Science
'We've created medical refugees.' LGBTQ+ healthcare workers fight for gender-affirming care amid rise in anti-trans laws

Nico Olalia had just finished her initial nurse training in the Philippines when she realized her aspirations were growing bigger than her home archipelago.
“There are a lot of trans Filipinos, but they’re always known in the beauty industry, and they’re very seldom found in the professional side,” Olalia said.
So she moved back to the United States, where she was born, for better career prospects. Today, she is a clinical nurse at Cedars-Sinai, one of the largest hospitals in Southern California, where she assists new hires and cares for patients in the neurology division.
Olalia feels like it’s a dream come true; her peers and patients respect her and welcome her contributions. It’s a hope shared by a small but growing number of trans and nonbinary healthcare workers in the U.S.
Yearly surveys of first-year medical students by the Assn. of American Medical Colleges show that the percentage identifying as transgender and gender nonconforming doubled from 0.7% in 2020 to 1.4% in 2023.
These numbers align with the growing LGBTQ+ population in the United States. Today, younger generations are more likely to identify as LGBTQ+ than generations before. A national survey this year found that 28% of Gen Z respondents identified as lesbian, gay, bisexual, transgender or queer.
But that rise in LGBTQ+-identified youths and trans healthcare workers has coincided with escalating restrictions on gender-affirming care.
Between 2022 and 2023, anti-trans legislation proposed across statehouses tripled, with a majority of the bills proposing restrictions on gender-affirming care. According to the Movement Advancement Project, at least half of the states exclude transgender-related healthcare for youths from their Medicaid programs, while only 22 explicitly cover it.
U.S. Assistant Secretary for Health Rachel Levine, center, is shown at a transgender health event in Miami with Tatiana Williams, left, of Transinclusive Group and Arianna Inurritegui-Lint of Arianna’s Center.
(Wilfredo Lee / Associated Press)
“We’ve created medical refugees who have to leave their state to get that care,” said U.S. Assistant Secretary for Health Rachel Levine, the first transgender person confirmed by the Senate to a high government post.
“Transgender medicine can be suicide prevention care. It’s been shown in many studies that it improves the quality of life and can save lives for youth and adults,” said Levine, a pediatrician specializing in adolescent care.
When Levine was doing her medical residency at Mount Sinai Hospital in New York City during the 1980s AIDS crisis, she saw friends and co-workers succumb to the epidemic — an experience that rings eerily familiar to the discrimination she sees transgender people facing today, she said.
One study from 2023 showed that 70% of transgender and gender nonconforming patients faced at least one negative interaction with a healthcare provider, ranging from an “unsolicited harmful opinion about gender identity to physical attacks and abuse.” It was only in 2019 that the World Health Organization removed gender dysphoria from its list of mental health illnesses.
Alex Keuroghlian, a clinical psychologist at Harvard Medical School, directs training programs through the National LGBTQIA+ Health Education Center that educate healthcare providers across the country on gender-affirming care. They’ve noticed a double standard when it comes to the doubts that people raise against transgender healthcare.
“Given how well resourced anti-trans political groups are, it can really distort the public discourse and make it harder to advance evidence-based, clinically sound practices,” Keuroghlian said of the rampant misinformation they’ve seen online.

Mack Allen, an 18-year-old transgender high school student from Leavenworth, Kan., stands with other young advocates of LGBTQ+ rights after a rally at the state capitol in Topeka, Kan.
(John Hanna / Associated Press)
An uptick in the number of transgender-identifying youths seeking gender-affirming care sparked a theory that “social contagion” was influencing teens to experience “rapid-onset gender dysphoria.” Some practitioners oppose this framing, and research published by the American Academy of Pediatrics has disproved it. Both the American Psychiatric Assn. and the American Pediatric Assn. support gender-affirming care for adolescents.
The news on the legal front hasn’t been all bad for trans healthcare providers; last month, a federal court judge struck down Florida’s law restricting gender-affirming care for minors and adults. However, the practice of categorizing gender in a binary medical system continues.
That’s problematic, said Mauricio Dankers, the intensive care unit director at HCA Florida Aventura Hospital, because the medical erasure of trans people can prevent a proper diagnoses. When doctors have to make split-second decisions in the ICU, he said, failing to recognize a transgender person could prevent them from receiving lifesaving care.
“If I don’t know that a transgender woman may have gone through laryngoplasty to change the tone of her voice, I’m going to go and put the breathing tube [and] I may run into trouble,” Dankers offered as an example. Chest binding used by some transgender people to appear more masculine can also lead to pneumonia if done improperly, he said.

Violet Rin, a transgender woman in Florida, gives herself estrogen injections once a week.
(Francine Orr/Los Angeles Times)
Dankers, a gay immigrant who left Peru for the more tolerant New York City, worries that the politicization of transgender healthcare will put a target on LGBTQ+ healthcare providers.
These restrictions “are going to change how the LGBTQ+ trainee thinks about their career,” Dankers said. He said they might think, “I’m not going to a place where they don’t want me by law.”
After Texas banned gender-affirming care for teens, a pediatric endocrinologist closed her practice and moved out of the state because she feared violence from armed protesters. And this year, a Texas man was sentenced to three months in prison for threatening a Boston physician serving transgender patients.
Fear and violence have had a ripple effect even on states that have enshrined transgender healthcare into law.
Baltimore Safe Haven, a nonprofit that provides transitional housing service focused especially on Black trans women, received an increase of 7,000 calls last year after Gov. Wes Moore signed an executive order protecting gender-affirming medical care in Maryland, according to the Baltimore Sun. Most of the callers lived out of state.
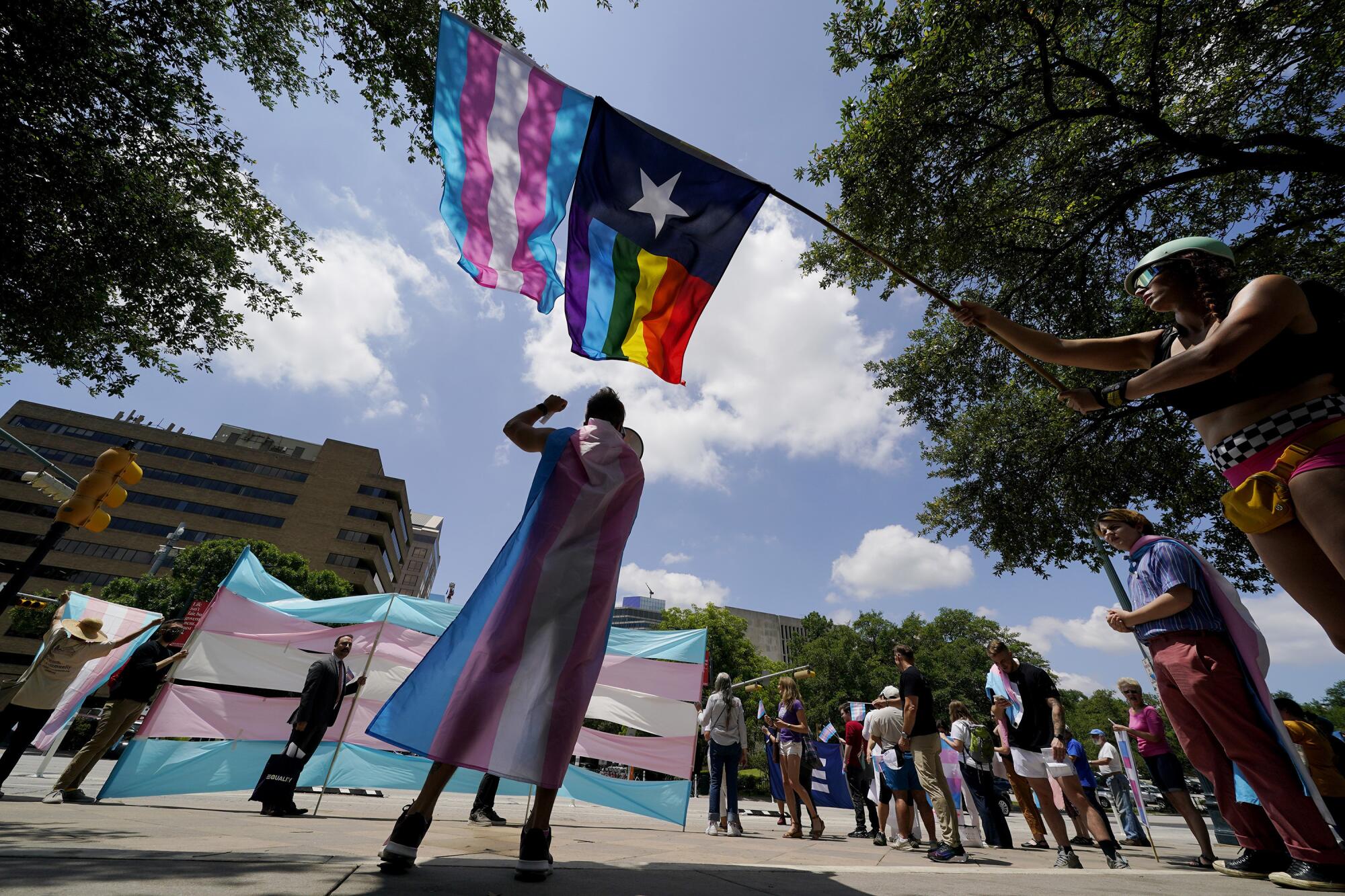
Demonstrators gather on the steps to the state capitol to speak against transgender-related bills being considered in the Texas Legislature.
(Eric Gay / Associated Press)
“I can’t even see my own doctor,” said Jules Gill-Peterson, a transgender woman and associate professor at Johns Hopkins University in Baltimore who studies the history of transgender medicine. Anecdotally, she’s heard of doctors’ caseloads tripling with the slew of requests they receive from new transgender patients.
“It’s only going to put greater pressure on [the] system as people migrate from states where it’s illegal to transition medically to states where it’s not,” Gill-Peterson said.
LGBTQ+ healthcare workers are on the defensive, said Kate Steinle, a queer nurse and chief clinical officer at Folx, a nationwide healthcare provider that serves transgender and queer patients.
“Our general counsel wakes up in the morning and is looking at every single possible legislation that could affect our care,” Steinle said. Folx lobbies the government to ensure that its patients have access to gender-affirming care, but Steinle said fighting anti-trans legislation can sometimes feel like “a game of whack-a-mole” — as one goes down, another takes its place.
Anti-trans legislation is largely symbolic because most of these bills fail, said D Dangaran, a lawyer and director of gender justice at Rights Behind Bars. According to the Trans Legislation Tracker, of the 617 bills introduced, 44 have passed, 348 failed and the rest are pending.
But the fate of transgender healthcare could shift dramatically depending on the outcome of the presidential election in November.
“A Trump presidency will signal to the states another possibility to move forward on all fronts with anti-trans legislation,” Dangaran said. Former President Trump has promised to end gender-affirming care for minors if he wins, and Dangaran anticipates that he would sign “executive orders that are antithetical to protecting trans rights.”

Glenda Starke wears a transgender flag as a counterprotest during a rally in favor of a bill to ban gender-affirming care at the Missouri Capitol in Jefferson City, Mo.
(Charlie Riedel / Associated Press)
Keuroghlian worries that many career government employees in the Department of Health and Human Services could be ousted by political appointees as part of Trump’s ambition to reshape the federal workforce. “There is a lot of important healthcare and research funded by the federal government,” he said.
All of this could reverse the progress that the Biden administration has done to advance gender-affirming care across the country.
“There hasn’t been any president that has more explicitly supported access to gender-affirming care,” said Elana Redfield, the federal policy director at the Williams Institute at UCLA School of Law.
Last week, the Supreme Court agreed to consider the Biden administration’s challenge to Tennessee’s ban on gender-affirming care for teens. The administration argues that the ban violates the 14th amendment’s equal protection clause. A ruling is expected next year that could cement or further erode transgender rights.
Redfield warns that “people who are multiply marginalized are also most affected by these laws,” particularly people of color who live in the Deep South. Beyond the legal restrictions to care, they face problems affording the cost of procedures such as gender-affirming surgery and traveling to where care is available, she said.
Nor can lower-income transgender people afford Folx, a private subscription service that charges $39.99 a month on top of any out-of-pocket costs and co-pays levied by an insurer.
“Trans people have a lot to tell us about just how bad U.S. healthcare can get,” Gill-Peterson said. “Trans healthcare is not really that different than the rest of healthcare.”

People attend a rally as part of a Transgender Day of Visibility on March 31, 2023, by the U.S. Capitol in Washington.
(Jacquelyn Martin / Associated Press)
Increasing the representation of transgender people in a healthcare system where “profit is placed over people” won’t solve those fundamental inequities, she said. Even if doctors support their transgender patients, Gill-Peterson said, they are still bound by law to follow state regulations and insurers’ dictates.
On the other hand, studies have linked positive health outcomes in LGBTQ+ patients and patients of color to having a healthcare provider who shares their background. That’s one reason University of Michigan medical student Gaines Blasdel, a trans man, wants to become a urologist who can provide gender-affirming surgery to transgender patients such as himself.
Blasdel said gender-affirming care can be an abstract social justice issue to his cisgender classmates, but it isn’t to him. “I’ve been embedded [in medicine] and I’m going to be, no matter how hard it is.”
Jona Tanguay, a physician assistant and medical lead in the medical substance use disorder programs at Whitman-Walker Health in Washington, D.C., said it’s important not to discredit the incremental but meaningful progress in the representation and quality of care offered to transgender people.
“Progress isn’t always linear,” they said. Tanguay, who is nonbinary, is also the president of GLMA, formerly known as the Gay and Lesbian Medical Assn. They already see the curriculum expanding and the number of out transgender healthcare providers growing steadily. “Every generation after is going to be more self-aware than they used to be about health disparities.”

Nico Olalia, a transgender woman, moved back to the United States from the Philippines for better career opportunities as a nurse.
(Jireh Deng / Los Angeles Times)
Olalia said her story demonstrates that trans people can practice medicine just as well as their cisgender colleagues. Because she’s also enrolled full time in a nursing doctoral program, her days start at 4:30 a.m., when she wakes up to prepare for her 10- to 12-hour shifts. Her efforts at Cedars-Sinai earned her a prestigious $10,000 no-strings-attached grant from the Simms/Mann Institute & Foundation.
“I do hope that I can have more power to inspire transgender women,” Olalia said. “I want those who are walking behind me to … have that opportunity to go beyond what they’re told to do or what society deems them to be.”

Science
Newsom’s fight with Trump and RFK Jr. on public health

SACRAMENTO — California Gov. Gavin Newsom has positioned himself as a national public health leader by staking out science-backed policies in contrast with the Trump administration.
After Health and Human Services Secretary Robert F. Kennedy Jr. fired Centers for Disease Control and Prevention Director Susan Monarez for refusing what her lawyers called “the dangerous politicization of science,” Newsom hired her to help modernize California’s public health system. He also gave a job to Debra Houry, the agency’s former chief science and medical officer, who had resigned in protest hours after Monarez’s firing.
Newsom also teamed up with fellow Democratic governors Tina Kotek of Oregon, Bob Ferguson of Washington and Josh Green of Hawaii to form the West Coast Health Alliance, a regional public health agency, whose guidance the governors said would “uphold scientific integrity in public health as Trump destroys” the CDC’s credibility. Newsom argued establishing the independent alliance was vital as Kennedy leads the Trump administration’s rollback of national vaccine recommendations.
More recently, California became the first state to join a global outbreak response network coordinated by the World Health Organization, followed by Illinois and New York. Colorado and Wisconsin signaled they plan to join. They did so after President Trump officially withdrew the United States from the agency on the grounds that it had “strayed from its core mission and has acted contrary to the U.S. interests in protecting the U.S. public on multiple occasions.” Newsom said joining the WHO-led consortium would enable California to respond faster to communicable disease outbreaks and other public health threats.
Although other Democratic governors and public health leaders have openly criticized the federal government, few have been as outspoken as Newsom, who is considering a run for president in 2028 and is in his second and final term as governor. Members of the scientific community have praised his effort to build a public health bulwark against the Trump administration’s slashing of funding and scaling back of vaccine recommendations.
What Newsom is doing “is a great idea,” said Paul Offit, an outspoken critic of Kennedy and a vaccine expert who formerly served on the Food and Drug Administration’s vaccine advisory committee but was removed under Trump in 2025.
“Public health has been turned on its head,” Offit said. “We have an anti-vaccine activist and science denialist as the head of U.S. Health and Human Services. It’s dangerous.”
The White House did not respond to questions about Newsom’s stance and Health and Human Services declined requests to interview Kennedy. Instead, federal health officials criticized Democrats broadly, arguing that blue states are participating in fraud and mismanagement of federal funds in public health programs.
Health and Human Services spokesperson Emily Hilliard said the administration is going after “Democrat-run states that pushed unscientific lockdowns, toddler mask mandates, and draconian vaccine passports during the COVID era.” She said those moves have “completely eroded the American people’s trust in public health agencies.”
Public health guided by science
Since Trump returned to office, Newsom has criticized the president and his administration for engineering policies that he sees as an affront to public health and safety, labeling federal leaders as “extremists” trying to “weaponize the CDC and spread misinformation.” He has excoriated federal officials for erroneously linking vaccines to autism, warning that the administration is endangering the lives of infants and young children in scaling back childhood vaccine recommendations. And he argued that the White House is unleashing “chaos” on America’s public health system in backing out of the WHO.
The governor declined an interview request, but Newsom spokesperson Marissa Saldivar said it’s a priority of the governor “to protect public health and provide communities with guidance rooted in science and evidence, not politics and conspiracies.”
The Trump administration’s moves have triggered financial uncertainty that local officials said has reduced morale within public health departments and left states unprepared for disease outbreaks and prevention efforts. The White House last year proposed cutting Health and Human Services spending by $33 billion, including $3.6 billion from the CDC. Congress largely rejected those cuts last month, although funding for programs focusing on social drivers of health, such as access to food, housing and education, were axed.
The Trump administration announced that it would claw back more than $600 million in public health funds from California, Colorado, Illinois and Minnesota, arguing that the Democratic-led states were funding “woke” initiatives that didn’t reflect White House priorities. Within days, the states sued and a judge temporarily blocked the cut.
“They keep suddenly canceling grants and then it gets overturned in court,” said Kat DeBurgh, executive director of the Health Officers Assn. of California. “A lot of the damage is already done because counties already stopped doing the work.”
Federal funding has accounted for more than half of state and local health department budgets nationwide, with money going toward fighting HIV and other sexually transmitted infections, preventing chronic diseases, and boosting public health preparedness and communicable disease response, according to a 2025 analysis by KFF, a health information nonprofit that includes KFF Health News.
Federal funds account for $2.4 billion of California’s $5.3-billion public health budget, making it difficult for Newsom and state lawmakers to backfill potential cuts. That money helps fund state operations and is vital for local health departments.
Funding cuts hurt all
Los Angeles County public health director Barbara Ferrer said if the federal government is allowed to cut that $600 million, the county of nearly 10 million residents would lose an estimated $84 million over the next two years, in addition to other grants for prevention of HIV and other sexually transmitted infections. Ferrer said the county depends on nearly $1 billion in federal funding annually to track and prevent communicable diseases and combat chronic health conditions, including diabetes and high blood pressure. Already, the county has announced the closure of seven public health clinics that provided vaccinations and disease testing, largely because of funding losses tied to federal grant cuts.
“It’s an ill-informed strategy,” Ferrer said. “Public health doesn’t care whether your political affiliation is Republican or Democrat. It doesn’t care about your immigration status or sexual orientation. Public health has to be available for everyone.”
A single case of measles requires public health workers to track down 200 potential contacts, Ferrer said.
The U.S. eliminated measles in 2000 but is close to losing that status as a result of vaccine skepticism and misinformation spread by vaccine critics. The U.S. had 2,281 confirmed cases last year, the most since 1991, with 93% in people who were unvaccinated or whose vaccination status was unknown. This year, the highly contagious disease has been reported at schools, airports and Disneyland.
Public health officials hope the West Coast Health Alliance can help counteract Trump by building trust through evidence-based public health guidance.
“What we’re seeing from the federal government is partisan politics at its worst and retaliation for policy differences, and it puts at extraordinary risk the health and well-being of the American people,” said Georges Benjamin, executive director of the American Public Health Assn., a coalition of public health professionals.
Robust vaccine schedule
Erica Pan, California’s top public health officer and director of the state Department of Public Health, said the West Coast Health Alliance is defending science by recommending a more robust vaccine schedule than the federal government. California is part of a coalition suing the Trump administration over its decision to rescind recommendations for seven childhood vaccines, including for hepatitis A, hepatitis B, influenza and COVID-19.
Pan expressed deep concern about the state of public health, particularly the uptick in measles. “We’re sliding backwards,” Pan said of immunizations.
Sarah Kemble, Hawaii’s state epidemiologist, said Hawaii joined the alliance after hearing from pro-vaccine residents who wanted assurance that they would have access to vaccines.
“We were getting a lot of questions and anxiety from people who did understand science-based recommendations but were wondering, ‘Am I still going to be able to go get my shot?’” Kemble said.
Other states led mostly by Democrats have also formed alliances, with Pennsylvania, New York, New Jersey, Massachusetts and several other East Coast states banding together to create the Northeast Public Health Collaborative.
Hilliard, of Health and Human Services, said that even as Democratic governors establish vaccine advisory coalitions, the federal Advisory Committee on Immunization Practices “remains the scientific body guiding immunization recommendations in this country, and HHS will ensure policy is based on rigorous evidence and gold standard science, not the failed politics of the pandemic.”
Influencing red states
Newsom, for his part, has approved a recurring annual infusion of nearly $300 million to support the state Department of Public Health, as well as the 61 local public health agencies across California, and last year signed a bill authorizing the state to issue its own immunization guidance. It requires health insurers in California to provide patient coverage for vaccinations the state recommends even if the federal government doesn’t.
Jeffrey Singer, a doctor and senior fellow at the libertarian Cato Institute, said decentralization can be beneficial. That’s because local media campaigns that reflect different political ideologies and community priorities may have a better chance of influencing the public.
A KFF analysis found some red states are joining blue states in decoupling their vaccine recommendations from the federal government’s. Singer said some doctors in his home state of Arizona are looking to more liberal California for vaccine recommendations.
“Science is never settled, and there are a lot of areas of this country where there are differences of opinion,” Singer said. “This can help us challenge our assumptions and learn.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling and journalism.
Science
How Rising Home Insurance Costs Are Linked to Credit Scores

Two friends bought nearly identical homes last year, in the same northern Minnesota neighborhood, for the same price.
But Tara Novak pays more than twice as much for home insurance as Petra Rodriguez. The only difference? Ms. Novak has a lower credit score.
Across the country, people with weaker credit histories are paying far more for home insurance than owners with spotless records.
Where the home insurance rate gap between “fair” and “excellent” credit is higher
Home insurance premiums have risen rapidly in recent years, fueled by climate change, building costs and inflation. The price shock has rippled into the real estate market, dragging down home prices in areas vulnerable to disasters and leading insurers to abandon homeowners in risky places.
But these dynamics obscure another problem: The home insurance market has cleaved in two along a boundary defined more by a customer’s personal history than by the risk of a disaster hitting their home.
Americans with weaker credit histories, usually from missed payments or high amounts of debt, now pay significantly more for insurance, regardless of where they live, two new studies have found. While those with poor credit histories often can’t purchase homes at all, people with “fair” scores, which range from around 580 to 669, are paying twice as much in some places as people with “excellent” scores of about 800 or higher. And the gap is growing.
Insurers use a metric based on credit history known as an insurance score to set rates, and the figure tracks closely with a customer’s credit score.
The penalty for having a “fair” credit history versus an “excellent” one
States with the biggest pricing gaps
That can mean owners of identical homes, like Ms. Novak and Ms. Rodriguez, pay wildly different rates to insure them. For most people, it’s now just as expensive to have a credit score of “fair” as it is to live in an area likely to experience a disaster like a hurricane or wildfire. About 29 percent of consumers have credit scores that are categorized as “fair” or “poor.”
“There’s so many reasons people have bad credit,” Ms. Novak said. “It’s not like I’ve ever not paid a bill on time. I’m a stickler on my bills, I’m a stickler on my rent, never been late. This is not fair.”
“The choice to use credit scores in pricing means that those lower-credit home owners in risky areas are effectively subsidizing more affluent high-credit homeowners who also live in risky areas,” said Nick Graetz, assistant professor of sociology at the University for Minnesota, who wrote one of the recent papers. “So in a lot of ways, you can keep your insurance price down if you’re high income, high credit — even if you live on the coast of Florida.”
A handful of states have banned insurers from using credit data because of concerns about fairness and the potential for discrimination against low-income people and people of color, but the majority allow it.
For those with both weaker credit and high disaster risk, the combination can set them up for a downward spiral: disasters tend to be followed by decreases in credit scores as people use credit cards and bank loans to recover. That can lead to higher insurance rates, pushing monthly housing costs further out of reach.
“When a disaster hits, there’s a loss of income that occurs, and then that can impact someone’s credit score because they can’t pay their debt, they can’t pay their rent, they can’t pay their mortgage,” said Lance Triggs, executive vice president at Operation HOPE, a financial literacy nonprofit. “And now they’re faced with higher insurance premiums post-disaster.”
A working paper released today by the National Bureau of Economic Research found that homeowners with the lowest credit scores paid, on average, $550 more in 2024 for home insurance than those with the highest scores.
The findings broadly track with data from Quadrant Information Services analyzed by The New York Times, which found that, on average, lower credit scores meant higher premiums across every state that allowed the practice. Dr. Graetz used the same data set for his research, which he did in collaboration with the Consumer Federation of America and the Climate and Community Institute.
When a windstorm last year hit the home of Audrey Thayer, a city council member in Bemidji, Minn., it ripped the siding off her house and stripped shingles from her roof.
Ms. Thayer’s insurance did not cover all the damage. As she fought her insurer for more money, she opened new credit cards and bank loans to repair her home. Her credit score dropped as she tried to find a new insurance plan.
Ms. Thayer, a member of the White Earth Nation, said she was not aware that her credit score could affect her home insurance rates, even though she teaches about credit ratings at a nearby tribal college. “Most of the folks here do not have good credit,” said Ms. Thayer, whose community is one of the poorest in the state. “I did not know what a credit score was until I was 35 or so.”
In Texas, the advocacy group Texas Appleseed found that some insurers charge people with poor credit up to 12 times as much as people with excellent credit for certain policies, said Ann Baddour, the director of the nonprofit’s Fair Financial Services Project.
Higher costs have serious implications for low-income homeowners who live in the path of hurricanes, said Nadia Erosa, the operations manager at Come Dream Come Build, a nonprofit community housing development organization. After the Brownsville, Texas, region saw intense flooding last spring, some residents turned to companies offering high-interest loans to fund repairs, she said, raising the risk of the disaster-credit spiral.
“Delinquencies are going up because people cannot afford their payment,” she said.
The price of risk
Before they can get a mortgage, homebuyers are usually required by lenders to purchase home insurance.
“Households with insurance have fewer financial burdens, fewer unmet needs, they recover faster, they’re more likely to rebuild,” said Carolyn Kousky, an economist and founder of Insurance for Good, a nonprofit that focuses on finding new approaches to risk management. “Yet the people who need insurance the most are the least able to afford it.”
Insurance companies consider a variety of factors when setting the premium for a property. They might examine the age of the roof, or the area’s vulnerability to hurricanes or wildfires. They factor in how much it would cost to rebuild the house if it were damaged.
Insurers have argued that credit history is also worth considering because people with low scores tend to file more claims than those with excellent scores, an assertion that is backed up by the working paper published in the National Bureau of Economic Research today. This likely happens because people with weaker credit histories tend to have less income, and when their home is damaged, they file insurance claims for smaller fixes that a wealthier homeowner might pay for out of pocket.
Paul Tetrault, senior director at the American Property Casualty Insurance Association, a trade organization, said credit scores are a valid way to price premiums.
But others argue that using credit information to price insurance doesn’t make sense.
Because a homeowner pays for insurance upfront, “it’s not like you’re really extending a loan to the customer where you would be worried about the risk of repayment,” Ms. Kousky said. She points out that insurance companies can opt not to renew a homeowner’s policy if they believe it is too risky — a tactic they have been using with increasing frequency.
The NBER analysis found that homeowners who want to pay less for insurance should pay off debt to raise their credit score rather than replace roofs and make other improvements to avoid damage when disaster strikes.
Others believe that even if credit scores are accurate predictors of future claims, they shouldn’t be used to set premiums because that can perpetuate or worsen disparities. For example, people in their mid-20s who are Black, low-income, or grow up in impoverished regions have significantly lower credit scores than their peers, a July working paper from Opportunity Insights, a not-for-profit organization at Harvard University, found.
“When the government and the financial system mandate that we buy a product, there’s a special obligation to make sure the pricing is fair,” said Doug Heller, director of insurance at the Consumer Federation. “To me that is an absolutely solid reason, just like we don’t allow pricing based on race or income or ethnicity or religion.”
A natural experiment
A handful of states, including California and Massachusetts, have banned or limited the use of credit scores in setting home insurance premiums, despite opposition from the insurance industry.
In Nevada, where a temporary pandemic-related rule prevented insurers from using credit history to increase premiums for existing customers from 2020 to 2024, companies refunded approximately $27 million to nearly 200,000 policyholders, said Drew Pearson, a spokesman for the Nevada Division of Insurance.
Perhaps the clearest example of the effects of these bans comes from Washington State, which banned the use of credit information in setting home insurance premiums starting in June 2021. The rule immediately faced legal challenges, and was in effect for just a few months until it was overturned in court.
But the episode allowed researchers to evaluate the effect of credit factors on insurance premiums. When the rule took effect, people with the lowest credit scores saw a decrease in premiums of about $175 annually while those with the highest scores saw an increase of about $100, the NBER analysis found.
“We could see the dynamics of insurance pricing for the same households over time,” said Benjamin Keys, a professor at the University of Pennsylvania’s Wharton School, who co-authored the paper.
What homeowners paid before and after a ban on credit-based pricing in Washington State
Values compared with premiums paid by homeowners with “medium” credit scores (717 to 756)
In Minnesota, where Tara Novak, Petra Rodriguez and Audrey Thayer live, a state task force looked at ways to lower insurance costs for residents. It recently considered a ban or limit on the use of credit scores to set rates, but did not move forward with a recommendation.
Ms. Rodriguez said she doesn’t think it’s fair that her friend Ms. Novak should have to pay so much more for insurance to live in an identical house.
A credit score doesn’t capture anything about a person’s habits, or what they’re like as a tenant, or even years of on-time rent payments, she said. “It’s not who you are,” she said.
Methodology
Home insurance policy rates were supplied by Quadrant Information Services, an insurance data solutions company. The rates shown are representative of publicly sourced filings and should not be interpreted as bindable quotes. Actual individual premiums may vary.
‘States with the biggest pricing gaps’Rates shown are based on a home insurance policy with $400,000 of dwelling coverage and a $100,000 liability limit on a new home, for a homeowner age 50 or younger. Rates are averaged for all the individual company filings represented in the sample, which add up to a majority of the market share in each state but do not cover all active insurers in the state. Rates are also averaged to the state level from zip code level data.
‘The credit penalty in each state’Each insurance company incorporates credit history information differently, often using proprietary methods, so the scores do not map directly to FICO credit scores.
‘What homeowners paid before and after a ban on credit-based pricing in Washington State’Data shown are based on observations of real home insurance policies and homeowner credit scores from ICE McDash analyzed by the researchers of Blonz, Hossain, Keys, Mulder and Weill (2026). The price comparisons across credit score tiers controlled for variance in disaster risk, insurance policy characteristics, geography, and other year to year fluctuations.
Science
Earth is warming faster than previously estimated, new study shows

Planetary warming has significantly accelerated over the past 10 years, with temperatures rising at a higher rate since 2015 than in any previous decade on record, a new study showed.
The Earth warmed around 0.35 degrees Celsius in the decade to 2025, compared to just under 0.2C per decade on average between 1970 and 2015, according to a paper published on Friday in the scientific journal Geophysical Research Letters. This is the first statistically significant evidence of an acceleration of global warming, the authors said.
The past three years have been the hottest on record, compared to the average before the Industrial Revolution. In 2024, warming went past 1.5C, the lower limit set by the Paris Agreement. That target refers to temperature increases over 20 years, but breaching it for one year shows efforts to slow down climate change have been insufficient, the scientists who wrote the new paper said.
The findings shed light on an ongoing debate among researchers. While there is consensus that greenhouse gas emissions have caused the planet to heat up since pre-industrial times, that warming had been steady for decades. But record-breaking temperatures in recent years have led scientists to question whether the pace of temperature gains is accelerating.
Demonstrating that was difficult due to natural fluctuations in temperatures. The researchers filtered out the “noise” to make the “underlying long-term warming signal” more clearly visible, said Grant Foster, a co-author of the study and a U.S.-based statistics expert.
Researchers isolated phenomena including the El Niño weather phase, volcanic eruptions and solar irradiance. When looking at temperature increases without their influence, the authors concluded the evidence is “strong” that the accelerated warming was not due to an unusually hot 2023 and 2024, but that since 2015 global temperatures departed from their previous, slower path of warming.
The new report adds to a growing body of work that indicates climate change is having a quicker and larger impact on the planet than scientists have understood. A separate paper published this week found that many studies on sea-level increases underestimate how much water along the coast has already risen.
“If the warming rate of the past 10 years continues, it would lead to a long-term exceedance of the 1.5C limit of the Paris Agreement before 2030,” said Stefan Rahmstorf, the lead author of the warming study and a researcher at the Potsdam Institute for Climate Impact Research. “How quickly the Earth continues to warm ultimately depends on how rapidly we reduce global CO2 emissions from fossil fuels to zero.”
Millan writes for Bloomberg.
-

 Wisconsin1 week ago
Wisconsin1 week agoSetting sail on iceboats across a frozen lake in Wisconsin
-

 Massachusetts1 week ago
Massachusetts1 week agoMassachusetts man awaits word from family in Iran after attacks
-

 Pennsylvania6 days ago
Pennsylvania6 days agoPa. man found guilty of raping teen girl who he took to Mexico
-

 Detroit, MI5 days ago
Detroit, MI5 days agoU.S. Postal Service could run out of money within a year
-

 Miami, FL7 days ago
Miami, FL7 days agoCity of Miami celebrates reopening of Flagler Street as part of beautification project
-

 Sports6 days ago
Sports6 days agoKeith Olbermann under fire for calling Lou Holtz a ‘scumbag’ after legendary coach’s death
-

 Virginia7 days ago
Virginia7 days agoGiants will hold 2026 training camp in West Virginia
-

 Culture1 week ago
Culture1 week agoTry This Quiz on the Real Locations in These Magical and Mysterious Novels


















