nation’s dairy herds, where it infected dozens of dairy workers, millions of cows and thousands of wild, feral and domestic mammals. It’s also been found in wild birds and killed millions of commercial chickens, geese and ducks.
Two Americans have died from the virus since 2024, and 71 have been infected. The vast majority were dairy or commercial poultry workers. One death was that of a Louisiana man who had underlying conditions and was believed to have been exposed via backyard poultry or wild birds.
Scientists at UC Santa Cruz and UC Davis increased their surveillance of the elephant seals in Año Nuevo in recent years. The catastrophic effect of the disease prompted worry that it would spread to California elephant seals, said Beltran, whose lab leads UC Santa Cruz’s northern elephant seal research program at Año Nuevo.
Johnson, the UC Davis researcher, said the team has been working with stranding networks across the Pacific region for several years — sampling the tissue of birds, elephant seals and other marine mammals. They have not seen the virus in other California marine mammals. Two previous outbreaks of bird flu in U.S. marine mammals occurred in Maine in 2022 and Washington in 2023, affecting gray and harbor seals.
The virus in the animals has not yet been fully sequenced, so it’s unclear how the animals were exposed.
“We think the transmission is actually from dead and dying sea birds” living among the sea lions, Johnson said. “But we’ll certainly be investigating if there’s any mammal-to-mammal transmission.”
Genetic sequencing from southern elephant seal populations in Argentina suggested that version of the virus had acquired mutations that allowed it to pass between mammals.
The H5N1 virus was first detected in geese in China in 1996. Since then it has spread across the globe, reaching North America in 2021. The only continent where it has not been detected is Oceania.
Año Nuevo State Park, just north of Santa Cruz, is home to a colony of some 5,000 elephant seals during the winter breeding season. About 1,350 seals were on the beach when the outbreak began. Other large California colonies are located at Piedras Blancas and Point Reyes National Sea Shore. Most of those animals — roughly 900 — are weaned pups.
It’s “important to keep this in context. So far, avian influenza has affected only a small proportion of the weaned at this time, and there are still thousands of apparently healthy animals in the population,” Beltran said in a press conference.
Public access to the park has been closed and guided elephant seal tours canceled.
Health and wildlife officials urge beachgoers to keep a safe distance from wildlife and keep dogs leashed because the virus is contagious.
Science
When slowing down can save a life: Training L.A. law enforcement to understand autism

Kate Movius moved among a roomful of Los Angeles County sheriff’s deputies, passing out a pop trivia quiz and paper prism glasses.
She told them to put on the vision-distorting glasses, and to write with their nondominant hand. As they filled out the tests, Movius moved about the City of Industry classroom pounding abruptly on tables. Then came the cowbell. An aide flashed the overhead lights on and off at random. The goal was to help the deputies understand the feeling of sensory overwhelm, which many autistic people experience when incoming stimulation exceeds their capacity to process.
“So what can you do to assist somebody, or de-escalate somebody, or get information from someone who suffers from a sensory disorder?” Movius asked the rattled crowd afterward. “We can minimize sensory input. … That might be the difference between them being able to stay calm and them taking off.”
Movius, founder of the consultancy Autism Interaction Solutions, is one of a growing number of people around the U.S. working to teach law enforcement agencies to recognize autistic behaviors and ensure that encounters between neurodevelopmentally disabled people and law enforcement end safely.
She and City of Industry Mayor Cory Moss later passed out bags filled with tools donated by the city to aid interactions: a pair of noise-damping headphones to decrease auditory input, a whiteboard, a set of communication cards with words and images to point to, fidget toys to calm and distract.
“The thing about autistic behavior when it comes to law enforcement is a lot of it may look suspicious, and a lot of it may feel very disrespectful,” said Movius, who is also the parent of an autistic 25-year-old man. Responding officers, she said, “are not coming in thinking, ‘Could this be a developmentally disabled person?’ I would love for them to have that in the back of their minds.”
A sheriff’s deputy reads a pamphlet on autism during the training program.
(Genaro Molina / Los Angeles Times)
Autism spectrum disorder is a developmental condition that manifests differently in nearly every person who has it. Symptoms cluster around difficulties in communication, social interaction and sensory processing.
An autistic person stopped by police might hold the officer’s gaze intensely or not look at them at all. They may repeat a phrase from a movie, repeat the officer’s question or temporarily lose their ability to speak. They might flee.
All are common involuntary responses for an autistic person in a stressful situation, which a sudden encounter with law enforcement almost invariably is. To someone unfamiliar with the condition, all could be mistaken for intoxication, defiance or guilt.
Autism rates in the U.S. have increased nearly fivefold since the Centers for Disease Control began tracking diagnoses in 2000, a rise experts attribute to broadening diagnostic criteria and better efforts to identify children who have the condition.
The CDC now estimates that 1 in 31 U.S. 8-year-olds is autistic. In California, the rate is closer to 1 in 22 children.
As diverse as the autistic population is, people across the spectrum are more likely to be stopped by law enforcement than neurotypical peers.
About 15% of all people in the U.S. ages 18 to 24 have been stopped by police at some point in their lives, according to federal data. While the government doesn’t track encounters for disabled people specifically, a separate study found that 20% of autistic people ages 21 to 25 have been stopped, often after a report or officer observation of a person behaving unusually.
Some of these encounters have ended in tragedy.
In 2021, Los Angeles County sheriff’s deputies shot and permanently paralyzed a deaf autistic man after family members called 911 for help getting him to a hospital.
Isaias Cervantes, 25, had become distressed about a shopping trip and started pushing his mother, his family’s attorney said at the time. He resisted as two deputies attempted to handcuff him and one of the deputies shot him, according to a county report.
In 2024, Ryan Gainer’s family called 911 for support when the 15-year-old became agitated. Responding San Bernardino County sheriff‘s deputies shot and killed him outside his Apple Valley home.
Last year, police in Pocatello, Idaho, shot Victor Perez, 17, through a chain-link fence after the nonspeaking teenager did not heed their shouted commands. He died from his injuries in April.

Sheriff’s deputies take a trivia quiz using their non-writing hands, while wearing vision-distorting glasses, as Kate Movius, standing left, and Industry Mayor Cory Moss, right, ring cowbells. The idea was to help them understand the sensory overwhelm some autistic people experience.
(Genaro Molina / Los Angeles Times)
As early as 2001, the FBI published a bulletin on police officers’ need to adjust their approach when interacting with autistic people.
“Officers should not interpret an autistic individual’s failure to respond to orders or questions as a lack of cooperation or as a reason for increased force,” the bulletin stated. “They also need to recognize that individuals with autism often confess to crimes that they did not commit or may respond to the last choice in a sequence presented in a question.”
But a review of multiple studies last year by Chapman University researchers found that while up to 60% of officers have been on a call involving an autistic person, only 5% to 40% had received any training on autism.
In response, universities, nonprofits and private consultants across the U.S. have developed curricula for law enforcement on how to recognize autistic behaviors and adapt accordingly.
The primary goal, Movius told deputies at November’s training session, is to slow interactions down to the greatest extent possible. Many autistic people require additional time to process auditory input and verbal responses, particularly in unfamiliar circumstances.
If at all possible, Movius said, wait 20 seconds for a response after asking a question. It may feel unnaturally long, she acknowledged. But every additional question or instruction fired in that time — what’s your name? Did you hear me? Look at me. What’s your name? — just decreases the likelihood that a person struggling to process will be able to respond at all.
Moss’ son, Brayden, then 17, was one of several teenagers and young adults with autism who spoke or wrote statements to be read to the deputies. The diversity of their speech patterns and physical mannerisms showed the breadth of the spectrum. Some were fluently verbal, while others communicated through signs and notes.
“This population is so diverse. It is so complicated. But if there’s anything that we can show [deputies] in here that will make them stop and think, ‘Hey, what if this is autism?’ … it is saving lives,” Moss said.

Mayor Cory Moss, left, and Kate Movius hug at the end of the training program last November. Movius started Autism Interaction Solutions after her son was born with profound autism.
(Genaro Molina / Los Angeles Times)
Some disability advocates cautioned that it takes more than isolated training sessions to ensure encounters end safely.
Judy Mark, co-founder and president of the nonprofit Disability Voices United, says she trained thousands of officers on safe autism interactions but stopped after Cervantes’ shooting. She now urges families concerned about an autistic child’s safety to call an ambulance rather than law enforcement.
“I have significant concern about these training sessions,” Mark said. “People get comfort from it, and the Sheriff’s Department can check the box.”
While not a panacea, supporters argue that a brief course is better than no preparation at all. Some years ago, Movius received a letter from a man whose profoundly autistic son slipped away as the family loaded their car at the beach. He opened the unlocked door of a police vehicle, climbed into the back and began to flail in distress.
Though surprised, the officer seated at the wheel de-escalated the situation and helped the young man find his family, the father wrote to Movius. He had just been to her training.
-

 World2 days ago
World2 days agoExclusive: DeepSeek withholds latest AI model from US chipmakers including Nvidia, sources say
-

 Massachusetts2 days ago
Massachusetts2 days agoMother and daughter injured in Taunton house explosion
-

 Montana1 week ago
Montana1 week ago2026 MHSA Montana Wrestling State Championship Brackets And Results – FloWrestling
-

 Oklahoma1 week ago
Oklahoma1 week agoWildfires rage in Oklahoma as thousands urged to evacuate a small city
-

 Louisiana4 days ago
Louisiana4 days agoWildfire near Gum Swamp Road in Livingston Parish now under control; more than 200 acres burned
-

 Technology6 days ago
Technology6 days agoYouTube TV billing scam emails are hitting inboxes
-

 Denver, CO2 days ago
Denver, CO2 days ago10 acres charred, 5 injured in Thornton grass fire, evacuation orders lifted
-

 Technology6 days ago
Technology6 days agoStellantis is in a crisis of its own making


















