Science
A new COVID subvariant spreads rapidly as Trump pivots away from vaccines
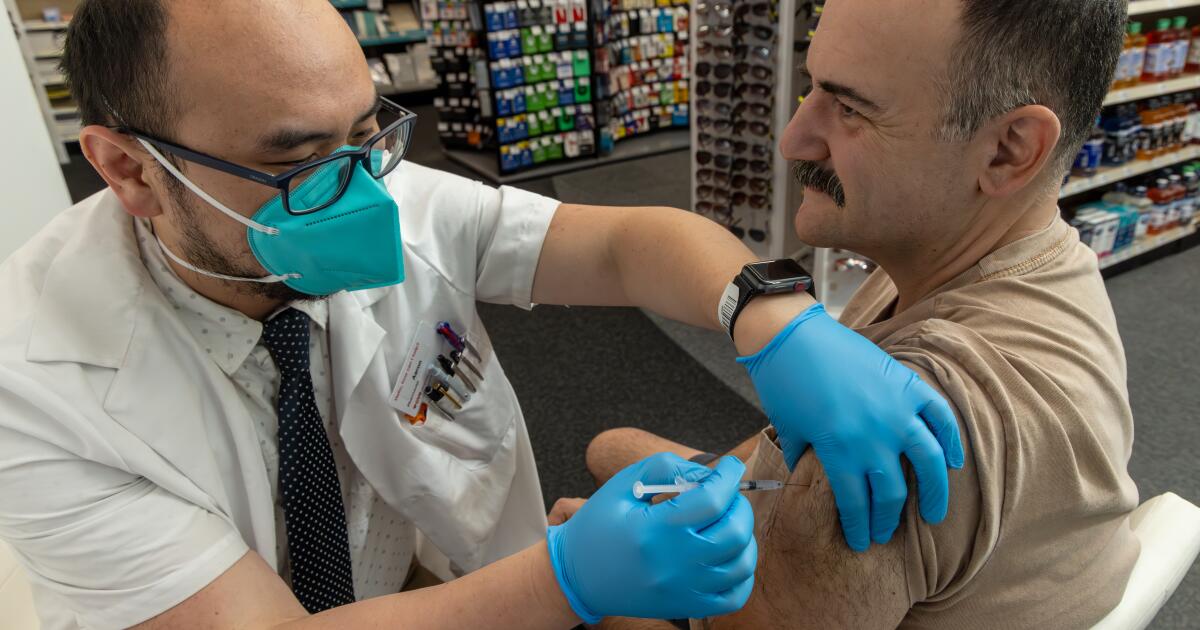
A new, highly transmissible COVID subvariant has been detected in California — heightening the risk of a potential summer wave as recent moves by the Trump administration threaten to make vaccines harder to get, and more expensive, for many Americans, some health experts warn.
Health and Human Services Secretary Robert F. Kennedy Jr. announced this week that he was rescinding the federal government’s recommendation that pregnant women and healthy children get immunized against COVID, effective immediately.
Dr. Marty Makary, commissioner of the U.S. Food and Drug Administration, also said the agency will no longer routinely approve annually formulated COVID-19 vaccinations for healthy people under age 65.
“We simply don’t know whether a healthy 52-year-old woman with a normal BMI who has had COVID-19 three times and has received six previous doses of a COVID-19 vaccine will benefit from the seventh dose,” Makary, along with another FDA official, Dr. Vinay Prasad, wrote in the New England Journal of Medicine this month. “This policy will compel much-needed evidence generation.”
However, some experts say mandating more extensive testing could delay vaccine access for many, as those efforts may not even be complete until after the end of the upcoming winter flu-and-COVID season.
“Pregnant women, infants and young children are at higher risk of hospitalization from COVID, and the safety of the COVID vaccine has been widely demonstrated,” Dr. Sean O’Leary, chair of the American Academy of Pediatrics’ Committee on Infectious Diseases, said in a statement.
The U.S. Centers for Disease Control and Prevention has said that, in general, getting an updated vaccine provides children and adults additional protection from COVID-related emergency room and urgent care visits.
The recent federal changes, according to some experts, could also prompt private insurance companies and government insurers to stop paying for COVID shots for wide segments of the population, including babies and children.
Absent a recommendation by federal officials, Americans could end up paying the entire cost of a vaccine, experts say. The out-of-pocket cost for a COVID vaccine at CVS, for instance, is $198.99.
Although the emergency phase of the pandemic has long since passed, authorities note COVID remains a public health concern. A relatively new subvariant has been spreading in Europe and Asia, “particularly Hong Kong, Taiwan, other countries, Japan, etc.,” said Dr. Peter Chin-Hong, a UC San Francisco infectious diseases expert.
That subvariant, NB.1.8.1, was first documented in January and has since been detected in California, including in Los Angeles County and the San Francisco Bay Area. The World Health Organization designated it a “Variant Under Monitoring” last week.
NB.1.8.1 has grown exponentially worldwide in recent weeks. The Omicron subvariant represented 10.7% of genetically analyzed viral samples worldwide for the week ending April 27, WHO data show. That was up sharply from the week ending April 6, when the subvariant accounted for 2.5% of samples worldwide.
“While still low numbers, this is a significant rise,” the WHO said, adding that there was a “concurrent increase in cases and hospitalizations in some countries where NB.1.8.1 is widespread.”
NB.1.8.1 isn’t yet prevalent enough in the United States to be publicly tracked by the CDC. Another strain, LP.8.1, accounted for an estimated 73% of coronavirus specimens nationally for the two-week period ending Saturday.
Data suggest NB.1.8.1 does not cause more severe illness, “but it is more transmissible, at least from what we’re seeing around the world and also from lab experiments,” said Dr. Yvonne Maldonado, an infectious-disease expert at Stanford University.
In Taiwan, a top health official told reporters that an NB.1.8.1-fueled outbreak was “continuing to rise rapidly, with a sustained increase in severe and fatal cases,” the Central News Agency reported, prompting a shortage of COVID testing kits. Health officials said a factor in Taiwan’s surge was the lack of a major COVID wave over the winter, and forecast that the island’s current spike may not peak for another four to six weeks.
NB.1.8.1 has seen increased prevalence in each of the three WHO regions that still consistently share genetic analysis of COVID samples — the Western Pacific (which includes East Asia, parts of Southeast Asia, and Australia); Europe; and the Americas.
The rate at which COVID tests are coming back positive in Los Angeles County has slightly increased over the past few weeks, although the overall positive rate remains low, at 3.5%, according to the county Department of Public Health. Coronavirus levels detected in the county’s wastewater have increased by 6% in the last three weeks, but also remain relatively low and are about one-eighth of the peak in the summer of last year.
Although California experienced a mild winter season — a first of the COVID era — that followed a powerful summer spike that was the strongest in years.
Many experts and officials have touted available COVID vaccines as effective both in warding off infection and in lessening the severity of symptoms. However, the need for otherwise healthy individuals to roll up their sleeves has been a matter of debate.
In a video message Tuesday on X, Kennedy — a noted vaccine skeptic — said that he “couldn’t be more pleased to announce that, as of today, the COVID vaccine for healthy children and healthy pregnant women has been removed from the CDC recommended immunization schedule.”
Experts said they could not recall a time when a political appointee circumvented a well-established process of making vaccine recommendations, which typically involves panels of scientists advising the FDA and CDC.
“It’s kind of chilling,” Chin-Hong said. “It’s out of step with the system we’ve learned to trust and follow.”
In a statement to The Times, the L.A. County Department of Public Health urged Kennedy to listen to experts in the field — including from the CDC’s Advisory Committee on Immunization Practices, which is scheduled to meet next month — “before decreasing access to any vaccine.”
As of Thursday, the CDC still had the long-standing vaccine recommendations on its website: Everyone ages 6 months and older should get the most recent COVID-19 vaccine, officially known as the 2024-25 version, which was introduced in September. The CDC also recommends seniors ages 65 and up get a second vaccine dose six months after their first.
In a statement, the California Department of Public Health said that it supports the current expansive recommendation for COVID vaccines, and that it “will continue to follow the federal conversation through this dynamic situation.”
“Staying up to date with COVID-19 vaccination can reduce the risk of disease, especially more severe cases that result in hospitalization or death,” the department added.
The Washington Post reported Wednesday that the CDC did not know of Kennedy’s directive until he posted it, and officials have been “scrambling to find out what it meant.”
Experts who spoke with The Times warned the practical effect of the edict — if it becomes official — could be far more costly vaccines for affected groups.
“If vaccines are not recommended by the CDC, insurance companies would NOT be required to cover the cost,” the L.A. County Department of Public Health said in a statement.
As a result, the vaccines may be less accessible to healthier people who still want them — perhaps because they live or work with elderly or other higher-risk people, they’ve had severe COVID illness before, or they want to protect themselves against the latest subvariant, the agency said.
If the FDA withholds a license for an updated COVID vaccination for younger, healthier adults, this group “would not be able to receive it unless their provider chooses to give it ‘off label,’” the county said.
When asked whether healthy pregnant women and healthy children can still get vaccinated at its pharmacies, Walgreens said its teams operate “in full compliance with applicable laws.” CVS said its locations “follow federal guidance regarding vaccine administration and are monitoring any changes that the government may make regarding vaccine eligibility.”
Kaiser Permanente Southern California said it was aware of potential changes, but noted no new formal guidance has yet been issued. As a result, Kaiser is continuing to follow existing guidance, which recommends the shots for everyone.
The L.A. County Department of Public Health said that as of Wednesday, “pregnant women and healthy children can get vaccinated for COVID-19,” according to existing recommendations from an advisory panel and the CDC.
Chin-Hong noted there were 150 pediatric deaths in the U.S. from COVID-19 in a recent one-year period. That’s in the same ballpark as the 231 pediatric flu deaths recorded this season, and federal health officials recommend everyone ages 6 months and older get an annual flu shot.
“Most people would agree that kids should be targeted for flu vaccines. It seems kind of weird to have COVID as an outlier in that respect,” Chin-Hong said.
In the video published this week, Makary said that “most countries in the world have stopped recommending the vaccine for children.”
Maldonado, however, said the U.S. doesn’t use other nations’ standards to dictate vaccine recommendations. The U.S., for instance, recommends other types of vaccines that have a lower prevalence than COVID that people want to get, Maldonado said, such as the meningococcal vaccine for children to guard against a serious bacterial disease that can infect the brain and spinal cord and cause death within hours.
The effect of a recommendation also varies by country. Canada, for instance, recommends updated COVID vaccines for seniors and other people who meet certain criteria, such as if they’re pregnant or are a healthcare worker. But the country’s universal healthcare system still allows everyone ages 6 months and older to get an updated COVID vaccine.
Although it’s true that children overall are at lower risk of developing severe COVID illness, those under 6 months of age “have the same risk of complications as the 65-year-old-plus population in this country,” said Stanford’s Maldonado, who also serves on the CDC’s Advisory Committee on Immunization Practices.
Among children eligible for vaccination, COVID-associated hospitalization rates are highest for those ages 6 months to 4 years, according to the CDC.
“So are children going to be the highest risk group? No, they’re not. But would you want to protect your child from a disease that could potentially put them in the hospital and get them on a ventilator? Yes, I would say that I would want to make that choice for myself. And why not allow the parent to make that choice?” Maldonado said.
The CDC says COVID vaccination during pregnancy builds antibodies that can help protect the baby; studies have also shown that vaccinated moms who breastfeed have protective antibodies in their milk, which could help protect their babies.
There have been an estimated 260,000 to 430,000 hospitalizations attributed to COVID since October, causing “an enormous burden on the healthcare system,” Dr. Fiona Havers, a medical epidemiologist with the CDC, said at a recent public meeting. There have also been an estimated 30,000 to 50,000 COVID-19 deaths over the same time period.
“It is a major cause of morbidity and mortality, particularly in older adults, but it does affect other people, particularly those with underlying conditions, in younger age groups.”
COVID is also a major cause of pediatric hospitalizations, even among otherwise healthy children, she said.
“If there’s a summer wave this year, we’ll be seeing it in children being hospitalized with COVID as well,” she said.

Science
Commentary: My toothache led to a painful discovery: The dental care system is full of cavities as you age

I had a nagging toothache recently, and it led to an even more painful revelation.
If you X-rayed the state of oral health care in the United States, particularly for people 65 and older, the picture would be full of cavities.
“It’s probably worse than you can even imagine,” said Elizabeth Mertz, a UC San Francisco professor and Healthforce Center researcher who studies barriers to dental care for seniors.
Mertz once referred to the snaggletoothed, gap-filled oral health care system — which isn’t really a system at all — as “a mess.”
But let me get back to my toothache, while I reach for some painkiller. It had been bothering me for a couple of weeks, so I went to see my dentist, hoping for the best and preparing for the worst, having had two extractions in less than two years.
Let’s make it a trifecta.
My dentist said a molar needed to be yanked because of a cellular breakdown called resorption, and a periodontist in his office recommended a bone graft and probably an implant. The whole process would take several months and cost roughly the price of a swell vacation.
I’m lucky to have a great dentist and dental coverage through my employer, but as anyone with a private plan knows, dental insurance can barely be called insurance. It’s fine for cleanings and basic preventive routines. But for more complicated and expensive procedures — which multiply as you age — you can be on the hook for half the cost, if you’re covered at all, with annual payout caps in the $1,500 range.
“The No. 1 reason for delayed dental care,” said Mertz, “is out-of-pocket costs.”
So I wondered if cost-wise, it would be better to dump my medical and dental coverage and switch to a Medicare plan that costs extra — Medicare Advantage — but includes dental care options. Almost in unison, my two dentists advised against that because Medicare supplemental plans can be so limited.
Sorting it all out can be confusing and time-consuming, and nobody warns you in advance that aging itself is a job, the benefits are lousy, and the specialty care you’ll need most — dental, vision, hearing and long-term care — are not covered in the basic package. It’s as if Medicare was designed by pranksters, and we’re paying the price now as the percentage of the 65-and-up population explodes.
So what are people supposed to do as they get older and their teeth get looser?
A retired friend told me that she and her husband don’t have dental insurance because it costs too much and covers too little, and it turns out they’re not alone. By some estimates, half of U.S. residents 65 and older have no dental insurance.
That’s actually not a bad option, said Mertz, given the cost of insurance premiums and co-pays, along with the caps. And even if you’ve got insurance, a lot of dentists don’t accept it because the reimbursements have stagnated as their costs have spiked.
But without insurance, a lot of people simply don’t go to the dentist until they have to, and that can be dangerous.
“Dental problems are very clearly associated with diabetes,” as well as heart problems and other health issues, said Paul Glassman, associate dean of the California Northstate University dentistry school.
There is one other option, and Mertz referred to it as dental tourism, saying that Mexico and Costa Rica are popular destinations for U.S. residents.
“You can get a week’s vacation and dental work and still come out ahead of what you’d be paying in the U.S.,” she said.
Tijuana dentist Dr. Oscar Ceballos told me that roughly 80% of his patients are from north of the border, and come from as far away as Florida, Wisconsin and Alaska. He has patients in their 80s and 90s who have been returning for years because in the U.S. their insurance was expensive, the coverage was limited and out-of-pocket expenses were unaffordable.
“For example, a dental implant in California is around $3,000-$5,000,” Ceballos said. At his office, depending on the specifics, the same service “is like $1,500 to $2,500.” The cost is lower because personnel, office rent and other overhead costs are cheaper than in the U.S., Ceballos said.
As we spoke by phone, Ceballos peeked into his waiting room and said three patients were from the U.S. He handed his cellphone to one of them, San Diegan John Lane, who said he’s been going south of the border for nine years.
“The primary reason is the quality of the care,” said Lane, who told me he refers to himself as 39, “with almost 40 years of additional” time on the clock.
Ceballos is “conscientious and he has facilities that are as clean and sterile and as medically up to date as anything you’d find in the U.S.,” said Lane, who had driven his wife down from San Diego for a new crown.
“The cost is 50% less than what it would be in the U.S.,” said Lane, and sometimes the savings is even greater than that.
Come this summer, Lane may be seeing even more Californians in Ceballos’ waiting room.
“Proposed funding cuts to the Medi-Cal Dental program would have devastating impacts on our state’s most vulnerable residents,” said dentist Robert Hanlon, president of the California Dental Assn.
Dental student Somkene Okwuego smiles after completing her work on patient Jimmy Stewart, 83, who receives affordable dental work at the Ostrow School of Dentistry of USC on the USC campus in Los Angeles on February 26, 2026.
(Genaro Molina / Los Angeles Times)
Under Proposition 56’s tobacco tax in 2016, supplemental reimbursements to dentists have been in place, but those increases could be wiped out under a budget-cutting proposal. Only about 40% of the state’s dentists accept Medi-Cal payments as it is, and Hanlon told me a CDA survey indicates that half would stop accepting Medi-Cal patients and many others will accept fewer patients.
“It’s appalling that when the cost of providing healthcare is at an all-time high, the state is considering cutting program funding back to 1990s levels,” Hanlon said. “These cuts … will force patients to forgo or delay basic dental care, driving completely preventable emergencies into already overcrowded emergency departments.”
Somkene Okwuego, who as a child in South L.A. was occasionally a patient at USC’s Herman Ostrow School of Dentistry clinic, will graduate from the school in just a few months.
I first wrote about Okwuego three years ago, after she got an undergrad degree in gerontology, and she told me a few days ago that many of her dental patients are elderly and have Medi-Cal or no insurance at all. She has also worked at a Skid Row dental clinic, and plans after graduation to work at a clinic where dental care is free or discounted.
Okwuego said “fixing the smiles” of her patients is a privilege and boosts their self-image, which can help “when they’re trying to get jobs.” When I dropped by to see her Thursday, she was with 83-year-old patient Jimmy Stewart.
Stewart, an Army veteran, told me he had trouble getting dental care at the VA and had gone years without seeing a dentist before a friend recommended the Ostrow clinic. He said he’s had extractions and top-quality restorative care at USC, with the work covered by his Medi-Cal insurance.
I told Stewart there could be some Medi-Cal cuts in the works this summer.
“I’d be screwed,” he said.
Him and a lot of other people.
steve.lopez@latimes.com
Science
Diablo Canyon clears last California permit hurdle to keep running

Central Coast Water authorities approved waste discharge permits for Diablo Canyon nuclear plant Thursday, making it nearly certain it will remain running through 2030, and potentially through 2045.
The Pacific Gas & Electric-owned plant was originally supposed to shut down in 2025, but lawmakers extended that deadline by five years in 2022, fearing power shortages if a plant that provides about 9 percent the state’s electricity were to shut off.
In December, Diablo Canyon received a key permit from the California Coastal Commission through an agreement that involved PG&E giving up about 12,000 acres of nearby land for conservation in exchange for the loss of marine life caused by the plant’s operations.
Today’s 6-0 vote by the Central Coast Regional Water Board approved PG&E’s plans to limit discharges of pollutants into the water and continue to run its “once-through cooling system.” The cooling technology flushes ocean water through the plant to absorb heat and discharges it, killing what the Coastal Commission estimated to be two billion fish each year.
The board also granted the plant a certification under the Clean Water Act, the last state regulatory hurdle the facility needed to clear before the federal Nuclear Regulatory Commission (NRC) is allowed to renew its permit through 2045.
The new regional water board permit made several changes since the last one was issued in 1990. One was a first-time limit on the chemical tributyltin-10, a toxic, internationally-banned compound added to paint to prevent organisms from growing on ship hulls.
Additional changes stemmed from a 2025 Supreme Court ruling that said if pollutant permits like this one impose specific water quality requirements, they must also specify how to meet them.
The plant’s biggest water quality impact is the heated water it discharges into the ocean, and that part of the permit remains unchanged. Radioactive waste from the plant is regulated not by the state but by the NRC.
California state law only allows the plant to remain open to 2030, but some lawmakers and regulators have already expressed interest in another extension given growing electricity demand and the plant’s role in providing carbon-free power to the grid.
Some board members raised concerns about granting a certification that would allow the NRC to reauthorize the plant’s permits through 2045.
“There’s every reason to think the California entities responsible for making the decision about continuing operation, namely the California [Independent System Operator] and the Energy Commission, all of them are sort of leaning toward continuing to operate this facility,” said boardmember Dominic Roques. “I’d like us to be consistent with state law at least, and imply that we are consistent with ending operation at five years.”
Other board members noted that regulators could revisit the permits in five years or sooner if state and federal laws changes, and the board ultimately approved the permit.
Science
Deadly bird flu found in California elephant seals for the first time

The H5N1 bird flu virus that devastated South American elephant seal populations has been confirmed in seals at California’s Año Nuevo State Park, researchers from UC Davis and UC Santa Cruz announced Wednesday.
The virus has ravaged wild, commercial and domestic animals across the globe and was found last week in seven weaned pups. The confirmation came from the U.S. Department of Agriculture’s National Veterinary Services Laboratory in Ames, Iowa.
“This is exceptionally rapid detection of an outbreak in free-ranging marine mammals,” said Professor Christine Johnson, director of the Institute for Pandemic Insights at UC Davis’ Weill School of Veterinary Medicine. “We have most likely identified the very first cases here because of coordinated teams that have been on high alert with active surveillance for this disease for some time.”
Since last week, when researchers began noticing neurological and respoiratory signs of the disease in some animals, 30 seals have died, said Roxanne Beltran, a professor of ecology and evolutionary biology at UC Santa Cruz. Twenty-nine were weaned pups and the other was an adult male. The team has so far confirmed the virus in only seven of the dead pups.
Infected animals often have tremors convulsions, seizures and muscle weakness, Johnson said.
Beltran said teams from UC Santa Cruz, UC Davis and California State Parks monitor the animals 260 days of the year, “including every day from December 15 to March 1” when the animals typically come ashore to breed, give birth and nurse.
The concerning behavior and deaths were first noticed Feb. 19.
“This is one of the most well-studied elephant seal colonies on the planet,” she said. “We know the seals so well that it’s very obvious to us when something is abnormal. And so my team was out that morning and we observed abnormal behaviors in seals and increased mortality that we had not seen the day before in those exact same locations. So we were very confident that we caught the beginning of this outbreak.”
In late 2022, the virus decimated southern elephant seal populations in South America and several sub-Antarctic Islands. At some colonies in Argentina, 97% of pups died, while on South Georgia Island, researchers reported a 47% decline in breeding females between 2022 and 2024. Researchers believe tens of thousands of animals died.
More than 30,000 sea lions in Peru and Chile died between 2022 and 2024. In Argentina, roughly 1,300 sea lions and fur seals perished.
At the time, researchers were not sure why northern Pacific populations were not infected, but suspected previous or milder strains of the virus conferred some immunity.
The virus is better known in the U.S. for sweeping through the nation’s dairy herds, where it infected dozens of dairy workers, millions of cows and thousands of wild, feral and domestic mammals. It’s also been found in wild birds and killed millions of commercial chickens, geese and ducks.
Two Americans have died from the virus since 2024, and 71 have been infected. The vast majority were dairy or commercial poultry workers. One death was that of a Louisiana man who had underlying conditions and was believed to have been exposed via backyard poultry or wild birds.
Scientists at UC Santa Cruz and UC Davis increased their surveillance of the elephant seals in Año Nuevo in recent years. The catastrophic effect of the disease prompted worry that it would spread to California elephant seals, said Beltran, whose lab leads UC Santa Cruz’s northern elephant seal research program at Año Nuevo.
Johnson, the UC Davis researcher, said the team has been working with stranding networks across the Pacific region for several years — sampling the tissue of birds, elephant seals and other marine mammals. They have not seen the virus in other California marine mammals. Two previous outbreaks of bird flu in U.S. marine mammals occurred in Maine in 2022 and Washington in 2023, affecting gray and harbor seals.
The virus in the animals has not yet been fully sequenced, so it’s unclear how the animals were exposed.
“We think the transmission is actually from dead and dying sea birds” living among the sea lions, Johnson said. “But we’ll certainly be investigating if there’s any mammal-to-mammal transmission.”
Genetic sequencing from southern elephant seal populations in Argentina suggested that version of the virus had acquired mutations that allowed it to pass between mammals.
The H5N1 virus was first detected in geese in China in 1996. Since then it has spread across the globe, reaching North America in 2021. The only continent where it has not been detected is Oceania.
Año Nuevo State Park, just north of Santa Cruz, is home to a colony of some 5,000 elephant seals during the winter breeding season. About 1,350 seals were on the beach when the outbreak began. Other large California colonies are located at Piedras Blancas and Point Reyes National Sea Shore. Most of those animals — roughly 900 — are weaned pups.
It’s “important to keep this in context. So far, avian influenza has affected only a small proportion of the weaned at this time, and there are still thousands of apparently healthy animals in the population,” Beltran said in a press conference.
Public access to the park has been closed and guided elephant seal tours canceled.
Health and wildlife officials urge beachgoers to keep a safe distance from wildlife and keep dogs leashed because the virus is contagious.
-

 World3 days ago
World3 days agoExclusive: DeepSeek withholds latest AI model from US chipmakers including Nvidia, sources say
-

 Massachusetts3 days ago
Massachusetts3 days agoMother and daughter injured in Taunton house explosion
-

 Montana1 week ago
Montana1 week ago2026 MHSA Montana Wrestling State Championship Brackets And Results – FloWrestling
-

 Louisiana6 days ago
Louisiana6 days agoWildfire near Gum Swamp Road in Livingston Parish now under control; more than 200 acres burned
-

 Denver, CO3 days ago
Denver, CO3 days ago10 acres charred, 5 injured in Thornton grass fire, evacuation orders lifted
-

 Technology1 week ago
Technology1 week agoYouTube TV billing scam emails are hitting inboxes
-

 Technology1 week ago
Technology1 week agoStellantis is in a crisis of its own making
-

 Politics1 week ago
Politics1 week agoOpenAI didn’t contact police despite employees flagging mass shooter’s concerning chatbot interactions: REPORT




















