Science
Kids are sucking down baby food pouches at record rates. ‘We’re going to pay for it,’ experts say

Every week, Caitlin Scuttio stops by Target and piles her cart with pureed food pouches for her 4-year-old and twin 18-month-olds sons.
In goes a 24-pack of unsweetened applesauce. Then a 24-pack of the fruit and veggie blend. And finally, the yogurt pouches for her oldest son’s breakfast. “He’d eat six apple sauce pouches a day if I let him,” Scuttio said.
Total monthly pouch budget: $200.
“They have such a choke hold on my family. I can’t imagine our grocery list without it at this point,” she said. “We are definitely a pouch family.”
Sales of baby food pouches have increased 900% over the last decade. Pouches are now the most popular baby food on the market.
And they aren’t alone. Sales of food pouches — soft bags with plastic spouts for easy consumption — have increased 900% since 2010, overtaking jarred purees as the predominant baby food on the market. Parents generally spoon-feed jars of pureed foods for a few months in the first year of life when introducing solids, but pouches marketed to parents of toddlers and older children have prolonged pureed food eating by years.
While the occasional pouch can be part of a healthy diet, doctors and nutritionists are raising concerns that an overreliance on pouches can interfere with nutrition, long-term food preferences, dental hygiene and even speech and language development. And marketing practices can leave parents confused about what’s actually inside the packages.
“Pouches are highly processed foods,” said Dr. Steven Abrams, a professor of pediatrics at the University of Texas at Austin Dell Medical School. “They certainly serve as a quick snack, but we need to make sure that pouches don’t make up too much of a toddler’s diet. We want kids to learn to chew and eat foods like meat, and fruits and vegetables that are not processed.”

Heidi Martinez gathers baby food pouches for her three kids at their home in Pittsburg, Calif. She said she always buys the pouches with at least one vegetable.
What’s inside varies greatly — some contain only fruit, while others have a mix of vegetables, grains, yogurt and even meat. Whereas many jarred foods contain a single ingredient like pureed peas or carrots, pouches are more often a blend that features a sweet fruit such as apple or pear as the primary ingredient.
A 2019 study found that infant and toddler food in pouches contained significantly more sugar per serving than foods available in other forms of packaging.
To be sure, there is not an epidemic of children who don’t know how to chew. But Dr. Mark Corkins, a pediatric gastroenterologist at the University of Tennessee Health Science Center who chairs the American Academy of Pediatrics committee on nutrition, said he sometimes sees children who are so reliant on the smooth, sweet taste of pouches that they have developed food and texture aversions and refuse to eat regular fruits or vegetables.
“In the long run we’re going to pay for it,” he said.
Engage with our community-funded journalism as we delve into child care, transitional kindergarten, health and other issues affecting children from birth through age 5.
Why are baby food pouches so popular?
Pouches are convenient: Unlike glass jars, they don’t shatter when dropped and toddlers can suck down the slurry without help from a caregiver.

Pouches are convenient because they don’t shatter when dropped, and toddlers can suck down the slurry without help from a caregiver.
“It is so dang hard to be a parent of young children in the U.S. Having [pouches] on an airplane, having them in the car — it is so convenient that I would never take that away from parents. I used pouches with my children,” said Bridget Young, an associate professor of pediatrics at the University of Rochester School of Medicine.
“The industry has gone from jars to pouches because it’s more cost-effective and convenient,” said Dr. Tanya Altmann, a pediatrician in Calabasas and author of the book What to Feed Your Baby. But it’s what’s inside that’s important, and “not all pouches are created equal.”
As a tool, she said, pouches “can be a contributor to a family’s nutrition,” but not a prime source. Those without added sugars or salt may even have advantages over other processed snacks.
Heidi Martinez, a mother of three in Pittsburg, Calif., said she always buys the pouches with at least one vegetable. As her oldest son goes through “picky stages, I like that he is still getting some kale and beets,” she said. “I don’t know that they’re actually healthier but I feel better about it.”

Heidi Martinez plays with her sons while they eat from pouches. “I don’t know that they’re actually healthier but I feel better about it,” she said of pouches that include vegetables.
At the age of 7, he eats two to three pouches a day.
Manufacturers appeal to parents by marketing a pouch as “all natural,” “organic” or containing vegetables.
But the advertising on the front of a pouch doesn’t necessarily reflect what’s inside. A green pouch advertised as broccoli-pear might turn out to be little more than pear puree. And a pouch labeled something like turkey dinner “might be apple sauce with a whisper of turkey,” Young said. “And there’s nothing wrong with apple sauce. But there is something wrong when you think you’re feeding your child turkey.”
Parents of picky eaters may be particularly vulnerable to this kind of marketing.
“It’s kind of the perfect storm, when the child is transitioning to solids and trying new foods,” said Fran Fleming-Milici, director of marketing initiatives at the Rudd Center for Food Policy and Health at the University of Connecticut. “You’re not sure of the nutrition that the child is getting.
Martinez said the real appeal, however, is the pouch itself. She considers pouches to be in the same category as a smoothie or yogurt, but in an easy to-go form.

Ezekiel Martinez, 7, eats from a pouch while hanging upside down at a park. He eats two to three pouches a day.
The slippery slope of sweet, smooth purees
The early years of a child’s life are crucial for developing lifelong healthy eating habits. Babies are born with a preference for sweet foods, said Jill Castle, a pediatric dietitian in Massachusetts and author of the book “Kids Thrive at Every Size.” Typically, a child must be repeatedly introduced to various foods to get them used to different textures and flavors, such as the taste of vegetables.
It’s hard to beat the convenience of pouches — they’re easy to throw in a diaper bag or hand to a screaming toddler in the car. But experts warn relying on them too much could be a problem.
Fruit puree can disguise the taste of vegetables, reinforcing sweetness, Castle said.
If a child’s diet consists mostly of pouches, “when you actually give them chopped-up carrot and peas that roll around the plate, they’re not used to that at all,” and may refuse it, said Daisy Coyle, who researches pouches at the George Institute for Global Health in Sydney, Australia.
Ideally, lumpy textures should be introduced as early as possible so the child can learn to use their tongue and jaw to manipulate and swallow food, a process that requires 30 different muscles to work together, said Susan Greenberg, a speech pathologist at Children’s Hospital Los Angeles. “We think it’s a natural process, but it’s like learning to walk,” she said.
A variety of textures is also crucial to developing a child’s long-term food preferences. “If you prolong purees and don’t introduce lumpy foods by 10 months, we have evidence that by 15 months and even 7 years, it influences food acceptance,” Greenberg said.
The full sensory experience of eating food is also important, she added — getting messy, using spoons, fingers and tiny fists to squish food and smear on a highchair and face.

Lucas Martinez, 5, snacks while at a park.
Dentists also have concerns about what pouches mean for oral hygiene. Dr. Francisco Ramos-Gomez, director of the UCLA Center for Children’s Oral Health, said the way purees such as apple sauce stick to the teeth is different from eating an actual apple, and it sits on a child’s teeth before being washed. This prolonged exposure increases the acidity of the mouth, erodes the teeth and causes cavities.
But it’s all a matter of moderation, Greenberg said. “Pouches are easy, and we live in a world that’s really busy these days. I think we can all agree that it’s not a bad thing. It just can’t replace the other things.”
Do toddlers really need their own special food?
By about 12 months old, typically developing children do not need pureed food. “It was always a goal to get kids off of purees by 9 months and get them onto table food,” Castle said. “By 1 year, you’re sitting at the table with your family, and you’re eating what the whole family is eating.”
Toddlers and young children can eat most anything that an adult can eat, as long as it’s cut or prepared in a way that’s appropriate for their eating skills and doesn’t make it a choking hazard.
But brands have invented a whole new, lucrative category of toddler foods, from pouches and teething crackers to bars and puffs, Fleming-Milici said.
The major pouch manufacturers — including Gerber, Plum Organics and Happy Family Organics — did not respond to requests for comment from The Times.
In the last 12 months, American families have spent more than $466 million on baby food pouches, according to data from the market research firm NIQ.
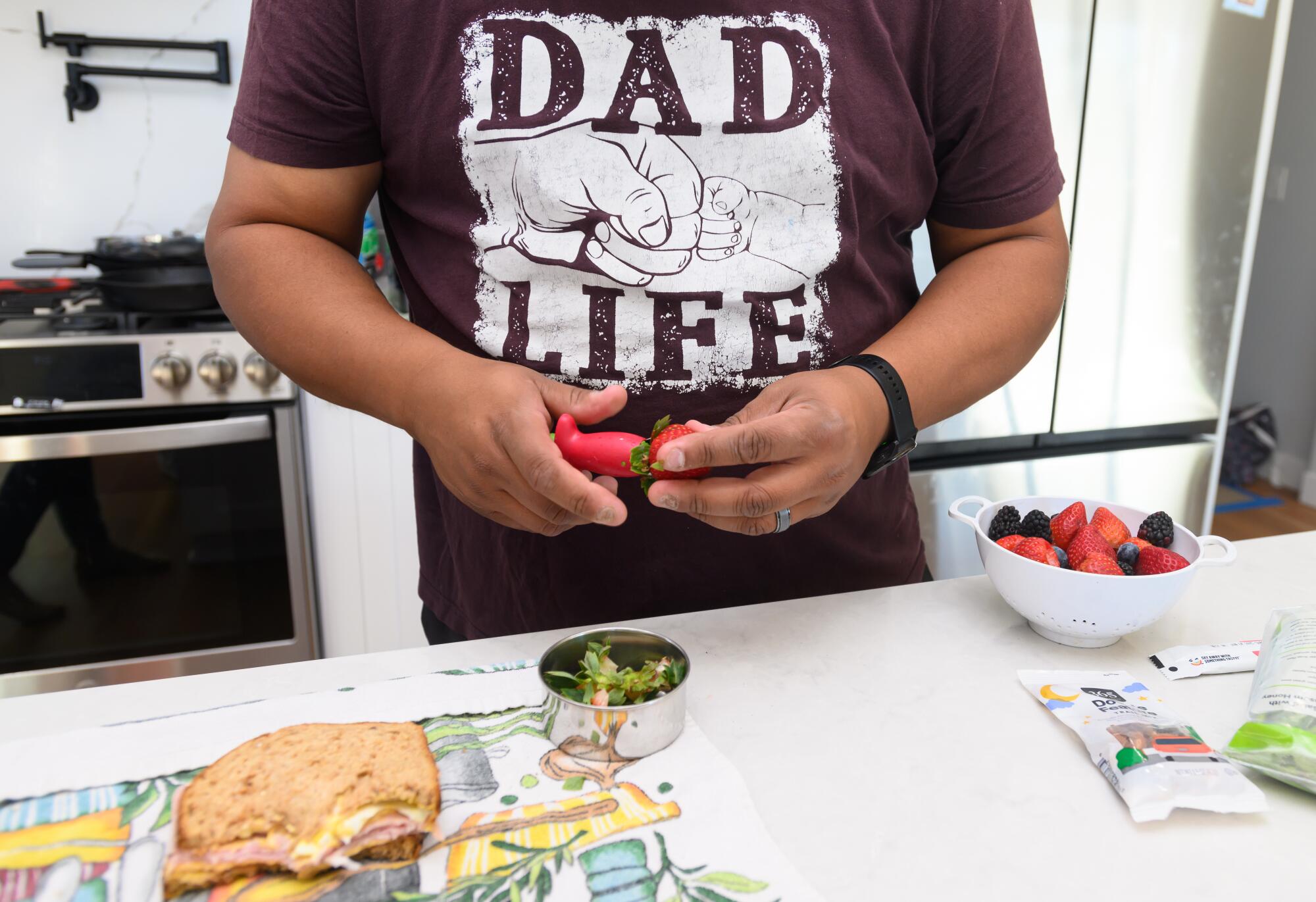
Mario Martinez prepares snacks for his three sons.
The “Wild West” of the baby food aisle
As opposed to the tightly regulated U.S. infant formula sector, baby and toddler foods do not have their own special marketing and production rules; they are subject to the same requirements as adult foods.
“The baby food market is like the Wild West,” Castle said.
The World Health Organization came up with its own nonbinding set of standards for baby food, which included limits on fat, sugar and sodium. It also requires clear labeling of ingredients and prohibits the use of health, nutrition and marketing claims on the packaging.
A study by Coyle earlier this year published in the journal Nutrients found 60% of the baby or toddler food products for sale at the top 10 grocery stores in the U.S. failed to meet the WHO nutritional recommendations. Almost all packages included at least one prohibited marketing claim, and some had as many as 11.
Earlier this year, the FDA recalled 3 million cinnamon applesauce pouches that contained extremely high levels of lead, after dozens of children across the United States were found to be suffering from lead poisoning. The FDA does not currently set heavy-metal limits or require baby food manufacturers to test for them.
“We really need to have some U.S.-based regulations, or decide we’re following the World Health Organization’s regulations. But there needs to be more tight control,” Castle said. “These are some of our youngest, most vulnerable members of our population.”
Instead of blaming families for overusing pouches, she said, new regulations, healthier ingredients that target key nutrients, and more transparent advertising are needed. “Even just having more pouches that are predominantly veggie based and less sweet would be a really positive change,” she said.

Lucas Martinez eats from a pouch. Manufacturers appeal to parents by marketing a pouch as “all natural,” “organic” or containing vegetables.
How to see through marketing pitches
To select the healthiest pouches, nutritionist Young recommends ignoring the advertising on the front of the package — including the name of the product.
Instead, flip to the back, where the ingredients are listed in order of how much is in the package, and look for pouches that list the veggies first. A pouch that lists apple first probably will be mostly applesauce.
Beth Saltz, a pediatric dietitian in Woodland Hills, said a general rule of thumb is to make sure that all of the ingredients listed could be sold in the grocery store. If the ingredients include things such as “organic tapioca starch” or “pea protein isolate,” or even natural coloring, you might reconsider.
“A little toddler does not need those,” she said.
This article is part of The Times’ early childhood education initiative, focusing on the learning and development of California children from birth to age 5. For more information about the initiative and its philanthropic funders, go to latimes.com/earlyed.

Science
A virus without a vaccine or treatment is hitting California. What you need to know

A respiratory virus that doesn’t have a vaccine or a specific treatment regimen is spreading in some parts of California — but there’s no need to sound the alarm just yet, public health officials say.
A majority of Northern California communities have seen high concentrations of human metapneumovirus, or HMPV, detected in their wastewater, according to data from the WastewaterScan Dashboard, a public database that monitors sewage to track the presence of infectious diseases.
A Los Angeles Times data analysis found the communities of Merced in the San Joaquin Valley, and Novato and Sunnyvale in the San Francisco Bay Area have seen increases in HMPV levels in their wastewater between mid-December and the end of February.
HMPV has also been detected in L.A. County, though at levels considered low to moderate at this point, data show.
While HMPV may not necessarily ring a bell, it isn’t a new virus. Its typical pattern of seasonal spread was upended by the COVID-19 pandemic, and its resurgence could signal a return to a more typical pre-coronavirus respiratory disease landscape.
Here’s what you need to know.
What is HMPV?
HMPV was first detected in 2001, according to the U.S. Centers for Disease Control and Prevention. It’s transmitted by close contact with someone who is infected or by touching a contaminated surface, said Dr. Neha Nanda, chief of infectious diseases and hospital epidemiologist for Keck Medicine of USC.
Like other respiratory illnesses, such as influenza, HMPV spreads and is more durable in colder temperatures, infectious-disease experts say.
Human metapneumovirus cases commonly start showing up in January before peaking in March or April and then tailing off in June, said Dr. Jessica August, chief of infectious diseases at Kaiser Permanente Santa Rosa.
However, as was the case with many respiratory viruses, COVID disrupted that seasonal trend.
Why are we talking about HMPV now?
Before the pandemic hit in 2020, Americans were regularly exposed to seasonal viruses like HMPV and developed a degree of natural immunity, August said.
That protection waned during the pandemic, as people stayed home or kept their distance from others. So when people resumed normal activities, they were more vulnerable to the virus. Unlike other viruses, there isn’t a vaccine for human metapneumovirus.
“That’s why after the pandemic we saw record-breaking childhood viral illnesses because we lacked the usual immunity that we had, just from lack of exposure,” August said. “All of that also led to longer viral seasons, more severe illness. But all of these things have settled down in many respects.”
In 2024, the national test positivity for HMPV peaked at 11.7% at the end of March, according to the National Respiratory and Enteric Virus Surveillance System. The following year’s peak was 7.15% in late April.
So far this year, the highest test positivity rate documented was 6.1%, reported on Feb. 21 — the most recent date for which complete data are available.
While the seasonal spread of viruses like HMPV is nothing new, people became more aware of infectious diseases and how to prevent them during the pandemic, and they’ve remained part of the public consciousness in the years since, August and Nanda said.
What are the symptoms of HMPV?
Most people won’t go to the doctor if they have HMPV because it typically causes mild, cold-like symptoms that include cough, fever, nasal congestion and sore throat.
HMPV infection can progress to:
- An asthma attack and reactive airway disease (wheezing and difficulty breathing)
- Middle ear infections behind the ear drum
- Croup, also known as “barking” cough — an infection of the vocal cords, windpipe and sometimes the larger airways in the lungs
- Bronchitis
- Fever
Anyone can contract human metapneumovirus, but those who are immunocompromised or have other underlying medical conditions are at particular risk of developing severe disease — including pneumonia. Young children and older adults are also considered higher-risk groups, Nanda said.
What is the treatment for HMPV?
There is no specified treatment protocol or antiviral medication for HMPV. However, it’s common for an infection to clear up on its own and treatment is mostly geared toward soothing symptoms, according to the American Lung Assn.
A doctor will likely send you home and tell you to rest and drink plenty of fluids, Nanda said.
If symptoms worsen, experts say you should contact your healthcare provider.
How to avoid contracting HMPV
Infectious-disease experts said the best way to avoid contracting HMPV is similar to preventing other respiratory illnesses.
The American Lung Assn.’s recommendations include:
- Wash your hands often with soap and water. If that’s not available, clean your hands with an alcohol-based hand sanitizer.
- Clean frequently touched surfaces.
- Crack open a window to improve air flow in crowded spaces.
- Avoid being around sick people if you can.
- Avoid touching your eyes, nose and mouth.
Assistant data and graphics editor Vanessa Martínez contributed to this report.
Science
After rash of overdose deaths, L.A. banned sales of kratom. Some say they lost lifeline for pain and opioid withdrawal

Nearly four months ago, Los Angeles County banned the sale of kratom, as well as 7-OH, the synthetic version of the alkaloid that is its active ingredient. The idea was to put an end to what at the time seemed like a rash of overdose deaths related to the drug.
It’s too soon to tell whether kratom-related deaths have dissipated as a result — or, really, whether there was ever actually an epidemic to begin with. But many L.A. residents had become reliant on kratom as something of a panacea for debilitating pain and opioid withdrawal symptoms, and the new rules have made it harder for them to find what they say has been a lifesaving drug.
Robert Wallace started using kratom a few years ago for his knees. For decades he had been in pain, which he says stems from his days as a physical education teacher for the Glendale Unified School District between 1989 and 1998, when he and his students primarily exercised on asphalt.
In 2004, he had arthroscopic surgery on his right knee, followed by varicose vein surgery on both legs. Over the next couple of decades, he saw pain-management specialists regularly. But the primary outcome was a growing dependence on opioid-based painkillers. “I found myself seeking doctors who would prescribe it,” he said.
He leaned on opioids when he could get them and alcohol when he couldn’t, resulting in a strain on his marriage.
When Wallace was scheduled for his first knee replacement in 2021 (he had his other knee replaced a few years later), his brother recommended he take kratom for the post-surgery pain.
It seemed to work: Wallace said he takes a quarter of a teaspoon of powdered kratom twice a day, and it lets him take charge of managing his pain without prescription painkillers and eases harsh opiate-withdrawal symptoms.
He’s one of many Angelenos frustrated by recent efforts by the county health department to limit access to the drug. “Kratom has impacted my life in only positive ways,” Wallace told The Times.
For now, Wallace is still able to get his kratom powder, called Red Bali, by ordering from a company in Florida.
However, advocates say that the county crackdown on kratom could significantly affect the ability of many Angelenos to access what they say is an affordable, safer alternative to prescription painkillers.
Kratom comes from the leaves of a tree native to Southeast Asia called Mitragyna speciosa. It has been used for hundreds of years to treat chronic pain, coughing and diarrhea as well as to boost energy — in low doses, kratom appears to act as a stimulant, though in higher doses, it can have effects more like opioids.
Though advocates note that kratom has been used in the U.S. for more than 50 years for all sorts of health applications, there is limited research that suggests kratom could have therapeutic value, and there is no scientific consensus.
Then there’s 7-OH, or 7-Hydroxymitragynine, a synthetic alkaloid derived from kratom that has similar effects and has been on the U.S. market for only about three years. However, because of its ability to bind to opioid receptors in the body, it has a higher potential for abuse than kratom.
Public health officials and advocates are divided on kratom. Some say it should be heavily regulated — and 7-OH banned altogether — while others say both should be accessible, as long as there are age limitations and proper labeling, such as with alcohol or cannabis.
In the U.S., kratom and 7-OH can be found in all sorts of forms, including powder, capsules and liquids — though it depends on exactly where you are in the country. Though the Food and Drug Administration has recommended that 7-OH be included as a Schedule 1 controlled substance under the Controlled Substances Act, that hasn’t been made official. And the plant itself remains unscheduled on the federal level.
That has left states, counties and cities to decide how to regulate the substances.
California failed to approve an Assembly bill in 2024 that would have required kratom products to be registered with the state, have labeling and warnings, and be prohibited from being sold to anyone younger than 21.
It would also have banned products containing synthetic versions of kratom alkaloids. The state Legislature is now considering another bill that basically does the same without banning 7-OH — while also limiting the amount of synthetic alkaloids in kratom and 7-OH products sold in the state.
“Until kratom and its pharmacologically active key ingredients mitragynine and 7-OH are approved for use, they will remain classified as adulterants in drugs, dietary supplements and foods,” a California Department of Public Health spokesperson previously told The Times.
On Tuesday, California Gov. Gavin Newsom announced that the state’s efforts to crack down on kratom products has resulted in the removal of more than 3,300 kratom and 7-OH products from retail stores. According to a news release from the governor’s office, there has been a 95% compliance rate from businesses in removing the products.
(Los Angeles Times photo illustration; source photos by Getty Images)
Newsom has equated these actions to the state’s efforts in 2024 to quash the sale of hemp products containing cannabinoids such as THC. Under emergency state regulations two years ago, California banned these specific hemp products and agents with the state Department of Alcoholic Beverage Control seized thousands of products statewide.
Since the beginning of 2026, there have been no reported violations of the ban on sales of such products.
“We’ve shown with illegal hemp products that when the state sets clear expectations and partners with businesses, compliance follows,” Newsom said in a statement. “This effort builds on that model — education first, enforcement where necessary — to protect Californians.”
Despite the state’s actions, the Los Angeles County Board of Supervisors is still considering whether to regulate kratom, or ban it altogether.
The county Public Health Department’s decision to ban the sale of kratom didn’t come out of nowhere. As Maral Farsi, deputy director of the California Department of Public Health, noted during a Feb. 18 state Senate hearing, the agency “identified 362 kratom-related overdose deaths in California between 2019 and 2023, with a steady increase from 38 in 2019 up to 92 in 2023.”
However, some experts say those numbers aren’t as clear-cut as they seem.
For example, a Los Angeles Times investigation found that in a number of recent L.A. County deaths that were initially thought to be caused by kratom or 7-OH, there wasn’t enough evidence to say those drugs alone caused the deaths; it might be the case that the danger is in mixing them with other substances.
Meanwhile, the actual application of this new policy seems to be piecemeal at best.
The county Public Health Department told The Times it conducted 2,696 kratom-related inspections between Nov. 10 and Jan. 27, and found 352 locations selling kratom products. The health department said the majority stopped selling kratom after those inspections; there were nine locations that ignored the warnings, and in those cases, inspectors impounded their kratom products.
But the reality is that people who need kratom will buy it on the black market, drive far enough so they get to where it’s sold legally or, like Wallace, order it online from a different state.
For now, retailers who sell kratom products are simply carrying on until they’re investigated by county health inspectors.
Ari Agalopol, a decorated pianist and piano teacher, saw her performances and classes abruptly come to a halt in 2012 after a car accident resulted in severe spinal and knee injuries.
“I tried my best to do traditional acupuncture, physical therapy and hydrocortisone shots in my spine and everything,” she said. “Finally, after nothing was working, I relegated myself to being a pain-management patient.”
She was prescribed oxycodone, and while on the medication, battled depression, anhedonia and suicidal ideation. She felt as though she were in a fog when taking oxycodone, and when it ran out, ”the pain would rear its ugly head.” Agalopol struggled to get out of bed daily and could manage teaching only five students a week.
Then, looking for alternatives to opioids, she found a Reddit thread in which people were talking up the benefits of kratom.
“I was kind of hesitant at first because there’re so many horror stories about 7-OH, but then I researched and I realized that the natural plant is not the same as 7-OH,” she said.
She went to a local shop, Authentic Kratom in Woodland Hills, and spoke to a sales associate who helped her decide which of the 47 strains of kratom it sold would best suit her needs.
Agalopol currently takes a 75-milligram dose of mitragynine, the primary alkaloid in kratom, when necessary. It has enabled her to get back to where she was before her injury: teaching 40 students a week and performing every weekend.
Agalopol believes the county hasn’t done its homework on kratom. “They’re just taking these actions because of public pressure, and public pressure is happening because of ignorance,” she said.
During the course of reporting this story, Authentic Kratom has shut down its three locations; it’s unclear if the closures are temporary. The owner of the business declined to comment on the matter.
When she heard the news of the recent closures, Agalopol was seething. She told The Times she has enough capsules of kratom for now, but when she runs out, her option will have to be Tylenol and ibuprofen, “which will slowly kill my liver.”
“Prohibition is not a public health strategy,” said Jackie Subeck, executive director of 7-Hope Alliance, a nonprofit that promotes safe and responsible access to 7-OH for consumers, at the Feb. 18 Senate hearing. “[It’s] only going to make things worse, likely resulting in an entirely new health crisis for Californians.”
Science
There were 13 full-service public health clinics in L.A. County. Now there are 6

Because of budget cuts, the Los Angeles County Department of Public Health has ended clinical services at seven of its public health clinic sites.
As of Feb. 27, the county is no longer providing services such as vaccinations, sexually transmitted infection testing and treatment, or tuberculosis diagnosis and specialty TB care at the affected locations, according to county officials and a department fact sheet.
The sites losing clinical services are Antelope Valley in Lancaster; the Center for Community Health (Leavy) in San Pedro, Curtis R. Tucker in Inglewood, Hollywood-Wilshire, Pomona, Dr. Ruth Temple in South Los Angeles, and Torrance. Services will continue to be provided by the six remaining public health clinics, and through nearby community clinics.
The changes are the result of about $50 million in funding losses, according to official county statements.
“That pushed us to make the very difficult decision to end clinical services at seven of our sites,” said Dr. Anish Mahajan, chief deputy director of the L.A. County Department of Public Health.
Mahajan said the department selected clinics with relatively lower patient volumes. Over the last month, he said, the department has sent letters to patients about the changes, and referred them to unaffected county clinics, nearby federally qualified health centers or other community providers. According to Mahajan, for tuberculosis patients, particularly those requiring directly observed therapy, public health nurses will continue visiting patients.
Public health clinics form part of the county’s healthcare safety net, serving low-income residents and those with limited access to care. Officials said that about half of the patients the county currently sees across its clinics are uninsured.
Mahajan noted that the clinics were established decades ago, before the Affordable Care Act expanded Medi-Cal coverage and increased the number of federally qualified health centers. He said that as more residents gained access to primary care, utilization at some county-run clinics declined.
“Now that we have a more sophisticated safety net, people often have another place to go for their full range of care,” he said.
Still, the closures have unsettled providers who work closely with local vulnerable populations.
“I hate to see any services that serve our at-risk and homeless community shut down,” said Mark Hood, chief executive of Union Rescue Mission in downtown Los Angeles. “There’s so much need out there, so it always is going to create hardship for the people that actually need the help the most.”
Union Rescue Mission does not receive government funding for its healthcare services, Hood said. The mission’s clinics are open not only to shelter guests, up to 1,000 people nightly, but also to people living on the streets who walk in seeking care.
Its dental clinic alone sees nearly 9,000 patients a year, Hood said.
“We haven’t seen it yet, but I expect in the coming days and weeks we’ll see more people coming through our doors looking for help,” he said. “They’re going to have to find help somewhere.” Hood said women experiencing homelessness are especially vulnerable when preventive care, including sexual and reproductive health services, becomes harder to access.
County officials said staffing impacts so far have been managed through reassignment rather than layoffs. Roughly 200 to 300 positions across the department have been eliminated amid funding cuts, officials said, though many were vacant. About 120 employees whose positions were affected have been reassigned; according to Mahajan, no one has been laid off.
The clinic closures come amid broader fiscal uncertainty. Mahajan said that due to the Trump administration’s “Big Beautiful Bill,” Los Angeles County could lose $2.4 billion over the next several years. That funding, he said, supports clinics, hospitals and community clinic partners now absorbing patients who previously went to the clinics that closed on Feb. 27.
In response, the L.A. County Board of Supervisors has backed a proposed half-cent sales tax measure that would generate hundreds of millions of dollars annually for healthcare and public health services. Voters are expected to consider the measure in June.
-

 World1 week ago
World1 week agoExclusive: DeepSeek withholds latest AI model from US chipmakers including Nvidia, sources say
-

 Massachusetts1 week ago
Massachusetts1 week agoMother and daughter injured in Taunton house explosion
-

 Wisconsin3 days ago
Wisconsin3 days agoSetting sail on iceboats across a frozen lake in Wisconsin
-

 Maryland4 days ago
Maryland4 days agoAM showers Sunday in Maryland
-

 Denver, CO1 week ago
Denver, CO1 week ago10 acres charred, 5 injured in Thornton grass fire, evacuation orders lifted
-

 Florida4 days ago
Florida4 days agoFlorida man rescued after being stuck in shoulder-deep mud for days
-

 Massachusetts2 days ago
Massachusetts2 days agoMassachusetts man awaits word from family in Iran after attacks
-

 Oregon6 days ago
Oregon6 days ago2026 OSAA Oregon Wrestling State Championship Results And Brackets – FloWrestling





















