Science
More parents are delaying their kids’ vaccines, and it’s alarming pediatricians
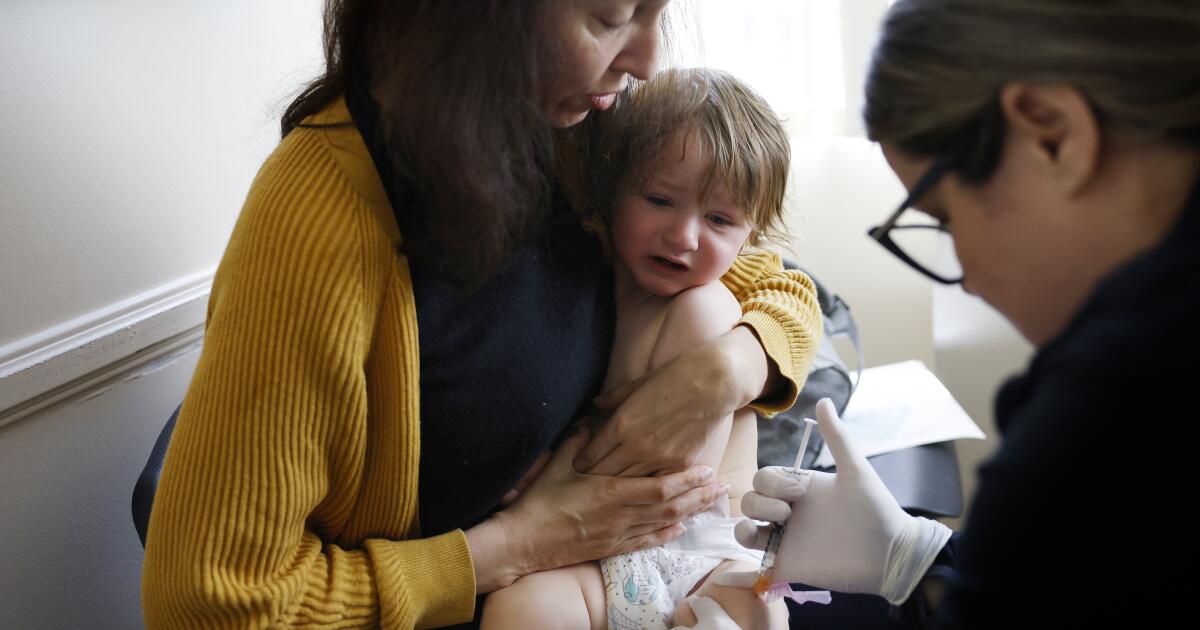
As measles cases pop up across the country this winter — including several in California — one group of children is stirring deep concerns among pediatricians: the babies and toddlers of vaccine-hesitant parents who are delaying their child’s measles-mumps-rubella shots.
Pediatricians across the state say they have seen a sharp increase recently in the number of parents with concerns about routine childhood vaccinations who are demanding their own inoculation schedules for their babies, creating a worrisome pool of very young children who may be at risk of contracting measles, a potentially deadly yet preventable disease.
“Especially early on, when a parent is already feeling really vulnerable and doesn’t want to give something to their beautiful baby who was just born if they don’t need it, it makes them think, ‘Maybe I’ll just delay it and wait and see.’” said Dr. Whitney Casares, a pediatrician and author who has written on vaccination for the American Academy of Pediatrics. “What they don’t realize is if they don’t vaccinate according to the recommended schedule, that can really set their child up for a whole lot of risks.”
It is difficult to know how widespread such delays have become. California keeps careful track of the rate of kindergartners who have been vaccinated against measles, but does not have comprehensive data for children at younger ages.
Dr. Eric Ball has seen the shift firsthand. At his Orange County pediatric practice, Ball said, he has noticed an increase in parents asking about delays since the COVID-19 pandemic, as politicization of and misinformation about that vaccine has seeped into discussions about routine childhood vaccinations, including measles-mumps-rubella, known as MMR.
Dr. Eric Ball examines 9-month-old Noah at Southern Orange County Pediatric Associates in Ladera Ranch on Feb. 28.
(Christina House / Los Angeles Times)
Rather than an outright refusal, however, these vaccine-hesitant parents express a softer kind of reluctance, asking if it’s possible to use an “alternative schedule” of vaccines, rather than sticking to the Centers for Disease Control and Prevention’s recommendations. Sometimes they seek to delay the shots by a few months, and sometimes by several years.
“I have patients who have three kids, and they vaccinated the first two kids on schedule. And then since COVID, with their third kid, they are like, ‘I don’t know if this is safe. I want to wait until the kids are older’, or ‘instead of doing two shots today, I want to do one shot,’” said Ball. “It just prolongs the time where you have a child who’s unprotected and potentially can get sick from these diseases.”
He tries his best to explain to parents the importance and safety of vaccines, including MMR. He even brings out his own children’s vaccine records to prove his point, and he is often successful. But not always.
At Children’s Hospital Los Angeles, attending pediatrician Dr. Colleen Kraft said about half of parents are questioning the CDC’s recommended vaccine schedule — a significant increase since the pandemic.
“Even my most reasonable parents ask questions. So it’s definitely in the mainstream,” she said. She also worries about her patients who are behind on vaccines because they missed so many appointments during the pandemic and are only now returning to her office.
Karla Benzl holds her son, 15-month-old Marcus, before he gets vaccinated at Southern Orange County Pediatric Associates in Ladera Ranch on Feb. 28.
(Christina House / Los Angeles Times)
In Marin County, parents’ requests to delay vaccinations have become so frequent that Dr. Nelson Branco said last month his practice decided to tighten vaccine requirements as cases of both measles and pertussis have spread. Babies seen by doctors in the practice will need to have their first set of vaccines completed by 4 months of age. The primary series of vaccines against the most serious and common diseases, including measles, must be completed by 24 months.
If parents don’t agree, they must leave the practice.
“Kids are doing a lot of things that are high risk before they’re 5 and are required to be vaccinated to attend kindergarten, said Branco. “They’re getting on international flights, they’re going to Disneyland where there are lots of kids,” leaving young children vulnerable to measles when they could be protected.
The CDC recommends that the first dose of MMR be given when a baby is 12 to 15 months old. Usually this happens at a child’s 12-month well visit. A second dose is then given at 4 to 6 years of age.
At least 95% of people in a community must be vaccinated to achieve a level of “herd immunity” that protects everyone in a community, including those who cannot get the vaccine because they are too young or are immunocompromised, according to the World Health Organization.
Low vaccination rates have led to measles outbreaks in several states over the last decade, most recently in Florida.
Nationally, the rate of kindergartners fully immunized against the measles dropped from 95% in the 2019-20 school year to 93% in 2022-23, according to the CDC.
But there is overall good news in California. Since the state’s 2015 ban on parents’ personal beliefs as a reason to skip vaccinating children before school, the measles vaccination rate for kindergartners has grown from 92% in the 2013-2014 school year to 96.5% in 2022-2023.
Are you a SoCal mom?
The L.A. Times early childhood team wants to connect with you! Find us in The Mamahood’s mom group on Facebook.
Share your perspective and ask us questions.
But those postponing vaccinations have created a potential vulnerability gap in a child’s first four years.
One in 5 unvaccinated people who get measles in the U.S. will be hospitalized. Since there is no good treatment for measles, doctors can often do little more than offer supportive care. One in 1,000 children with measles will develop brain swelling that can leave a child deaf or with an intellectual disability; 1 to 3 children in 1,000 will die, according to the CDC.
Measles is so contagious that 90% of people close to an infected person will catch it if they are not immune, according to the CDC. The virus can remain contagious in a room or on a surface for up to two hours after the infected person has left.
In the Children’s Hospital Orange County primary care network, which has more than 130 pediatricians, the share of 15-month-olds with an MMR vaccine has been dropping consistently over the past last few years, from 98% in 2019, down to 93.5% in 2023.
For years in the early 2000s, anti-vaccine sentiment was at an all-time high after the publication of a now-debunked and retracted study that falsely tied the MMR vaccine to autism. In December 2014, an unvaccinated 11-year-old was hospitalized with measles following a visit to Disneyland. Over the next few months, measles spread to 125 people across seven states.
The outbreak helped galvanize support for vaccination nationwide. A year after the Disneyland outbreak, California passed its ban on personal exemption.
“The pendulum swung back the other way, and we had a few years where vaccination rates were really high,” said Ball. But the rumors and rhetoric surrounding the COVID vaccines have caused the pendulum to swing in the other direction. “We’re back to dealing with conspiracy theories, things that people heard on the internet, or something that their cousin’s neighbor’s roommate said. It’s really hard.”
Noah, who is 9 months old, gets his measurements taken by medical assistant Shellee Rayl at Southern Orange County Pediatric Associates in Ladera Ranch on Feb. 28.
(Christina House / Los Angeles Times)
A Pew Research poll conducted in March 2023 found that 88% of Americans are confident that the benefits of an MMR vaccine outweigh the risks, a percentage that has remained fairly consistent since before the pandemic.
But support for all school-based vaccine mandates has fallen; 28% now say that parents should be able to decide not to vaccinate their children, even if it causes health risks for others, up from 16% in October 2019. Among Republicans, the share has more than doubled, from 20% in 2019 to 42% in 2023.
Support for the MMR vaccine was lower among parents with young children, the poll found. About 65% of parents with children under age 5 reported that the preventative health benefits of MMR were high — compared to 88% of all adults — and 39% said the risk of side effects was either medium or high; half said they worried about whether all childhood vaccines are necessary.
Tara Larson, a former ER nurse who lives in Santa Monica, said she became concerned about childhood vaccination when she was pregnant last year. She started watching anti-vaccine documentaries, reading vaccine safety inserts, and following several social media accounts “to make us an informed vaxxer. We’re not anti-vax,” she said.
Larson decided that she wanted to delay vaccinating her son until he was 3 months old, to limit him to just three vaccines in his first year that she felt were essential, and to spread them out so that he would only get one shot per month. “By the time he starts playing on the playground and goes to school, he’ll need to start his course of Hep B, but why overload his course of vaccines right now?” she said.
The first pediatrician she saw refused to follow her requested schedule. But, Larson said, “in my gut, I just felt like this is the right thing to be doing for our baby, and I left.” After weeks of searching, she found a holistic provider who charges a $250 monthly fee and agreed with her approach.
She said she hasn’t yet decided whether to give her son, who is now 8 months old, the MMR vaccine when he becomes eligible. “I think some doctors will say to wait until they’re 3, but that was when there wasn’t a resurgence of measles,” she said. “That’s my next thing to dive into.”
Karla Benzl of Mission Viejo comforts her 15-month-old son, Marcus, after he received his vaccinations.
(Christina House / Los Angeles Times)
But there’s no scientific basis and no known benefits to delaying vaccines except in very rare medical circumstances, said Casares, whose pediatric practice is in Oregon.
Casares said the problem is that parents have an “exposure bias.” They often consume an onslaught of information on social media about the risks, but very little about the benefits of vaccines or the enormous risks of the diseases themselves. She said in a country such as the United States, where vaccination rates are fairly high, most people don’t see the ravages that the diseases can cause if rates fall.
This article is part of The Times’ early childhood education initiative, focusing on the learning and development of California children from birth to age 5. For more information about the initiative and its philanthropic funders, go to latimes.com/earlyed.

Science
5 Great Stargazing Trains

Stargazing, it turns out, doesn’t have to be a stationary activity.
On railway lines around the world, from the Arctic Circle to New Zealand, a select set of evening train excursions take riders deep into dark-sky territory — some en route to remote station stops decked out with telescopes, others featuring onboard astronomers.
These five rail journeys (all of which are accessible) range from two- to three-hour desert outings to a hunt for the northern lights. One route even has a planetarium on rails. All promise a renewed appreciation of train travel — and of our pale blue dot’s improbable place in the cosmos.
Nevada
The Great Basin Star Train
Any stargazing train worth its salt requires one thing: a dark sky. The Star Train resoundingly checks that box, traveling through a part of eastern Nevada that is one of the least-populated places in the lower 48.
Run by the Nevada Northern Railway in partnership with nearby Great Basin National Park, the train departs the historic East Ely Depot, in Ely, Nev., early enough in the evening to catch the sunset over the Steptoe Valley, and then cruises through darkening skies to its destination: a remote corner of the desert appropriately called Star Flat, where a stargazing platform outfitted with telescopes awaits. There, riders disembark (equipped with red-light necklaces to help preserve their night vision) and take turns viewing the cosmos, guided by professional astronomers. (Last year’s onboard stargazing guides came from Caltech; in previous seasons, the National Park Service’s Dark Rangers, who specialize in night-sky activities, accompanied trips.)
The Star Train makes its two-and-a-half-hour round-trip journey most Friday evenings between mid-May and mid-September, and tickets ($65 for adults) can sell out almost a year in advance — though members of the Nevada Northern Railway Museum get early access. Alternatively, the railroad’s more frequent Sunset, Stars and Champagne excursions trade telescopes for desert sundowners but feature the same expert stargazers and the same Nevada night sky, which is often dark enough to see the Milky Way with the naked eye.
New Mexico
The Stargazer
While plenty of heritage railroads across the United States offer twilight rides and nighttime excursions, at the moment there’s only one other dedicated, regularly scheduled stargazing train in North America besides the Star Train: the Stargazer, operated by Sky Railway, in Santa Fe, N.M.
Much like its Nevada counterpart, the Stargazer makes a two-and-a-half-hour round trip through dark-sky country, though in this case, the journey really is the destination, because it doesn’t make any stops. More of a rolling night-sky revue, the Stargazer features live music and professional astronomers who share their celestial knowledge and stories as the train rumbles into the vast Galisteo Basin south of Santa Fe. Sky Railway’s colorfully painted trains feature heated, enclosed passenger cars to stave off the evening chill and flatbed cars open to the night sky.
Departing from the Santa Fe Depot downtown, the train normally runs once a month (adult tickets from $139, including a champagne welcome toast). Sky Railway also occasionally schedules excursions for special celestial events.
New Zealand
Matariki Rail Experience
With its alpine landscapes and rugged coastline, New Zealand’s South Island is practically tailor-made for scenic daytime train journeys. But when night falls, the sparsely populated island — home to the Southern Hemisphere’s largest International Dark Sky Reserve — is heaven for stargazers, too.
This year, Great Journeys New Zealand, which operates the country’s tourist-centric long-distance trains, is offering a special nighttime run of the Coastal Pacific, whose route skirts the South Island’s northeastern coast. Timed to Matariki, the Maori new year, which is heralded by the first rising of the Pleiades star cluster, the eight-hour round trip from Christchurch is a cultural and astronomical celebration.
After the first half of a four-course onboard dinner, the train arrives in Kaikoura, in dark-sky country, for a guided stargazing stop with a range of telescopes — and fire pits and a night market. (The rain plan involves a virtual stargazing session at the local museum using virtual reality headsets.) Dinner resumes back on the train as it returns to Christchurch. This is a strictly limited engagement, on the rails for one night only: July 11, for 499 New Zealand dollars, about $295, per person.
In the far northern reaches of Norway, inside the Arctic Circle, you can ride a train that chases another wonder of the night sky: the aurora borealis. Twice a week from October to March, the Northern Lights Train takes its riders into the dark polar night in pursuit of the aurora’s celestial light show.
From the remote town of Narvik, the train travels along the Ofoten Railway, the northernmost passenger rail line in Western Europe. The destination on this three-hour round-trip excursion (1,495 kroner, or about $160) is Katterat, a mountain village accessible only by rail and free of light pollution, making it an ideal place to spot the aurora. At the Katterat station, local guides and a campfire cookout await, as does a lavvu, the traditional tent used by the Sami people of northern Scandinavia, offering a respite from the cold (as well as hot drinks and an open fire for roasting sausages).
And aboard the train, the lights stay off, which means that on a clear night, you might even catch the northern lights on the way there and back.
Leave it to Japan to take the stargazing train to another level.
The High Rail 1375 train — so named because it runs along Japan’s highest-elevation railway line (the high point is 1,375 meters, or roughly 4,500 feet, above sea level) — is one of JR East’s deliberately unhurried Joyful Trains, which the railway company describes as “not only a means of transportation, but also a package of various pleasures.” This astronomy-themed train certainly packs plenty of joy into its two cars, with seat upholstery inspired by constellations, a snack bar, a souvenir shop and a planetarium car with a library of astronomy books and images of the night sky projected onto its domed ceiling.
The train makes two daytime runs along the mountainous Koumi Line, taking a little over two hours to travel between Kobuchizawa (accessible by express train from Tokyo) and Komoro. But the main event is the High Rail Hoshizora (“Starry Sky”) evening trip, which includes an extended stop at Nobeyama Station (the highest in the country) for a guided stargazing session. A one-way ride on High Rail 1375, which runs on weekends and occasional weekdays, requires a seat reservation if you’re traveling on a Japan Rail pass, or a stand-alone ticket plus seat reservation (2,440 yen, or about $15). And remember to preorder a special “Starry Sky” bento box.
Follow New York Times Travel on Instagram and sign up for our Travel Dispatch newsletter to get expert tips on traveling smarter and inspiration for your next vacation. Dreaming up a future getaway or just armchair traveling? Check out our 52 Places to Go in 2026.
Science
A Physicist Who Thinks in Poetry from the Cosmic Edge

Much of the praise for Chanda Prescod-Weinstein’s debut book in 2021, “The Disordered Cosmos: A Journey Into Dark Matter, Spacetime, and Dreams Deferred,” lauded the way she used personal experiences in physics to discuss the social and political inequities that exist alongside scientific breakthroughs.
“It contains the narrative of dreams deferred,” Dr. Prescod-Weinstein, a physicist at the University of New Hampshire, explained in April at a bookstore in Chicago. But its very existence, she said, also “represented a dream deferred, because that was not the dream of what my first book was going to be.”
Her second book reclaims that dream. Released on April 7, “The Edge of Space-Time: Particles, Poetry, and the Cosmic Dream Boogie” is less pain and more play, a homage to the big questions that made Dr. Prescod-Weinstein want to become a physicist in the first place. She begins the book by asserting that it is humanity’s duty to uncover and share the story of our universe. Her latest offering toward that duty is a journey through physics that is tightly bound to her own cultural roots.
In the midst of a multicity book tour, Dr. Prescod-Weinstein spoke with The New York Times about guiding readers through the cosmos from her own point of view and about some of the art, poetry and literature she drew on to shape that journey. This conversation has been edited for brevity and clarity.
Why include so many references to poetry in a book about physics?
I knew poetry before I knew physics. It was part of my upbringing. I loved A.A. Milne’s “Now We Are Six” and Edward Lear’s “Nonsense Limericks.” Both of my books draw their subtitles from Langston Hughes’s “Montage of a Dream Deferred.”
Adrienne Rich’s poem “The Burning of Paper Instead of Children” became a guiding light for how my work would move in the world. It also opened up for me that I need language. That’s true among physicists. Even an equation is a sentence; even an equation is telling a story.
As physicists, we’re always working in language to connect what we learn with what we know. Poetry is one of the first places that my brain goes to draw those links. Language, as it moves in my brain, is often in Hughes and Rich and Shakespeare. Those are the lines that flicker up for me.
What if we got away from the argument that doing cosmology and particle physics is practical or materially valuable? Then we have to accept that we’re like the poets. What we do is important culturally in the same way poetry is. A piece of this book is me saying there is value in banding with the poets, and fighting for the value of being curious and trying to articulate the world with whatever tools are available to us. Not for the purposes of selling something, but for the purpose of fulfilling our humanity.
Another theme throughout the book is the story of Lewis Carroll’s Alice and her adventures in Wonderland.
Being a science adviser on future installments in The Legendborn Cycle, a fantasy series written by Tracy Deonn, is one reason Alice is in my book. It has allowed me to be open to the playful side that physics, as a Black queer person, can take from you. I wanted the book to be whimsical, because that’s who I was when I first arrived in physics, and that’s who I want to be when I die.
Part of the call of quantum physics is to change what our sense and sensibility are. When you look at the world through this framework — like the idea that particles have spin but don’t really spin — it sounds like nonsense. Except that’s literally how the universe works. Physics is our “through the looking glass.” It’s real.
Your first chapter invites readers to reflect on the metaphors used to describe the universe, like the “fabric” of space-time or electromagnetic “fields.” Why open in this way?
A lot of books about quantum physics start with its history. I wanted as much as possible not to just do that. I had actually planned to start it with the Stern-Gerlach experiment of 1922. But then I read an essay by the poet Natasha Trethewey about abiding metaphors and started to ask myself what the abiding metaphors of my physics training were.
We don’t ever take time in our classes to ask, “What do we mean when we say ‘space’? What do we mean when we say ‘space-time’?” There are these metaphysical questions that I often told myself were for the philosophers. This book was me letting myself think of them as physics.
One metaphor you invoke is the “edge” — not only the edge of the universe and of scientists’ understanding, but also existing at the edge of certain identities.
In “Disordered Cosmos,” I talked a lot about being at the margin and looking toward the center. With “The Edge of Space-Time,” I’m choosing to make the margin the center of the story. Part of that was me fully embracing what makes me the physicist I am. I’m an L.A. Dodgers fan. I love “Alice in Wonderland.” I love “Star Trek.” There’s lots of all of that in the book.
Picking a metaphor is a culturally situated decision. I wrote a line that says black holes are the best laid edges in the universe. I did, at some point, think that only some people were going to get this. But for people who don’t understand the reference to Black hairstyles, the sentence is still legible. And for those who do, it will feel like we just had an in-group moment. Anyone who thinks about laying their edges deserves to have an in-group moment in a physics book. Because we are physics, too.
Black students are often told that if you want to be a physicist, then you will make yourself as close to such-and-such mold as possible. At a young age, we have this understanding that whiteness and science are associated with each other, but we are also witnessing in ourselves that this can’t be entirely correct. There’s this narration of, “Well, sure, you can be Black in physics, but that means you have to acclimate to the ‘in physics’ part, and never that physics has to acclimate to the Black part.”
I use the example of rapper Big K.R.I.T.’s song “My Sub Pt. 3 (Big Bang),” in which someone tries to wire up subwoofers in his car but fries the wires because he doesn’t ground them properly. I don’t know if Big K.R.I.T. would think of this as a science story, but I think we should learn to read it as one. Not to contain it in science, but to say it overlaps there. This can be a rap song. It can be about the cultural significance of subwoofers and the Big Bang as a metaphor for the beat. And it can also be about cosmology and about how everybody who wires up cars or does this kind of work is a scientist, too.
How do you want readers to approach this book?
There is this feeling that you’re supposed to read a book like this and walk away an expert. That’s actually not the point of this book at all. The point is to wander through physics. Even if math terrifies you, you are entitled to spend some time with it.
And so here, I have made you a book with a bunch of tidbits on the oddities of the universe. The universe is stranger and more queer and more wonderful and more full of possibility than whatever limitations you might be experiencing right now. Physics challenges what we are told are social norms. For example, non-trinary neutrinos are fundamental to our standard model of physics.
“Non-trinary,” as in they shift between three different forms.
Non-trinary is natural. It’s such a challenge to the current anti-trans rhetoric that says people can only ever be one thing.
I don’t need my book to be the most important thing that someone reads. But I want it to be a source of hope. If it reminds you that, as my mom says, the universe is bigger than the bad things that are happening to us, then that’s all you need to remember. I’m good with that.
Science
Footage shows Central Valley dairy workers kicking young calves, pulling them with pliers

In late February, animal rights activists flew a drone over a calf ranch in the Central Valley and watched as workers kicked and punched the animals.
For the record:
7:15 p.m. May 12, 2026This article has been updated to reflect that no calves from Agresti Calf Ranch have ever gone on to be used for Clover Sonoma milk supplies, and the calf ranch opened only in 2025. In additional comments, Clover Sonoma also said in the future, no animals from Agresti Calf Ranch will be part of its supply.
Footage reviewed by The Times shows a worker pulling a calf by the nose with pliers.
It shows two workers removing the budding horns of a calf with a hot iron. While one held the frightened animal’s head, the other — wearing a sweatshirt with an image of the Virgin Mary — applied the iron to a horn. After a puff of smoke, the calf fell to its side, appearing motionless.
-
Share via
Both male and female calves produce horns. To prevent injury to the animals and their handlers, these are commonly removed. Humane guidelines require anesthesia.
The footage was collected by the group Direct Action Everywhere, known for tactics including releasing beagles from medical breeding facilities and abused calves from farms. It was shot at the Agresti Calf Ranch in Ceres, near Modesto, which is certified by the American Humane Society for its ethical treatment of animals. The workers could not be reached for comment. One was subsequently terminated, the Humane Society said.
The Agresti Calf Ranch opened in 2025 and is operated by the owners of Double D Dairy, just up the road. Double D Dairy owns more than 10,000 cows across several operations.
The owner of Double D, Dominic Assali, declined to answer questions in person. A phone number for the dairy online is disconnected. In response to an email to his personal account, Assali said, “Animal welfare and safety are incredibly important to us, and we have a zero-tolerance policy for any mistreatment.
“We’ll always take immediate, thorough action to address any operational issues, as we have in this instance,” the email said.
The American Humane Society is a 150-year-old nonprofit focused on animal welfare. Among other things, it certifies animal safety on farms as well as on movie sets. In a statement, it said only 10% of animals raised on farms in the U.S. are certified as humanely treated.
Assali is the grandson of the farm’s founders, Harold and Marlene Agresti. He is a board member of Western United Dairies, the largest dairy trade group in California.
The mistreatment captured on video has also created a headache for a prominent California sustainable milk brand, Clover Sonoma, based in Sonoma County.
It gets 10% to 15% of its milk from Double D, and Assali and his family are featured on Clover Sonoma’s website. No calves from Agresti Calf Ranch have ever gone on to be used in Clover Sonoma milk supplies, the company said in a statement. It’s unclear whether the abused calves were being raised for beef or dairy.
A Clover Sonoma sign hung outside the main dairy complex on a recent visit.
Clover Sonoma markets its milk, yogurt and cheese products as humanely sourced and environmentally sound. It was the first dairy company to receive a cruelty-free certification from the American Humane Society in 2000. The website also features a “Our Promise” page, which states the company demands “the humane treatment of animals.”
“We were deeply concerned by the reported mistreatment of some cows captured on video at Agresti Calf Ranch during a separate cow operation,” the company said in an email.
“The rough handling shown at Agresti Calf Ranch is contrary and inconsistent with the humane practices we have fostered for decades and which we demand of all our suppliers.”
Clover Sonoma said it suspended business with Double D as soon as it became aware of the incidents and began “a rigorous audit,” which just ended.
“Clover and the American Humane Society have concluded that the mistreatment was an isolated issue, not systemic or reflective of Agresti Calf Ranch’s personnel. Corrections have been made, including the termination of the employee in the video. As such, we are comfortable reinstating the milk from Double D Dairy.”
After this story published, Clover went further and said a condition of Double D’s reinstatement will be that no animals from Agresti Calf Ranch will be part of Clover’s dairy supply.
A statement from the Humane Society said Clover Sonoma is working with Double D to strengthen its whistleblower policy and training, and has “reiterated its commitment to ongoing independent, third-party audits,” with both announced and unannounced visits.
Clover Sonoma mainly buys and processes milk from dairies in verdant Sonoma County, as the company’s marketing suggests. Double D Dairy is one of its few suppliers in the Central Valley, which is associated more with industrial-scale agriculture.
On a recent weekday, the calf ranch and dairy farm were visible from a public road. Holstein calves, a popular dairy breed, could be seen in cages through small trees in front of the enclosures. The sound of mooing and a pressure washer could be heard. The smell of manure and dirt wafted in the humid air.
Most dairy companies remove calves from their mothers after birth, raising them separately so they don’t take the mother’s commercially valuable milk. Some dairy farms send calves out to third-party calf ranches for rearing. Others raise them on-site. Female calves are typically raised to become milk cows. Male calves are sent away to become beef or other meat-based products, such as pet food.
A 2025 State Water Board document shows the farm houses an average of 700 calves at any one time, with a maximum 1,400.
The Direct Action Everywhere activists were recently on a public road near Double D’s main farm, flying a drone over the property. Within 30 minutes of their arrival, seven Stanislaus County sheriff’s vehicles arrived and surrounded the activists.
A heavily armed officer asked to see the drone pilot’s Federal Aviation Administration license, which he provided. After confirming it was valid, a sheriff’s deputy — one of nine at the scene — told the activists they could remain on the road but could not trespass.
Asked about the heavy response, a deputy said there had been several recent violent incidents from animal rights groups at the site, and mentioned the groups had sent in “busloads” of activists.
The Times reached out to the Sheriff’s Office to get more details about those events but did not get a response.
Temple Grandin, author and professor of livestock medicine at Colorado State University, said that punching and kicking livestock is considered abusive.
An expert in livestock welfare, she said that handlers can tap, push and nudge animals. But if the level of force goes beyond what could bend the side of a cardboard box, “it’s abuse. Period.”
She said the calves’ reaction to the hot iron indicates that pain medication, such as lidocaine, was not applied before the procedure. Double D did not respond to a question about whether medication was given before the procedure.

A pickup truck rolls by the barns at Agresti Calf Ranch at sunrise in Ceres.
(Tomas Ovalle/For The Times)
-

 Michigan1 minute ago
Michigan1 minute agoPuppies, prom and pancakes: What to do in West Michigan this weekend
-

 Massachusetts7 minutes ago
Massachusetts7 minutes agoBattenfeld: Have Massachusetts voters finally had enough of soft on crime?
-
Minnesota13 minutes ago
Caribou Coffee in Minnesota launches value menu
-
Mississippi19 minutes ago
Mississippi State, Ole Miss baseball hosting scenarios for NCAA Tournament bracket
-
Missouri25 minutes ago
Missouri Lottery Powerball, Pick 3 winning numbers for May 13, 2026
-
Montana31 minutes ago
Montana Lottery Powerball, Lotto America results for May 13, 2026
-

 Nebraska37 minutes ago
Nebraska37 minutes agoNebraska QB has high expectations heading into 2026 season
-

 Nevada43 minutes ago
Nevada43 minutes agoArbor View beats rival Centennial for 5A boys volleyball state title