Science
‘I just wanted to help.’ Father turns to 9-year-old son for lifesaving stem cell donation

The question came at dinner toward the end of June.
Anesthesiologist Nick Mondek, 48, was dying of acute myeloid leukemia, a cancer that affects blood-forming cells in the bone marrow. It was a serious topic to tackle with his then-9-year-old son, Stephen, as they ate bowls of pasta.
But Mondek needed a stem cell donor — and fast. So he asked his son to save his life.
The youngster agreed to be tested at Cedars-Sinai Medical Center to see if he could donate stem cells to his father.
The Rolling Hills Country Day fourth-grader, who dreams of becoming a doctor for a Major League Baseball team, had his own question first: “When do we go?”
In July, Stephen became what Cedars-Sinai Medical Center believes is its youngest known stem cell donor.
“I just wanted to help,” Stephen said.
His donation doesn’t just buy his father time but offers hope that Stephen’s stem cells will build a newer, stronger immune system that will help his father fight off blood cancer.
“I wanted him to do this as his own decision,” Mondek said. “I didn’t want him to feel forced. I didn’t want him to feel like he had to do it.”
Nick Mondek, a 48-year-old anesthesiologist, was dying of acute myeloid leukemia, a cancer that affects blood-forming cells in the bone marrow, and needed a stem donation to rebuild his immune system. His 9-year-old son Stephen stepped in to help.
(Courtesy of Cedars-Sinai)
Mondek’s journey from doctor to patient began in April 2022.
The then-45-year-old, an employee at the Martin Luther King Jr. Ambulatory Surgery Center, felt constantly fatigued with little appetite. Then one day he couldn’t turn his head. His resting heart rate jumped from a standard 60 beats per minute to a concerning, racing 100 bpm.
“Being a typical stubborn physician, I just kept writing it off,” he said. “I would take antibiotics, I would take ibuprofen, thinking it’s this, thinking it’s that, not even entertaining the fact that it could be cancer or even leukemia.”
Weeks of unrelenting symptoms led Mondek to take a simple Complete Blood Count, or CBC, test. He was hospitalized within hours of receiving the results.
Mondek first found aid in his brother, whose stem cell donation sent Mondek’s blood cancer into remission.
In April, however, the leukemia returned.
“We followed every clinical protocol, but the disease still managed to come back, so we had a new problem on our hands,” Dr. Ronald Paquette, clinical director of the Stem Cell and Bone Marrow Transplant Program at Cedars-Sinai Cancer, said in a news release. “How could we treat his cancer a second time around and have a better chance that it doesn’t return?”
Paquette and Mondek searched for genetic matches but found none in his family or in the National Bone Marrow Registry.

Stephen Montek with his dad, Nick; mom, Danielle Boyer, and brother, John.
(Courtesy of Cedars-Sinai)
That’s when Mondek opted for a curveball.
He recalled a friend successfully fought lymphoma after receiving a stem cell transplant from his 18-year-old son.
Paquette confirmed that Stephen, who turned 10 last month, was a possibility. Stephen was automatically a partial match since children receive half their DNA from each of their parents.
Further testing revealed that Stephen’s immune system was compatible with his father’s.
Mondek’s next conversation with his son was even more challenging than the initial lifesaving ask. He had to explain the ins and outs of the taxing preparation and procedure.
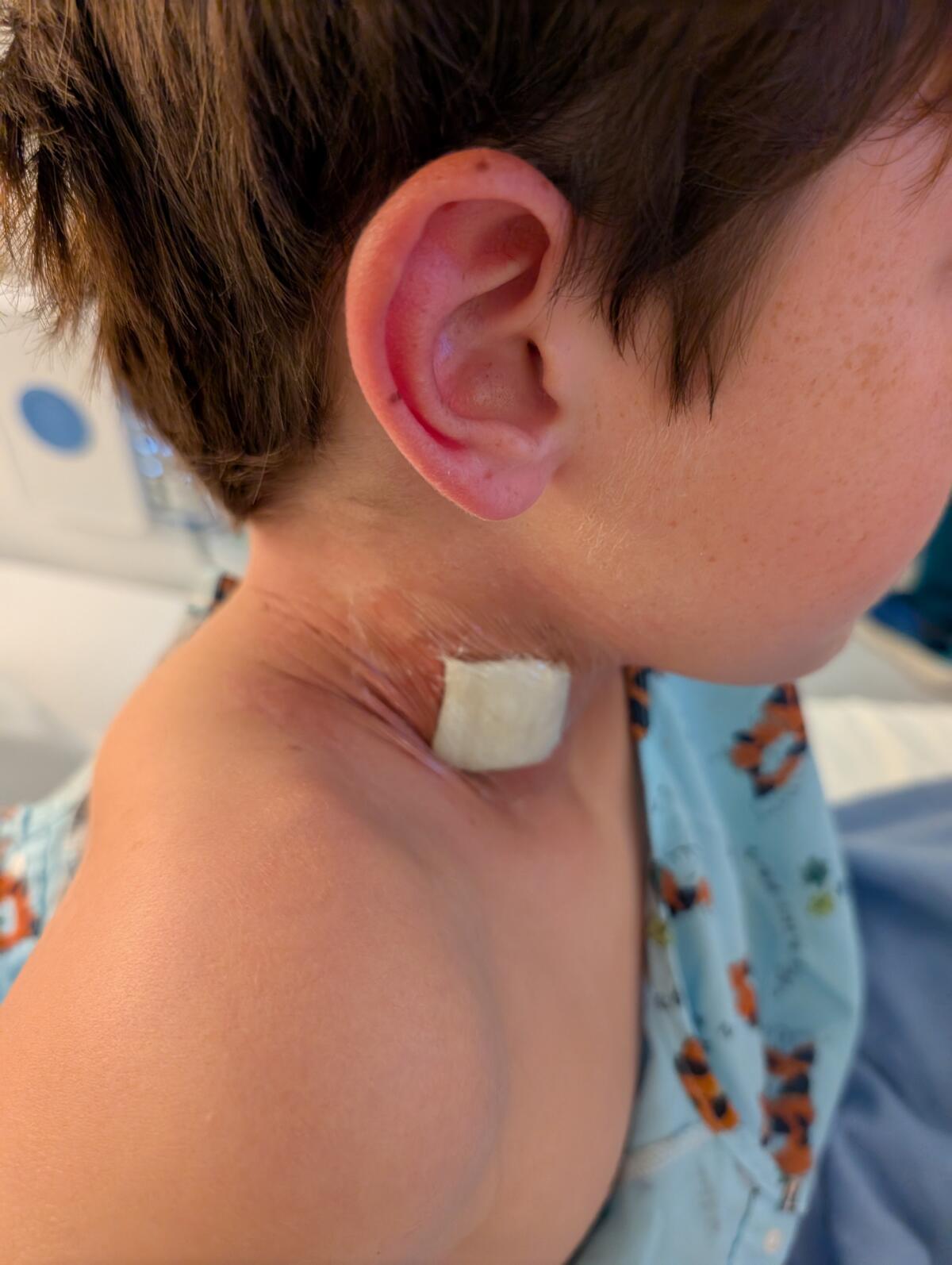
A bandage covers Stephen Mondek’s neck where a central line catheter was inserted for the stem cell donation.
(Courtesy of Cedars-Sinai)
“Every day, I tell patients about the risks and benefits before their procedures,” Mondek said. “And obviously they’re over 18 and they’re adults, so they can understand the pros and cons. So it’s like, how do I talk to a 9-year-old?”
Mondek explained to his son that there would be several weeks of pre-donation prep that included shots and blood exams. Although his son had reservations, he wasn’t concerned about anesthesia or procedures. He did have one worry.
“I didn’t want to miss any time playing baseball,” said Stephen, a Chicago Cubs fan and a catcher on the Rolling Hills Little League baseball team.
There were, however, special considerations because of Stephen’s age. A normal stem cell donation, for instance, is generally a non-surgical procedure in which blood is extracted from an arm through an IV.
Since Stephen’s veins are significantly smaller than an adult’s, doctors had to find another entry point.
Stephen arrived the day of his procedure at 7 a.m. He was placed at Cedars-Sinai Guerin Children’s pediatric ICU, given general anesthesia, intubated and put on a ventilator before a central line (catheter) was inserted into his neck, according to his father.
Stephen was then extubated and woken up, and then he rested for an hour before his blood was drained and spun through a centrifuge for six hours to separate out the stem cells.
“A donation from a child this young is very rare,” critical care pediatrician Dr. Hoyoung Chung said. “Stephen was very brave, and our team made sure everything went perfectly so that this young boy could help his father.”
Stephen went home that same day to his father, mother Danielle Boyer, and his younger brother, John.
His father’s recovery was not nearly as quick.
Mondek was admitted on July 23 and spent six days at Cedars receiving chemotherapy to suppress his immune system, making it less likely to reject Stephen’s cells.
Mondek passed an additional two weeks in the hospital to protect his fledgling and vulnerable immune system.
Paquette told Mondek that although the surgery was successful, it could take more than a year to determine if his new immune system, powered by his son’s cells, could defeat the leukemia. For now, he’d just have to wait.
On Aug. 16, Mondek was finally discharged from the hospital.
He drove straight to Stephen’s baseball game to catch his son’s final inning.

Science
What’s in a Name? For These Snails, Legal Protection

The sun had barely risen over the Pacific Ocean when a small motorboat carrying a team of Indigenous artisans and Mexican biologists dropped anchor in a rocky cove near Bahías de Huatulco.
Mauro Habacuc Avendaño Luis, one of the craftsmen, was the first to wade to shore. With an agility belying his age, he struck out over the boulders exposed by low tide. Crouching on a slippery ledge pounded by surf, he reached inside a crevice between two rocks. There, lodged among the urchins, was a snail with a knobby gray shell the size of a walnut. The sight might not dazzle tourists who travel here to see humpback whales, but for Mr. Avendaño, 85, these drab little mollusks represent a way of life.
Marine snails in the genus Plicopurpura are sacred to the Mixtec people of Pinotepa de Don Luis, a small town in southwestern Oaxaca. Men like Mr. Avendaño have been sustainably “milking” them for radiant purple dye for at least 1,500 years. The color suffuses Mixtec textiles and spiritual beliefs. Called tixinda, it symbolizes fertility and death, as well as mythic ties between lunar cycles, women and the sea.
The future of these traditions — and the fate of the snails — are uncertain. The mollusks are subject to intense poaching pressure despite federal protections intended to protect them. Fishermen break them (and the other mollusks they eat) open and sell the meat to local restaurants. Tourists who comb the beaches pluck snails off the rocks and toss them aside.
A severe earthquake in 2020 thrust formerly submerged parts of their habitat above sea level, fatally tossing other mollusks in the snail’s food web to the air, and making once inaccessible places more available to poachers.
Decades ago, dense clusters of snails the size of doorknobs were easy to find, according to Mr. Avendaño. “Full of snails,” he said, sweeping a calloused, violet-stained hand across the coves. Now, most of the snails he finds are small, just over an inch, and yield only a few milliliters of dye.
Science
Video: This Parrot Has No Beak, But Is at the Top of the Pecking Order

new video loaded: This Parrot Has No Beak, But Is at the Top of the Pecking Order

By Meg Felling and Carl Zimmer
April 20, 2026
Science
Contributor: Focus on the real causes of the shortage in hormone treatments

For months now, menopausal women across the U.S. have been unable to fill prescriptions for the estradiol patch, a long-established and safe hormone treatment. The news media has whipped up a frenzy over this scarcity, warning of a long-lasting nationwide shortage. The problem is real — but the explanations in the media coverage miss the mark. Real solutions depend on an accurate understanding of the causes.
Reporters, pharmaceutical companies and even some doctors have blamed women for causing the shortage, saying they were inspired by a “menopause moment” that has driven unprecedented demand. Such framing does a dangerous disservice to essential health advocacy.
In this narrative, there has been unprecedented demand, and it is explained in part by the Food and Drug Administration’s recent removal of the “black-box warning” from estradiol patches’ packaging. That inaccurate (and, quite frankly, terrifying) label had been required since a 2002 announcement overstated the link between certain menopause hormone treatments and breast cancer. Right-sizing and rewording the warning was long overdue. But the trouble with this narrative is that even after the black-box warning was removed, there has not been unprecedented demand.
Around 40% of menopausal women were prescribed hormone treatments in some form before the 2002 announcement. Use plummeted in its aftermath, dipping to less than 5% in 2020 and just 1.8% in 2024. According to the most recent data, the number has now settled back at the 5% mark. Unprecedented? Hardly. Modest at best.
Nor is estradiol a new or complex drug; the patch formulation has existed for decades, and generic versions are widely manufactured. There is no exotic ingredient, no rare supply chain dependency, no fluke that explains why women are suddenly being told their pharmacy is out of stock month after month.
The story is far more an indictment of the broken insurance industry: market concentration, perverse incentives and the consequences of allowing insurance companies to own the pharmacy benefit managers that effectively control drug access for the majority of users. Three companies — CVS Caremark, Express Scripts and OptumRx — manage 79% of all prescription drug claims in the United States. Those companies are wholly owned subsidiaries of three insurance behemoths: CVS Health, Cigna and UnitedHealth Group, respectively. This means that the same corporation that sells you your insurance plan also decides which drugs get covered, at what price, and whether your pharmacy can stock them. This is called vertical integration. In another era, we might have called it a cartel. The resulting problems are not unique to hormone treatments; they have affected widely used medications including blood thinners, inhalers and antibiotics. When a low-cost generic such as estradiol — a medication with no blockbuster profit margins and no patent protection — runs into friction in this system, the friction is not random. It is structural. Every decision in that chain is filtered through the same corporate profit motive. And when the drug in question is an off-patent estradiol patch that has negligible profit margins because of generic competition but requires logistical investment to keep consistently in stock? The math on “how much does this company care about ensuring access” is not complicated.
Unfortunately, there is little financial incentive to ensure smooth, consistent access. There is, however, significant financial incentive to steer patients toward branded alternatives, or simply to let supply tighten — because the companies aren’t losing much profit if sales of that product dwindle. This is not a conspiracy theory: The Federal Trade Commission noted this dynamic in a report that documented how pharmacy benefit managers’ practices inflate costs, reduce competition and harm patient access, particularly for independent pharmacies and for generic drugs.
Any claim that the estradiol patch shortage is meaningfully caused by more women now demanding hormone treatments is a distraction. It is also misogyny, pure and simple, to imply that the solution to the shortage is for women’s health advocates to dial it down and for women to temper their expectations. The scarcity of estradiol patches is the outcome of a broken system refusing to provide adequate supply.
Meanwhile, there are a few strategies to cope.
- Ask your prescriber about alternatives. Estradiol is available in multiple formulations, including gel, spray, cream, oral tablet, vaginal ring and weekly transdermal patch, which is a different product from the twice-weekly patch and may be more consistently available depending on manufacturer and region.
- Consider an online pharmacy. Many are doing a good job locating and filling these prescriptions from outside the pharmacy benefit manager system.
- Call ahead. Patch shortages are inconsistent across regions and distributors. A call to pharmacies in your area, or a broader geographic radius if you’re able, can locate stock that your regular pharmacy doesn’t have.
- Consider a compounding pharmacy. These sources can sometimes meet needs when commercially manufactured products are inaccessible. The hormones used are the same FDA-regulated bulk ingredients.
Beyond those Band-Aid solutions, more Americans need to fight for systemic change. The FTC report exists because Congress asked for it and committed to legislation that will address at least some of the problems. The FDA took action to change the labeling on estrogen in the face of citizen and medical experts’ pressure; it should do more now to demand transparency from patch manufacturers.
Most importantly, it is on all of us to call out the cracks in the current system. Instead of repeating “there’s a patch shortage” or a “surge in demand,” say that a shockingly small minority of menopausal women still even get hormonal treatments prescribed at all, and three drug companies control the vast majority of claims in this country. Those are the real problems that need real solutions.
Jennifer Weiss-Wolf, the executive director of the Birnbaum Women’s Leadership Center at New York University School of Law, is the author of the forthcoming book “When in Menopause: A User’s Manual & Citizen’s Guide.” Suzanne Gilberg, an obstetrician and gynecologist in Los Angeles, is the author of “Menopause Bootcamp.”
-

 Miami, FL2 minutes ago
Miami, FL2 minutes agoRanking the Miami Heat’s Top Trade Targets
-

 Boston, MA8 minutes ago
Boston, MA8 minutes agoFormer Massachusetts doctor faces 81 new sexual assault charges
-

 Denver, CO14 minutes ago
Denver, CO14 minutes agoHouston County murder suspect returns to face charges after her arrest in Denver
-

 Seattle, WA20 minutes ago
Seattle, WA20 minutes agoWest Seattle Tool Library to host annual tool sale this Saturday, April 25 | The White Center Blog
-

 San Diego, CA26 minutes ago
San Diego, CA26 minutes agoBalboa Park museums see attendance decline of 34% in first quarter
-

 Milwaukee, WI32 minutes ago
Milwaukee, WI32 minutes agoMilwaukee County overdose deaths continue to fall, but challenges remain
-

 Atlanta, GA38 minutes ago
Atlanta, GA38 minutes agoDozens arrested during raid of drug
-

 Minneapolis, MN44 minutes ago
Minneapolis, MN44 minutes agoPrince’s legacy still shines in downtown Minneapolis 10 years after his death