Health
Addiction complicates pain management, but new guidelines offer help for ‘complex patients’

Opioids are often prescribed for pain management after surgery — but for the 19 million people in the U.S. with a history of substance abuse, that option may not be safe or desired.
Until now, there hasn’t been a cohesive set of guidelines for managing surgical pain in patients with a history of addiction and/or opioid tolerance.
To address this, the American Society of Anesthesiologists (ASA) gathered 15 medical organizations representing over 500,000 physicians to develop seven guiding principles to improve pain management before, during and after surgery for these patients.
The guidelines have been published in the Regional Anesthesia & Pain Medicine journal.
FOR ACUTE LOWER BACK PAIN, THESE ARE THE BEST MEDICATIONS, NEW STUDY FINDS
Dr. David Dickerson, an anesthesiologist and pain specialist at North Shore University Hospital in Chicago, Illinois, has had a leadership role on the ASRA Pain Medicine Committee for several years. (ASRA is the American Society of Regional Anesthesia and Pain Medicine.)
“Patients with these complex issues may require additional care after surgery,” Dickerson told Fox News Digital.
Opioids are often prescribed for pain management after surgery — but for the 19 million people in the U.S. with a history of substance abuse, that may not be a safe or desired option. Now, a new set of guidelines may help. (iStock)
“When someone undergoes a surgical procedure and they have a substance use disorder, chronic pain or pre-operative opioid tolerance, their nervous system is different,” he told Fox News Digital in an interview.
“Their ability to self-soothe in the face of injury or pain is also going to be a very different experience.”
TAKE THESE 5 SMART STEPS TO RELIEVE MUSCULOSKELETAL PAIN
As the director of four hospitals, Dickerson sees patients with many different types of pain in many different care environments. It’s why he’s calling for adopting a unified approach for patients who may not have a straightforward experience with pain management when it comes to surgery, injury, trauma or disease.
“Their ability to self-soothe in the face of injury or pain is also going to be a very different experience.”
“We want to make sure the patient has a consistent experience in terms of getting pain alleviated and also minimizing the risks of pain treatments,” he said.
Over a span of several years, Dickerson and other pain management specialists and physicians crafted the following seven principles to use as a “north star” for screening, treating and educating these vulnerable patients, while building awareness and education for safe and effective surgical care.
1. Identify patients at risk
Physicians should “screen for substance abuse preoperatively, risk stratify and refer for treatment as needed,” the first principle states.
The doctor should speak with the patient prior to surgery to determine whether there is any history of substance abuse, identify any risk factors and provide recommendations for referrals as needed.
“Clinicians should identify patients with a substance use disorder and facilitate evaluation and treatment before surgery.”
“As the majority of patients receive a post-surgery opioid prescription and 100,000 Americans die annually from accidental opioid overdose, clinicians should identify patients with a substance use disorder and facilitate evaluation and treatment before surgery,” Dickerson told Fox News Digital.
“Identifying and treating substance use disorders saves lives — especially when we recognize that 19 million Americans have at least one substance use disorder.”
2. Coordinate care for complex patients
“Coordinate care pre–operatively for complex patients and consult with pain medicine, behavioral health or addiction medicine specialists to optimize the treatment plan,” the second principle states.
This entails a multidisciplinary approach to patient care. This is when multiple health care professionals come together to define the appropriate treatment plan for an at-risk patient.

Until now, there hasn’t been a cohesive set of guidelines for managing surgical pain in patients with a history of chronic pain, addiction and/or opioid tolerance. (iStock)
“Patients with these complex issues may require additional care after surgery,” Dickerson said.
“A team of experts can plan and coordinate care that can help avoid a rocky surgical experience.”
3. Make a plan for patients already on opioids
This principle states: “For opioid-tolerant patients, coordinate and plan with the opioid prescriber to continue the home regimen; supplement analgesics perioperatively as needed.”
“Opioid-tolerant” patients are those who have been taking an opioid drug on a regular basis, resulting in the need for larger amounts to achieve the same effect.
CANCER CENTERS ARE SUFFERING MAJOR SHORTAGE OF POPULAR CHEMO DRUGS
“Patients taking opioids for weeks before surgery should not stop their opioids unless directed to do so, and clinicians should work to have a plan that avoids undertreating pain through using additional pain medications,” Dickerson said.
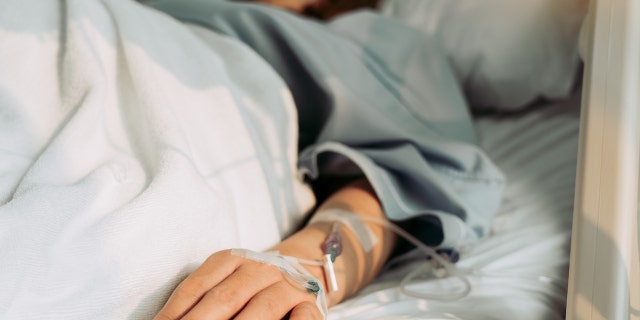
“Patients shouldn’t have to suffer after surgery with uncontrolled pain or awful medication side effects like nausea, vomiting, itching or constipation,” Dr. Dickerson said. (iStock)
In some cases, it may be necessary to continue home medications at pre-surgery doses to avoid withdrawal symptoms and a rough recovery, he noted.
“More opioids after surgery isn’t always the ideal option, either,” Dickerson added.
“There are many non-opioid therapies that are added to the home regimen to provide relief.”
4. Prescribe the lowest amount of opioids necessary
This principle states, “For opioid-tolerant patients, return to preoperative opioid dose or lower as soon as possible with an individualized tapering plan.”
In the event that an opioid-tolerant patient needs to increase the dose for post-surgery pain, the guidelines call for using the lowest necessary dose.
“Patients and their caregivers should know how to identify and respond to side effects before injury or harm occurs.”
If pre-surgery doses are increased after surgery for pain relief, those extra doses should be reduced as soon as possible as the patient heals, Dickerson said.
“This is often an individualized process, tailored to the patient’s day-to-day experience and recovery,” he added. “It is necessary to avoid creating even more significant opioid tolerance and dependence.”
5. Educate parents and caregivers
This principle says: “Educate patients and caregivers about opioid risks, how to recognize and treat respiratory depression, avoiding sedatives and alcohol, and when to call for help.”
While opioids can reduce pain, they also present specific risks and side effects that patients and their families should watch for, Dickerson said.
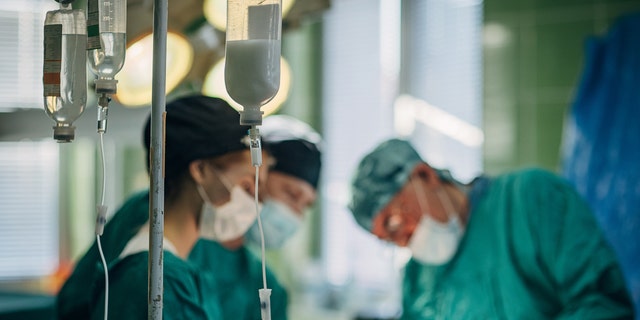
The new guidelines call for a multidisciplinary approach to patient care, in which multiple health care professionals come together to define the appropriate treatment plan for an at-risk patient. (iStock)
Additionally, he warned that alcohol and other sedatives should be avoided while taking opioids.
“Patients and their caregivers should know what to watch for and how to identify and respond to side effects before injury or harm occurs,” he said.
Some patients may be prescribed naloxone, an opioid antidote that can be given to reverse the effects of an overdose, Dickerson explained. Naloxone nasal spray can now be obtained by anyone without a prescription as an over-the-counter medication.
6. Consult with a pain specialist to provide relief as needed
“If adverse drug effects or uncontrolled pain occur, consult with a pain specialist or anesthesiologist,” this principle states.
WEIGHT LOSS SURGERIES ON THE RISE AMONG KIDS AND TEENS, STUDY FINDS: ‘ALTERING THE ANATOMY’
“Patients shouldn’t have to suffer after surgery with uncontrolled pain or awful medication side effects like nausea, vomiting, itching or constipation,” Dickerson said.
“Anesthesiologists and other pain specialists can provide additional treatments and therapies to reduce pain and the burden of side effects.”
He also said, “We have to work together to help patients have access to this team-based care.”
7. Use telehealth as needed
“If expert consultation is needed but in-person evaluation is not available, utilize telehealth to access pain medicine, behavioral health or addiction medicine,” states this principle.
Not all hospitals or clinicians have access to dedicated specialists in addiction or pain medicine, noted Dickerson. In scenarios where an in-person visit isn’t possible, the guidelines recommend relying on telehealth evaluation and consultations.

In scenarios where in-person evaluation is not available, the principles call for using telehealth to access pain medicine, behavioral health or addiction medicine. (iStock)
“We have to find a way to connect in-need patients and clinicians with help in a timely fashion and make sure patients without technology access or tech literacy still can connect with the care they need,” said Dickerson.
‘A step in the right direction’
Dr. Chris Tuell, clinical director of addiction services at the Lindner Center of HOPE at the University of Cincinnati College of Medicine, was not involved in creating the seven principles. He said he believes they are “a good start” and “a step in the right direction.”
He told Fox News Digital in an emailed statement, “We know that continuity of care and communication is essential in providing quality health care. Good treatment begins with good screening and assessment.”
“Continuity of care and communication is essential in providing quality health care.”
Given the fact that 83% of the individuals with substance use disorders also have a co-occurring mental health issue (per the Substance Abuse and Mental Health Services Administration), Tuell emphasized the need to coordinate care between the patient and his or her opioid prescriber and to create an individualized treatment plan.
“These principles stress the importance of the education of the patient and the caregiver,” he said. “Understanding the risks of opioids, and the dangers of utilizing alcohol or sedatives as a means of dealing with the adverse side effects of opioids, is essential.”
Non-opioid pain management options
In situations when someone in recovery cannot use opioids, Tuell said behavioral strategies — such as hypnotherapy, meditation and dialectical behavioral therapy — can be used to help manage pain.

Hypnotherapy is one option for non-opioid pain treatment. (iStock)
“I have utilized hypnotherapy with patients to assist in the regulation of pain when opioids were not an option,” said Tuell.
“Additionally, the use of teletherapy has provided therapy services for many underserved individuals who are residing in rural communities in which services are not readily available.”
Real patients’ stories
Dr. Lea McMahon, a licensed professional counselor, chief clinical officer at Symetria Recovery in Houston, Texas, and an adjunct professor of psychology at Columbia College, has helped many patients and people in recovery who have had to have surgery.
One patient at Symetria’s Chicago office, Ralph, 36 (he did not share his last name), became addicted to OxyContin after having surgery following a motorcycle accident in 2016.
BE WELL: TAKE THESE 5 SMART STEPS TO RELIEVE MUSCULOSKELETAL PAIN
After five years of addiction, he was in recovery for two years when he twisted his ankle in a stairwell in November 2022.
“He was already suffering a little from joint soreness before this, but he didn’t want to go back under the knife, as the pain was manageable,” said McMahon.
“However, this new injury meant he could hardly bear weight on the ankle for over a month, so he decided to have the surgery.”
Ralph had arthroscopic surgery to remove the excess scar tissue from the first operation and remove the build-up of debris.

In some cases, it may be necessary to continue home medications at pre-surgery doses to avoid withdrawal symptoms and a rough recovery, Dr. Dickerson said. (iStock)
“After a discussion with his health care provider and surgeon, it was decided to perform the operation under local general anesthetic, as with general anesthesia the entire body is in a state of deep sedation, which can increase inflammation and postoperative pain compared to local anesthesia,” McMahon said.
After the operation, Ralph’s pain medication was minimal, and he preferred to take less than recommended.
He used Advil for inflammation and could swap it out for Motrin if the pain level persisted.
Another patient, Indie (no last name given), spent 10 years addicted to heroin. She was in recovery for four years.
CLICK HERE TO SIGN UP FOR OUR HEALTH NEWSLETTER
When she suffered a burst appendix and was rushed to the ER in Houston, Texas, her sponsor shared her recovery status with the medical team and urged them not to give her any pain medications before the operation. Since it was an emergency, Indie was given a general anesthetic before surgery.
“After the procedure, her sponsor and family liaised with the medical team to keep her in the hospital for a few extra days,” McMahon said. “Barring any complications, patients can leave in one or two days, but this was extended to a week, so the hospital could monitor and manage Indie’s pain medication safely.”

“Patients with these complex issues may require additional care after surgery,” Dickerson explained. “A team of experts can plan and coordinate care that can help avoid a rocky surgical experience.” (iStock)
The pain medication was administered throughout a 24-span to temper the severity of the pain she was suffering.
“Self-administering of painkillers usually means the patient takes tablets when the pain starts to become unbearable, and this can then result in them looking elsewhere for stronger, more dangerous drugs,” McMahon explained.
“The use of around-the-clock dosing suppressed the pain and provided better comfort for Indie.”
Over the next seven days, the medication intervals remained the same, but the dose was gradually reduced.
After she was discharged, Indie was given a week’s supply of Tylenol and a non-opioid analgesic — and was instructed to call her physician twice a week to share her pain levels.

Health
C.D.C. Cuts Threaten to Set Back the Nation’s Health, Critics Say

The extensive layoffs of federal health workers that began on Tuesday will greatly curtail the scope and influence of the Centers for Disease Control and Prevention, the world’s premier public health agency, an outcome long sought by conservatives critical of its handling of the Covid-19 pandemic.
The reorganization of the Department of Health and Human Services shrinks the C.D.C. by 2,400 employees, or roughly 18 percent of its work force, and strips away some of its core functions.
Some Democrats in Congress described the reorganization throughout H.H.S. as flatly illegal.
“You cannot decimate and restructure H.H.S. without Congress,” said Senator Patty Murray, Democrat of Washington, and a member of the Senate health committee.
“This is not only unlawful but seriously harmful — they are putting Americans’ health and well-being on the line,” she added.
Ms. Murray noted that the Trump administration had not detailed which units are being cut at the C.D.C. and other health agencies. Robert F. Kennedy Jr., the health secretary, said last week the layoffs would affect primarily administrative functions.
But according to information gathered by The New York Times from dozens of workers, the reductions were more broadly targeted. Scientists focused on environmental health and asthma, injuries, lead poisoning, smoking and climate change were dismissed.
Researchers studying blood disorders, violence prevention and access to vaccines were let go. The agency’s center on H.I.V. and sexually transmitted diseases was among the hardest hit, losing about 27 percent of its staff.
The National Institute for Occupational Safety and Health, which makes recommendations on how to keep workers safe, was all but dissolved.
What remains is a hobbled C.D.C., with a smaller global footprint, devoting fewer resources to environmental health, occupational health and disease prevention, public health experts said.
Instead, the agency will be trained more narrowly on domestic disease outbreaks. Communications will be centralized at H.H.S. in Washington.
The department intends “to ensure a more coordinated and effective response to public health challenges, ultimately benefiting the American taxpayer,” said Emily Hilliard, deputy press secretary at the department.
“C.D.C. scientists have conducted numerous interviews on a variety of topics and will continue to do so,” she added.
Critics predicted the move would prevent scientists from speaking frankly about public health.
“American taxpayers provide the resources for C.D.C.’s specialists and have the right to hear directly from them without interference by politicians,” said Dr. Thomas R. Frieden, who led the agency from 2009 to 2017.
The sweeping reductions arrive as the nation confronts an outbreak of measles in Texas and elsewhere, a spreading bird flu epidemic on poultry and dairy farms, and a raft of new questions about public health measures like water fluoridation and school vaccine requirements.
“What we seem to be seeing is a dismantling rather than a restructuring” of the public health system, said Dr. Richard Besser, chief executive of the Robert Wood Johnson Foundation and a former acting director of the C.D.C.
On Capitol Hill, the Senate health committee, which recommended confirmation of Mr. Kennedy as secretary, scheduled a hearing on the reorganization of H.H.S., citing the possible impacts on public health.
Mr. Kennedy has described the reorganization as an effort to clean up waste and bureaucracy while promising that federal health agencies would do more to improve the health of Americans.
“We’re going to eliminate an entire alphabet soup of departments and agencies while preserving their core functions by merging them into a new organization called the Administration for a Healthy America,” the secretary said in a videotaped message announcing the layoffs.
The department did not respond to requests for more detailed information.
Society’s most vulnerable — the poor, Black, Latino and Native American people, rural Americans with less access to health care, the disabled and those at highest risk for illness — are likely to be hit hardest, experts said.
“These communities rely on public health to a larger extent than wealthy communities do,” Dr. Besser said.
For decades, public health and medical research drew support across the political spectrum.
But the C.D.C. has been in the political cross hairs since the first Trump administration, when the White House muzzled the agency’s communications, meddled with its publications and blamed its scientists for bungling the pandemic response.
In recent years, lawmakers have harshly criticized the agency’s advice on masks, lockdowns, social distancing, school closures and various other attempts to contain the pandemic, calling them economically and socially disastrous.
Project 2025, the conservative blueprint for reshaping the federal government, described the C.D.C. as “perhaps the most incompetent and arrogant” federal agency, and called on Congress to curb its powers.
Through staffing cuts, the administration reduced critical divisions of the National Center for Injury Prevention and Control, and employees studying how to prevent gun violence, child abuse and elder abuse were fired.
Injuries are the leading cause of death among Americans under 45. About 47,000 Americans are killed by firearms each year, more than half of them suicides.
But gun violence is a politically fraught topic. Pressure from the National Rifle Association and conservative politicians led to a ban on using federal funds to study gun violence for almost 25 years. Funding was restored in 2019.
The injury center studied ways to improve gun safety and promoted the use of gun locks, particularly in homes where children live.
“People think of gun violence as a question for law enforcement, but the public health approach has made a big difference,” said Dr. Mark Rosenberg, a former center director.
Most of the C.D.C.’s Division of Reproductive Health, which studies maternal health, was also shuttered. Whether some or all of its portfolio will be assumed by the new organization created by Mr. Kennedy was not clear.
Pregnant women and newborns die in the United States at a far higher rate than in other industrialized nations.
In recent years, the C.D.C. focused on stark racial health disparities that put Black American women at nearly three times the risk of dying of pregnancy complications than white women.
But the Trump administration has been defunding studies of health disparities in racial, ethnic and gender minorities, saying they do not align with the president’s executive orders ending diversity, equity and inclusion initiatives.
Mr. Kennedy said last week that the National Institute for Occupational Safety and Health, which makes recommendations for preventing work-related injuries and illnesses, would be absorbed into the health department.
But on Tuesday, most of its divisions were eliminated, among them offices dedicated to protecting workers in various industries, including mine inspectors.
Even one of the agency’s most essential functions, infectious disease research, was affected.
The Trump administration had been weighing moving the H.I.V. prevention division to a different agency within the health department.
But on Tuesday, teams leading H.I.V. surveillance and research within that division were laid off. It was unclear whether some of those functions would be recreated elsewhere. (A team in the global health center working on preventing mother-to-child transmission of H.I.V. was also cut.)
Until now, the C.D.C. provided funds to states and territories for responding to and preventing H.I.V. outbreaks. Roughly one in four new diagnoses of H.I.V. is made with agency funds.
Some H.I.V. experts warned that the move could lead to a rise in H.I.V. infections among Americans.
“H.I.V. prevention is a lot more than just giving out condoms,” said Dr. John Brooks, who served as chief medical officer for the division of H.I.V. prevention until last year. “It saves lives, averts illness and produces enormous cost savings.”
Broadly, the reorganization aligns with Mr. Kennedy’s preferred emphasis on research into chronic diseases; federal research has been far too focused on infectious diseases, he has said.
But the line between them is not always clear, said Dr. Anne Schuchat, former principal deputy director of the C.D.C. Research that seems disconnected from outbreak response may also be a key for fighting pathogens.
“For Zika, we needed experts in birth defects, entomology and vector control, virologists and environmental health experts,” she said. “Emerging threats don’t respect borders of C.D.C. organizational units.”
The reorganization risks choking the talent pipeline for public health, said Ursula Bauer, former director of the agency’s National Center for Chronic Disease Prevention and Health Promotion.
“Once you decimate an agency like C.D.C., which is full of high-caliber highly trained individuals, building back is going to be incredibly difficult,” she said.
“It will take two to three times as long to undo the damage as it took to inflict it.”
The cuts also will take a toll on the agency’s ability to gather and analyze data, which are keys to identifying trends and developing interventions, Dr. Phil Huang, director of Dallas County Health and Human Services, said at a news briefing.
“You take away those systems, and it takes away the ability to see the impact of all these cuts,” he added.
Health
Death probe of ex-Yankee's son triggers carbon monoxide warnings from experts

Experts are speaking out about the potential dangers attached to carbon monoxide, as authorities continue to probe the death of teen Miller Gardner, son of former New York Yankees player Brett Gardner.
While the cause of Miller Gardner’s death remains unconfirmed, Costa Rican Judicial Investigative Agency (OIJ) General Director Randall Zúñiga told reporters at a press conference on Monday that high levels of carbon monoxide contamination were found in the Gardner family’s hotel room, and that it might have caused the teen’s death.
“Which then leads us towards a line of investigation in which it seems that this person could have died from inhaling these very dangerous gases,” Zúñiga said.
Zúñiga said investigators who work on a specialized dangerous atmospheres team detected “high emissions of pollution of…carbon monoxide” in the room at Costa Rica’s Arenas Del Mar Beachfront & Rainforest Resort, which is where the Gardners were staying.
Officials at the hotel are denying the carbon monoxide claims.
DEATH OF EX-YANKEE’S SON IN COSTA RICA HAS EXPERTS SOUNDING ALARM ON HEALTHY TRAVEL
“The levels in the hotel room were non-existent and non-lethal. There was an error in this initial reporting. As mentioned, we await for conclusive results to confirm the cause of this unfortunate death,” a hotel spokesperson told Fox News Digital.
The spokesperson also said the room has been “closed off out of an abundance of precaution.”
Miller Gardner, 14, is photographed with his father, Brett Gardner, a former New York Yankee. Miller Gardner died last month in Costa Rica. His death is currently being investigated. (Courtesy of New York Yankees)
Dr. Nicole Saphier, a Fox News medical contributor, said no parent should ever have to endure the tragedy of losing a child.
In regard to carbon monoxide, she said the gas is “a silent, deadly threat.”
“We often focus on smoke alarms, but carbon monoxide is colorless, odorless and can overcome a person before they even realize what’s happening,” Saphier told Fox News Digital.
Saphier said every household should have multiple functioning carbon monoxide detectors, especially near sleeping areas.
For more Health articles, visit www.foxnews.com/health
“When we travel — whether staying at a hotel, Airbnb, or even in an RV — it’s worth considering bringing a portable carbon monoxide monitor for added protection,” she suggested.

The death of Miller Gardner, son of former New York Yankee Brett Gardner, has experts speaking out about carbon monoxide after the teen died while on vacation in Costa Rica. (AP Photo/Seth Wenig)
Dr. Marc Siegel, clinical professor of medicine at NYU Langone Health and a Fox News senior medical analyst, said, “symptoms can come on rapidly within minutes or hours and can include headache, nausea, fatigue, dizziness and vomiting.”
If you experience symptoms that you think could be from carbon monoxide poisoning, the Environmental Protection Agency recommends opening doors and windows, turning off combustion appliances and leaving the building.
CLICK HERE TO SIGN UP FOR OUR HEALTH NEWSLETTER
Siegel said prompt treatment with oxygen can sometimes reverse carbon monoxide poisoning.

Between 2009 and 2019, deaths from non-fire-related carbon monoxide poisoning have been on the rise, according to a new report released by the CPSC. (iStock)
“It is absolutely shocking to me that it took this long to be disclosed as a likely cause of death, when they could have done a test for carbon monoxide in [Miller Gardener’s] blood within hours during his autopsy weeks ago,” Siegel told Fox News Digital.
Between 2009 and 2019, deaths from non-fire-related carbon monoxide poisoning were on the rise, according to a report released by the U.S. Consumer Product Safety Commission (CPSC) in March 2023.
Fox News Digital reached out to OIJ in Costa Rica for additional comment.
Health
Federal Health Workers Make Up Less Than 1% of Agency Spending

A few days ago, Robert F. Kennedy Jr., the health secretary, embarked on a media tour to defend his decision to lay off thousands of his department’s workers.
He announced a plan last week to cut 10,000 jobs, in addition to the estimated 10,000 jobs cut through retirements and buyouts in the early weeks of the Trump administration.
Mr. Kennedy had called the Health and Human Services Department “the biggest agency in government, twice the size of the Pentagon, $1.9 trillion dollars,” during an interview with NewsNation. He went on to suggest that the department was doing little to improve the health of Americans, “with all the money that was being thrown at it, with all the personnel that were being brought in.”
H.H.S. does spend more than the Department of Defense, which has a discretionary budget of about $850 billion. But according to several budget experts, the overwhelming majority of the H.H.S. department’s $1.8 trillion budget is not spent on its staff.
Spending on personnel at the federal health agencies accounts for a small fraction of its budget — less than 1 percent, according to three budget experts. That includes the staff of the Food and Drug Administration, the Centers for Disease Control and Prevention, the National Institutes of Health and others.
The overwhelming majority of the money is spent through Medicare, for the health care of people older than 65, or through Medicaid, for people with low incomes. Those funds filter out to hospitals, clinics, nursing homes, dialysis centers, pharmaceutical companies, medical device makers and Medicare Advantage private insurance plans.
Melinda Buntin, professor of health policy and economics at Johns Hopkins University, said the $17.6 billion in costs for H.H.S. employees made up less than 1 percent of the department’s budget, and has risen in line with overall spending.
“I think that most people would be surprised by what a small share of Health and Human Services spending is for personnel, both their wages and compensation and benefits,” she said, noting that it made sense in the context of the agency’s spending on care.
Bobby Kogan, senior director of federal budget policy at the Center for American Progress, a left-leaning think tank, said Mr. Kennedy’s framing was “incredibly misleading.”
“It would leave someone with a super wrong understanding of what is going on really,” Mr. Kogan said. “The only story of what’s going on in H.H.S. is that we have a huge increase in the elderly population.”
An H.H.S. spokesman said the work force reductions are meant to cut $1.8 billion a year in federal spending, and that the amount is significant.
The Administration for Children and Families, another agency within H.H.S., also spends billions of dollars on services to the public. It operates Head Start programs, foster care, Temporary Assistance for Needy Families, formerly known as welfare, and care homes for unaccompanied minors from other countries.
Chris Towner, policy director for the Committee for a Responsible Federal Budget, made his own calculation, also concluding that H.H.S. staff costs appeared to be shy of 1 percent of the department’s spending. The figure could be slightly higher, he said, given the number of health agency workers with advanced degrees.
So far, the Trump administration has talked about fraud in the federal government repeatedly — though not the type that’s long been a target in Congress. Lawmakers have repeatedly raised the idea of reeling in Medicare Advantage insurance plans, which were estimated to overcharge Medicare by tens of billions of dollars a year.
-

 News1 week ago
News1 week agoTrump Is Trying to Gain More Power Over Elections. Is His Effort Legal?
-

 News1 week ago
News1 week agoWashington Bends to RFK Jr.’s ‘MAHA’ Agenda on Measles, Baby Formula and French Fries
-

 News1 week ago
News1 week agoCompanies Pull Back From Pride Events as Trump Targets D.E.I.
-

 World1 week ago
World1 week agoAt least six people killed in Israeli attacks on southern Syria
-

 Technology1 week ago
Technology1 week agoTrump officials planned a military strike over Signal – with a magazine editor on the line
-

 Technology1 week ago
Technology1 week agoThe FBI launched a task force to investigate Tesla attacks
-

 World1 week ago
World1 week agoNo, Norway and Sweden haven't banned digital transactions
-

 Culture1 week ago
Culture1 week agoAnalysing Jamal Musiala’s bizarre corner goal for Germany against Italy




















