Science
A UCLA doctor is on a quest to free modern medicine from a Nazi-tainted anatomy book

As Dr. Kalyanam Shivkumar pondered how to fix the human heart, he was given a gift laced with horror.
Shivkumar, a cardiac electrophysiologist known as “Shiv” to friends and co-workers at UCLA, was trying to better understand the intricate details of nerves in the chest. He hoped doing so might help him improve treatments for cardiac arrhythmias — aberrant rhythms of the heart — that can prove dangerous and even deadly.
A Canadian colleague sent him a set of anatomy books renowned for the beauty and detail of their drawings, but tipped him off that the “atlas” had an appalling history.
Shivkumar was aghast to learn it was the work of an ardent Nazi whose Vienna institute had dissected the bodies of prisoners, many executed for political reasons after Austria was annexed to Nazi Germany in 1938.
“Every time I open up that book,” he said, “my sense is revulsion.”
Shivkumar is a big thinker, an erudite physician quick with an apt quotation, whose Westwood office is stacked with Sanskrit volumes of the Mahabharata alongside books about late Bruins basketball coach John Wooden.
Dr. Shumpei Mori sets up a donated heart to be photographed at UCLA as part of the Amara Yad project to create new, ethically made anatomical images.
(Allen J. Schaben / Los Angeles Times)
As he waded into the scholarly debate over using the tainted atlas, the doctor bristled at hearing others praise its illustrations as “unsurpassable.” Much of the soul searching among physicians had revolved around when and how to use it. Shivkumar wanted to put those questions to bed.
“Could we be better?” he asked. “Could we not be making something that’s completely untainted?”
That question would launch Shivkumar on a quest that has lasted more than a decade and is expected to endure for years. He wants to surpass the anatomical atlas created by Dr. Eduard Pernkopf, a fervent supporter of the Nazi regime whose work was fueled by the dead bodies of its victims.
His passion project at the UCLA Cardiac Arrhythmia Center is called Amara Yad, a mashup of Sanskrit and Hebrew meaning “immortal hand.” The work has relied on the generosity of people who have willed their bodies for use at UCLA, as well as hearts that were donated but could not be used for transplant.
So far, Amara Yad has completed two volumes focused on the anatomy of the heart and is enlisting teams at other universities for more. The plan is to draft a freely available, ethically sourced road map to the entire body that eclipses the weathered volumes of watercolors from Pernkopf and honors the Nazis’ victims.
Anatomists have told him, “‘You’re crazy. It’s impossible. How could you ever surpass it?’” Shivkumar said of the Pernkopf atlas in a speech last year before members of the Heart Rhythm Society.
But “can it be beaten? The answer is yes.”
For decades, the origins of the Pernkopf Atlas were unknown to many who turned to its pages for guidance. Swastikas tucked into signatures of an illustrator were airbrushed out in later editions. Its history began to trickle out in journals in the 1980s.
When Dr. Howard Israel finally learned of its roots, he was horrified. Israel, an oral surgeon at Columbia University and self-described “very ordinary American Jew,” told the New York Times he had been relying on the book since he was a medical student.
‘’I felt stupid at using the book,” he told the newspaper, “that I could possibly have benefited from something that sounded so evil.” He and another physician enlisted the Holocaust remembrance group Yad Vashem and publicly pushed for the University of Vienna to investigate whose bodies were depicted in its pages.
The resulting probe found no evidence that the anatomy department under Pernkopf — who had ascended to become dean of the medical faculty at the University of Vienna in 1938 — had received bodies from the Mauthausen concentration camp, as some had wondered.
But the institute had been given at least 1,377 bodies of executed people, most of them sentenced to death for political reasons. Among the charges that led to their executions: “crimes of resistance” and “high treason.”
Using the bodies of executed people was “a centuries-old practice in anatomy,” preferred because anatomists could time their work swiftly after a scheduled death, said Dr. Sabine Hildebrandt, an anatomy educator at Harvard Medical School. What was new under the Nazis, she said, was the sheer number of executions.
The institute “was drowned in bodies,” and “the source for these bodies was mostly connected with the apparatus of repression of the Nazi regime,” said historian Herwig Czech, a member of the Lancet Commission on Medicine, Nazism, and the Holocaust, at a recent forum.
By the time those findings emerged, the publisher of the anatomy book had stopped printing it.
1

2

1. A stack of volumes of the Pernkopf atlas on a shelf in Dr. Kalyanam Shivkumar’s UCLA office. 2. Erich Lepier, one of the Pernkopf atlas illustrators, repeatedly included a swastika after the cursive R in his signature. (Allen J. Schaben / Los Angeles Times)
Yet use of the atlas persisted. Hildebrandt said that a decade ago, dental students in her classes “were basically giving each other thumb drives with bootlegged copies of the head and neck.”
Other anatomical atlases exist, but these illustrations had especially fine details, including of the nerves extending beyond the brain and spiral cord. One survey of nerve surgeons found that 13% of respondents were using the atlas. Among those who have publicly grappled with it is Dr. Susan Mackinnon, a surgery professor at Washington University School of Medicine in St. Louis known as a pioneer in nerve regeneration.
“I used this textbook for years before I knew the history of it,” she said. “My brain is contaminated with that. I can’t undo that.”
Mackinnon sought ethical guidance. Rabbi Joseph Polak, a Boston University assistant adjunct professor of health law who survived the concentration camps as a child, said one dilemma involved a patient in excruciating pain.
Polak recalled that the patient had told Mackinnon that “if you can’t find the nerve to stop the pain, then I want my leg amputated.” The rabbi walked through Jewish teachings that applied to the ethical quandary and conferred with other experts, penning a set of recommendations called the Vienna Protocol.
Among his urgings to doctors: If you use these drawings, make it clear to patients where they came from.
The Third Reich wanted “to extinguish them and to extinguish eventually all memory of them,” the rabbi said of Holocaust victims, speaking at a recent forum about the atlas. But when a doctor tells patients about what happened to the people depicted in the drawings, he said, “they’re being called out of that darkness.”
Mackinnon now keeps the atlas locked away. In the rare cases she feels she needs to consult it to operate, she tells patients and co-workers about the man behind it. His firings of Jewish doctors. The grim details in its pages — shorn hair, emaciated bodies — that began to raise suspicions about its terrible origins.
The only reason to use it, she said, is to save someone from misery — and only if “nothing else will help you.”

“Could we be better” than Pernkopf? Shivkumar asked. “Could we not be making something that’s completely untainted?”
(Allen J. Schaben / Los Angeles Times)
Shivkumar said his goal is to eliminate the need to consult those pages at all. Inside UCLA’s Center for the Health Sciences in Westwood, he showed off a donated heart, prepped and ready for its close-up in a corner of the lab outfitted with a black backdrop and brilliant lights.
A spent heart normally wilts like a deflated balloon, but this one had been pumped with chemicals to imitate the fullness of life. The team first puts the organs to use in research, then carefully dissects them for imaging.
Bringing out a bisected piece of a heart, Dr. Shumpei Mori displayed how its inner architecture could be captured on camera, threading a catheter through the organ as a co-worker snaked in an endoscope.
“The internal structure is really fine and delicate,” said Mori, a specialist in cardiac anatomy who had jumped at the chance to do something new in the field.
“Even Pernkopf simplified the anatomy” in its drawings, Mori said. “What we are doing is more complicated.”
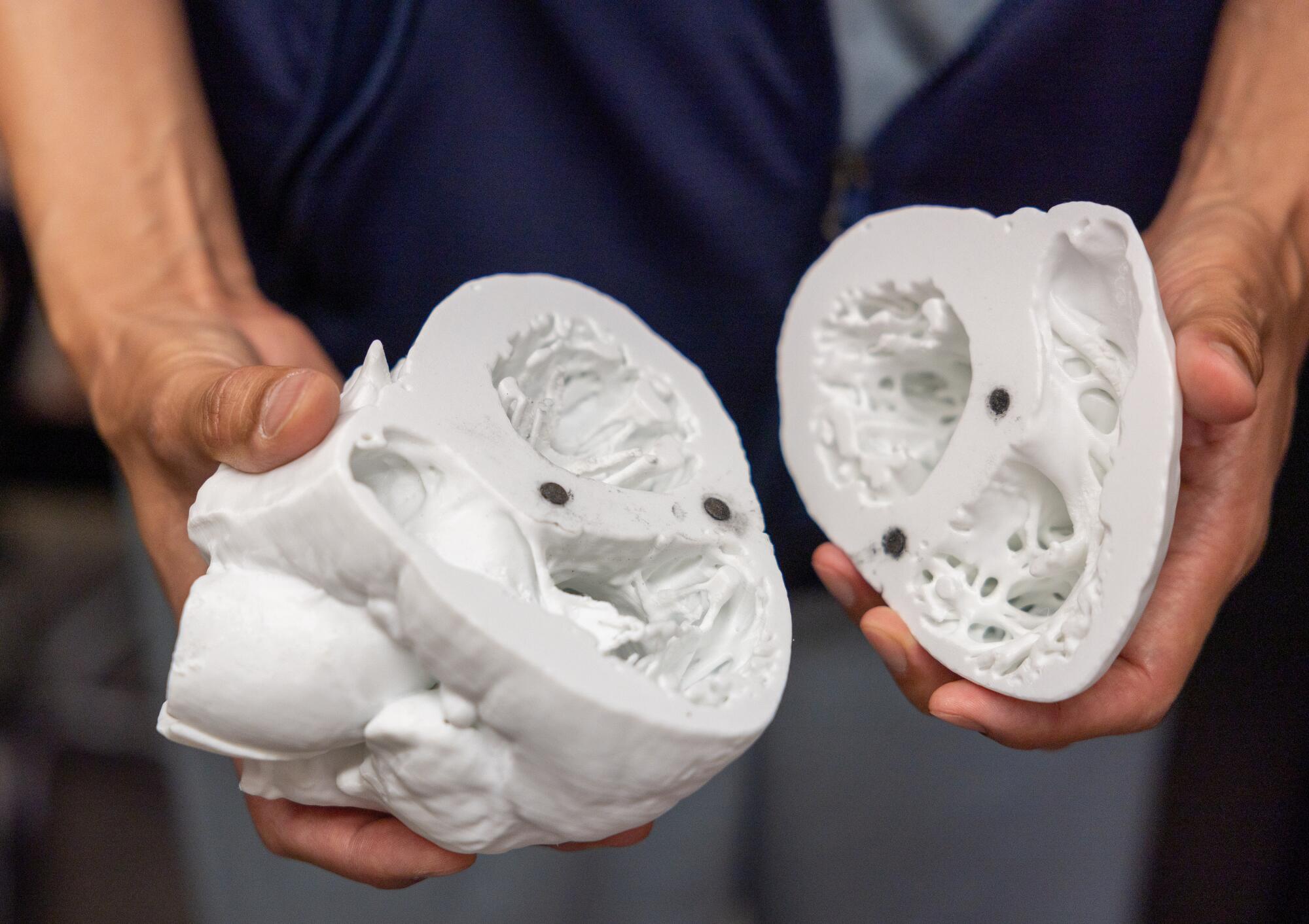
Dr. Shumpei Mori holds a detailed model of a heart. “Even Pernkopf simplified the anatomy,” he said. “What we’re doing is more complicated.”
(Allen J. Schaben / Los Angeles Times)
The camera is far from their only tool: The team has generated 3-D images to illustrate the dimensions of the inner structures of the heart; done CT scans to produce hand-held models; and used sophisticated imaging from a microscope to reveal the lattice of nerves connecting to the organ — part of the signaling system that Shivkumar calls “the internet of the human body.”
In another lab, Mori carefully unzipped a bag on a metal gurney to reveal the stripped-down interior of a cadaver diligently dissected over a year and a half, its rib cage cracked open like a weighty book. Shivkumar pointed out the pale web of nerves stretching up through the neck. Mori had painted them yellow by hand.
The human body might seem like well-traveled territory, but as physicians work to find less invasive ways of healing, such as attacking a cancer with ultrasound, Shivkumar said there is “a volcanic desire for this kind of information.” Snip the right nerve, he said, and you can avert the need for a heart transplant.
“Pernkopf never did nerves like this,” he said with pride.
Amara Yad is also an act of “moral repair” meant to honor the victims, said Dr. Barbara Natterson-Horowitz, a UCLA cardiologist and evolutionary biologist who helped support the project. The Nazi atlases “were like documents of death. The atlases that Shiv is creating are really living, interactive tools to support life.”
When Shivkumar decided to launch the project, he had been inspired by the words of USC emeritus professor of rheumatology Dr. Richard Panush, who had pushed to set the atlas aside in the library of the New Jersey medical center where he had worked, moving it to a display case that explained its history.
Panush said the old atlas should be preserved only as “a symbol of what we should not do, and how we should not behave, and the kind of people that we cannot respect.”
Doctors need to know that history to understand their own moral fallibility, Hildebrandt said. Physicians in Nazi Germany “still thought they were doing the right thing,” she said, even as they failed to see some people as human.
Rabbi Polak stressed that doctors at the time “had the deepest, most profound respect of the masses.”
Yet when the Nazis took power, “it turned out that a vast proportion of them were moral sleazeballs,” Polak said. “They were the first to join when they saw that it could promote their careers.”

Model hearts line a bookshelf at UCLA. The Amara Yad project is working with other universities to tackle other parts of human anatomy.
(Allen J. Schaben / Los Angeles Times)
Shivkumar said that beyond making new tools for physicians, the Amara Yad project is working with Oxford University to develop an accompanying curriculum that will explore ethical failures in medicine. Pernkopf’s anatomy book is only one example.
The history of the atlas “invites the contemplation of how doctors and medical scientists and anatomists are related to a regime,” said Sari J. Siegel, who heads the Center for Medicine, Holocaust and Genocide Studies at Cedars-Sinai. Thinking about it underscores that “medicine is political.”
“It can’t be divorced from the larger contexts in which it exists.”
Shivkumar, born to a Hindu family in the southernmost state of India, is used to people wondering why he became “possessed” with this project. He recalls first learning about the Holocaust from a photographer friend of his grandfather, a former newspaper editor once imprisoned for sedition against the British Empire.
He was 11 when the photographer showed him images dating to World War II, and it chilled him “to see that human beings could be so brutal to other humans.” As a child, his parents had told him they owed the world because their part of India was lucky to be long spared from such conflict.
In Amara Yad, we “get a rare opportunity in history to correct an unbelievably depressing stain that was placed in our field,” he told the Heart Rhythm Society.
It irritates him to think of the abundant resources that a Nazi had at hand to do this sort of work. “Imagine having five Shumpeis!” he exclaimed at one point, gesturing at his colleague who hand painted the nerves. At UCLA, the project has piggybacked on ongoing research and relied on donations. He is hoping to garner $500,000 annually to continue and expand the work.
But Shivkumar likes to quote the Emperor Ashoka on that point: “To do good is difficult. One who does good first does something hard to do. … Truly, it is easy to do evil.”

Science
Video: NASA Announces Artemis III Crew

new video loaded: NASA Announces Artemis III Crew
transcript
transcript
NASA Announces Artemis III Crew
NASA announced the crew of Artemis III mission, which will fly to low-Earth orbit to test rendezvous and docking maneuvers with one or two lunar landers.
-
“I am excited to welcome you as the next crew in the Artemis journey to successfully return to the moon — this time to stay.” “I’m honored by the role that I’ve been given. I’m also very humbled by the task in front of us. But first and foremost, I’m grateful.” “So with that, the Artemis II crew, comrade, hands you the baton. You got the controls.” “As you know, we had a significant anomaly at our Launch Complex 36A on May 28. We’ve redoubled our efforts and are moving forward.”
By Alisa Shodiyev Kaff
June 9, 2026
Science
Santa Monica Mountains’ last steelhead trout survived the Palisades fire — and even had babies

Scientists feared the Santa Monica Mountains’ last remaining steelhead trout were dead, smothered by debris flows unleashed by the Palisades fire.
But the endangered fish surprised them: A team of biologists recently spotted 30 of the rare trout — and 21 babies — in Topanga Creek.
“There was a lot of happy dancing in the creek,” said Rosi Dagit, principal conservation biologist for the Resource Conservation District of the Santa Monica Mountains, which works with public and private landowners to conserve natural resources.
That’s because the steelhead here are endangered, at both the state and federal levels. Once, they swam in most streams of the Santa Monicas, but their numbers plummeted amid overfishing and coastal development. Increasingly frequent wildfire has further stressed their habitat. Topanga Creek, a biodiversity hot spot, is home to their last known population in the mountains that stretch from the Hollywood Hills to Point Mugu in Ventura County.
The trout that were spotted, including this one, are part of a distinct Southern California population that’s listed as endangered at the state and federal levels.
(RCDSMM Stream Team)
The California Department of Fish and Wildlife spearheaded a complex mission to rescue trout threatened by the Palisades fire that sparked in January 2025.
Time was of the essence. The fire hadn’t yet been fully contained. But rain was on the way, which would sweep massive amounts of sediment from the denuded hillsides into the water. Fish are often killed this way.
Crews stunned the fish with electricity, scooped them up in buckets, trucked them to a hatchery and ultimately moved them to Arroyo Hondo Creek in Santa Barbara County.
Within days, Topanga Creek was choked with mud. Some assumed the fish left behind were goners.
But in March, the conservation district’s team found four. The following month, when water conditions were clearer, they saw more.
“These fish continue to amaze me,” said Kyle Evans, environmental program manager for the state Department of Fish and Wildlife, who had seen the damage to the creek. “I had seen populations get wiped out in similar situations. So when I heard, I was thrilled.”
Evans surmises the fish that survived were in an area of the creek where less charred material and sediment were swept in.
“These fish likely hunkered down, were hiding under some rocks or places to try to get away from the main concentration of flow,” he said. “And luckily they weren’t buried.”
The ones that were spotted were fairly small, around 6 to 14 inches. Rainbow trout and steelhead trout are the same species, but with different lifestyles. If the fish remain in freshwater, they’ll be considered rainbows. However, they can migrate to the ocean and become steelhead, where they typically grow larger before returning to their natal waters to spawn.
Topanga Creek hasn’t fully recovered from the damage it sustained, but scientists say it’s looking better. Surveys last year were “so depressing,” Dagit said, with very few animals, and stretches that were essentially transformed into flat roads from all the sediment buildup. Some of the riparian canopy burned right down to the creek.
Then came 32 inches of rain over the last nine months, scouring out and moving sediment, creating deeper pools. Dagit said they recently found newt egg masses for the first time in years, as well as a few adult newts and many frogs. Plants that provide cover are starting to recover.
She provided photos comparing certain pools last year and this year, some dramatically transformed. In September 2025, the Shrine Pool could have been an overgrown hiking trail. This April, it was filled with shallow water.

The Shrine Pool in September 2025, left, and the same location in April 2026, right, with RCDSMM’s Isaac Yelchin donning a wetsuit.
(RCDSMM Stream Team)
Topanga Creek is home to another endangered fish, the small but hardy northern tidewater goby, often described as cute. Not long before the trout operation, Dagit led a rescue of hundreds of these fish too. Many were repatriated to the lagoon at the mouth of the creek in a moving ceremony last June.
There’s still the matter of what to do with the trout that were moved to Santa Barbara County last year. Evans would like to bring them home to the Santa Monicas at some point, but isn’t sure if it will happen. On one hand, they could bolster the small, genetically isolated surviving population. On the other, they might inadvertently bring in a disease or bacteria. There is some time to decide. Evans estimates the creek still needs to recover for two to three more years.
For now, the fish are functioning fine in their adopted creek. Experts worried the trauma wrought by the move would disrupt their spawning process, but they had babies that spring. This year, they spawned again.
Science
Pacifica pier cracks, another coastal casualty as seas continue to rise

The Pacifica Municipal Pier was shut down and taped off Thursday after city workers noticed cracks running through the landmark structure and concrete chunks falling into the ocean.
It’s just one of many coastal California structures that have recently crumbled under pressure from a rising and relentless ocean.
Officials from the small, beach city south of San Francisco said the pier was closed due to “cracking, separation, and displacement of the concrete walkway and structural elements.”
It will stay closed while structural engineers asses its safety.
Photos taken by city employees show a wide crack that runs from top to bottom and across the structure as well. Other photos show a large horizontal crack under the foundation of a small restaurant on the pier, the Chit Chat Cafe.
The cafe was also shut down.
This is not the first time the 53-year-old pier has shown signs of stress. In 2021, part of it was shut down after handrails along the edge collapsed. And in 2023, after a series of storms pummeled the Central California coast, damaging parts of the pier, the structure was partially closed for more than year.
Those same storms caused extensive damage in Aptos and Capitola, 70 miles south, where piers and waterfront infrastructure were swept away or damaged.
In 2024, a 150- to 180- foot section of the Santa Cruz wharf was ripped off by powerful waves.
At least 10 of the state’s dozens of coastal public piers were closed for part or all of 2024 due to structural damage sustained in winter storms since 2022. At least five others have longer-term upgrades planned to address structural issues.
“These things are costly to maintain,” said Zach Plopper, senior environmental director at Surfrider. “They are a part of our California coastal culture in many ways, but we’re going to need to reckon with, one, the state that they’re in, and two, the continuous and worsening threats they’re going to experience,”
He said most of the piers were constructed in the early 1900s, and they weren’t built to withstand decades of rough seas, storms and rising sea level.
“With this incoming El Niño, which is forecasted to be significant, and this marine heat wave we’re in the midst of, we’re kind of in uncharted waters as far as what this winter could bring in terms of storms and swells to the California coast, and we’re likely going to see a lot more damage,” he said. “Not just piers, but roads and other coastal infrastructure up and down the state.”
There was no storm in Pacifica earlier this week, so no single event could be blamed for the destruction.
However, a 2025 report from an outside engineering firm, GHD, found that several sections of the pier were in “poor” or “serious” condition, and they recommended closure before anticipated storms or events that could “subject the piles to high winds, swells and large waves.”
The firm found several areas of the pier where concrete was missing and rebar was exposed and corroding.
“The pier has continued to experience high winds and large waves in a harsh marine environment,” the engineers wrote in the report, noting that continuous exposure to seawater or marine spray was “detrimental” to the structure.
A 2023 city report estimated it would cost $19 million to repair.
That same year, a state law was enacted to require local governments along the California coast to plan for sea level rise in the coming decades.
Sea level has risen some 8 inches, on average, along the coast in the past 150 years, Plopper said, and researchers anticipate another foot in the next 25 years.
“We’re going to see profound shifts on our coastline, none that we have ever experienced before, and building static structures on the coast just doesn’t work all that well,” he said. “We’re going to have to make some really hard decisions.”
-

 Business45 seconds ago
Business45 seconds agoPrimm is a spooky shell of its former self. But the gambling oasis may have found a savior
-

 Entertainment6 minutes ago
Entertainment6 minutes agoHiker who died in Runyon Canyon ID’d as Hollywood screenwriter, pal of Caitlyn Jenner
-

 Politics16 minutes ago
Politics16 minutes agoSupporters of L.A. County healthcare sales tax declare victory
-

 Sports28 minutes ago
Sports28 minutes agoUSC freshman linebacker Talanoa Ili joins lawsuit seeking to upend new NIL system
-

 World36 minutes ago
World36 minutes agoWho has the most and fewest judges in the EU?
-

 News56 minutes ago
News56 minutes agoIn Nevada, Trump’s policies are making things tough for Republican Gov. Joe Lombardo
-

 New York2 hours ago
New York2 hours agoThis Parking Spot Is Free. Should It Be?
-

 Los Angeles, Ca2 hours ago
Los Angeles, Ca2 hours agoO.C. Uber customer says driver asleep in Tesla on 405 Freeway