Science
Column: He got his ‘End of Life’ medication within 48 hours. Will the option be there for others?

Matt Fairchild loved movies, he loved serving in the Navy and the Army, and he adored his wife, Ginger.
But for nearly 10 years, cancer assaulted him, beginning as a melanoma lesion near his ear before marching through his bones, brain and spine. Matt fought not just the cancer, but the effects of chemotherapy and other treatment. A rod had been inserted into his back after his spine was ravaged, and when the rod snapped, Matt told Ginger he wasn’t going back to the hospital.
Matt Fairchild served in the Navy and the Army.
(Fairfield Family photos)
Friends began dropping by the Fairchilds’ Burbank home in January 2022, with Matt, 52, greeting them from his hospice bed in the dining room.
“We had nurses coming in and out, and he couldn’t get up to go to the bathroom,” said Ginger, a registered veterinary nurse, who had been with Matt for more than 30 years. “He couldn’t push himself up…and he was so swollen from the steroids.”
California’s End of Life Option Act had just been tweaked to allow terminally ill patients to get life-ending medication in 48 hours rather than having to wait 15 days.
California is about to be hit by an aging population wave, and Steve Lopez is riding it. His column focuses on the blessings and burdens of advancing age — and how some folks are challenging the stigma associated with older adults.
Matt, a supporter of Compassion & Choices, an advocacy group whose mission is to improve end-of-life care options, would be among the first Californians to act on the new provision. Not everyone who gets the life-ending prescription uses it. Of the 5,168 prescriptions written since the option took effect in 2016, about two-thirds have died from ingesting the medication.
Matt, who was Catholic, fought as long as he could, Ginger said. But when he knew he was ready, he wanted to get the medicine “as fast as possible.” Knowing it was on its way put him in a state of calm, Ginger said.
“It was really comforting, but it was also really sad and really hard,” she told me in the very room where this had played out. “He said that he didn’t want to leave me and that he loved me, and I told him that I’d be OK.”
They held hands. Matt drank the medication.

Matt Fairchild and his wife Ginger, who says: “Matt thought it was preposterous to think that anyone would be coerced.”
(Fairfield Family photos)
“And then he kind of laid back and went to sleep.”
Ginger is sharing this story now because California’s End of Life Option Act has been challenged in federal court. A lawsuit filed in April, with a hearing scheduled for next month, alleges that people with disabilities stand the risk of being coerced into choosing to end their lives because they don’t have access to quality care.
“Matt thought it was preposterous to think that anyone would be coerced,” said Ginger, who argues that ample safeguards are in place to make sure there’s no abuse.
The lawsuit, filed on behalf of several disability rights groups, makes the claim that California is “running a deadly system that steers people with terminal disabilities away from necessary mental health care, medical care, and disability supports, and towards death by suicide under the guise of ‘mercy’ and ‘dignity’ in dying.”
San Francisco civil rights attorney Michael Bien, who represents the disabilities groups, told me he doesn’t think the state should be in the business of helping people take their own lives. It should instead ensure that people with disabilities and people of all races and incomes get equal access to healthcare that allows them to extend their lives rather than cut them short.
I can’t argue with him about healthcare inequities. I did ask, however, if Bien thinks there are situations, such as that of Matt Fairchild, in which he supports a patient’s right of self-determination.

Ginger Fairchild holds a photo of her with her husband, Matt. When he knew he was ready, she says, Matt wanted to get the medicine “as fast as possible.”
(Steve Lopez/Los Angeles Times)
“I don’t think someone should be forced to live, and I think people have a right to die through natural means,” said Bien. “But I think it’s very dangerous to have doctors violating their Hippocratic oath and killing people…I want the doctor to play doctor, and not executioner.”
The lawsuit names two plaintiffs with severe disabilities.
One is a Black Navy veteran of limited means who is a formerly suicidal quadriplegic and “currently is unable to obtain the level of in-home care” he needs, according to the lawsuit. The Oakland resident “experiences anxiety and depression” and “fears that he will again become suicidal.”
The other is a white Berkeley woman with muscular dystrophy who uses a ventilator and “is fearful that her medical providers will steer her towards physician-assisted suicide in lieu of providing life-sustaining treatment during a time when she has impaired judgment due to anxiety and/or depression.”
State lawyers, in a motion to dismiss the lawsuit, argued that those two plaintiffs have not applied for aid in dying and might not be eligible. A person has to be deemed terminally ill, with less than six months or less to live, and must submit two requests for medication.
(Fairfield Family photos)
The requests must be witnessed by two adults — one of whom does not stand to benefit financially — who can attest that the patient is of sound mind. The physician who prescribes the medication must determine, among other things, whether the request for medication is being made voluntarily.
“There is no evidence…that the law steers anyone anywhere, or poses any harm to people with disabilities,” said a statement from Kathryn Tucker, an attorney representing several groups opposing the lawsuit, including the Golden West Chapter of the ALS Assn.
When I first wrote about right-to-die legislation, before California followed Oregon’s lead in 2016, I was a vocal advocate. My father, in his final years, surrendered much of what he had lived for, and it was that loss, rather than physical pain, that wore him down. He was, however, subjected to too many unpleasant and perhaps unnecessary medical procedures, and I remember him saying enough already when a doctor recommended a feeding tube.
My mother had a similar experience, and I still wonder — in a culture that has trouble accepting the natural course — whether we know the difference between extending our lives and prolonging our deaths.
After I spoke to Ginger Fairchild about Matt, I visited via Zoom with Bay Area poet Charles Entrekin, who is terminally ill, and his wife, Gail, also a poet. Charles is blind and has Parkinson’s; Gail cares for him. They both support the End of Life Option Act.
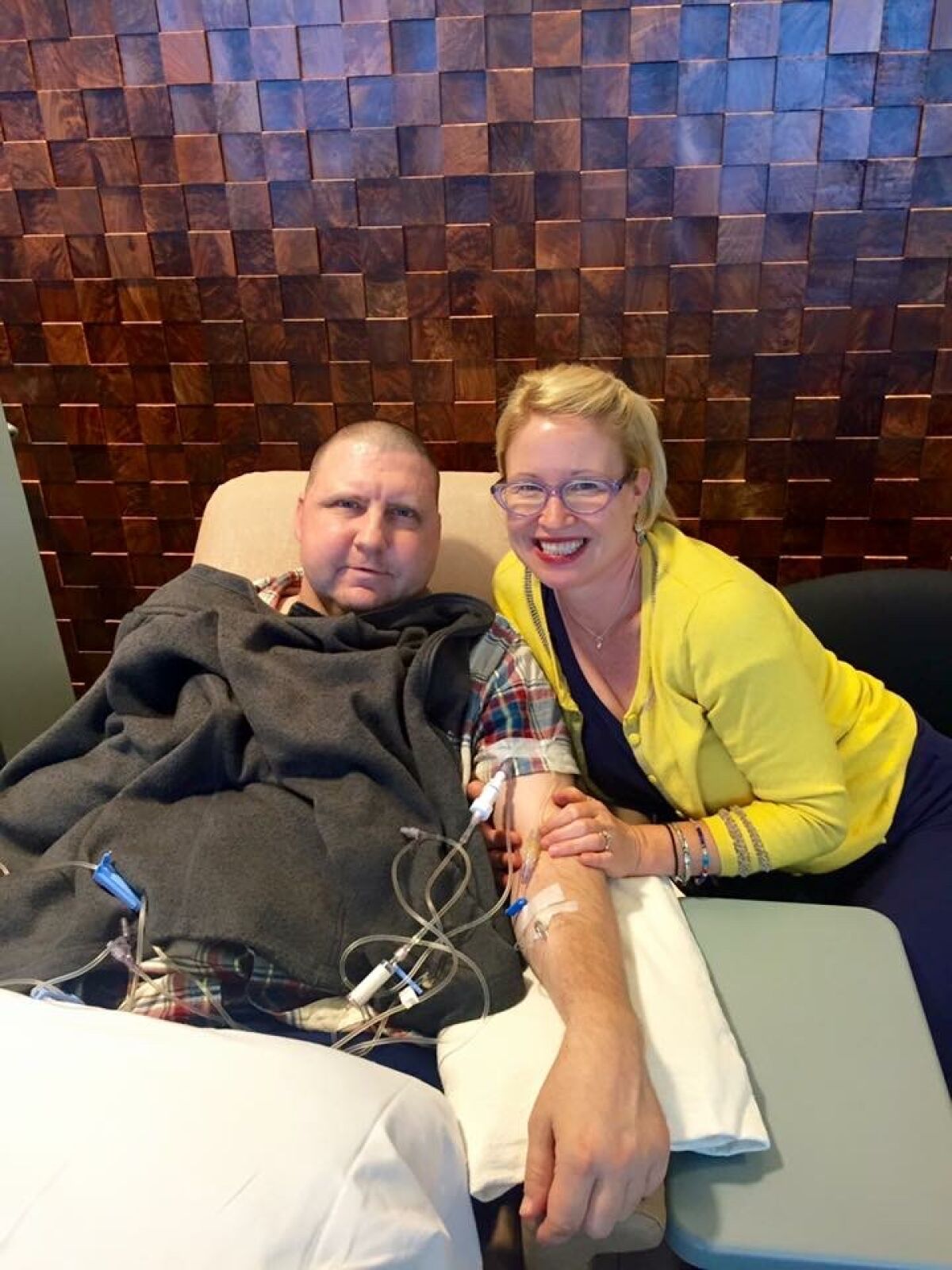
(Fairfield Family photos)
“I’d like not to be trapped into living my ending days drugged out and in hospice,” said Charles, who wants to hold onto the option of ending his own life, and I feel the same way.
The Entrekins sent me some of their poetry, and before I write more about their situation, I’d like to read the poems and pay them a visit.
“He’s walking a fine line,” Gail said of her husband. “Is there still some quality of life worth staying for? Or is it time?”
Steve.lopez@latimes.com

Science
The Tijuana River smells so bad, the CDC is coming to investigate

San Diego County residents will have an opportunity to share their pollution concerns about the Tijuana River when officials from the Centers for Disease Control and Prevention arrive later this month to conduct a health survey.
This is the first time that a federal agency is investigating the potential harm caused by millions of gallons of raw sewage pouring through the Tijuana River that have caused beach closures of more than 1,000 days. Residents living near the river say they have been suffering unexplained illnesses, including gastrointestinal issues and chronic breathing problems, because of the stench of hydrogen sulfide.
“We’re continuing to lean in and listen in on what our community residents are feeling,” said Dr. Seema Shah, the interim deputy public health officer with San Diego County. Supervisor Nora Vargas first wrote to the CDC back in May, formally asking the U.S. Department of Health and Human Services to look into the health complaints.
This week, the county began reaching out to thousands of residents to inform them that the CDC is coming in the hope that they will be more receptive to answering questions. “This is our chance to be able to communicate [pollution concerns] on a national level,” Shah added.
As part of what the CDC calls a Community Assessment for Public Health Emergency Response, 210 households will be surveyed about their mental and physical health, as well as the pollution’s effects on property values. The families will be randomly selected from 30 clusters of neighborhoods where San Diego County has identified air pollution complaints in the Tijuana River Valley.
Around 30 officials from the CDC and 50 graduate student volunteers from San Diego State University’s School of Public Health will be going door to door to conduct interviews with local residents over a three-day period. Here are the times when the survey will be conducted:
- Thursday, Oct. 17, 2024, from 2 p.m. to 7 p.m.
- Friday, Oct. 18, 2024, from 2 p.m. to 7 p.m.
- Saturday, Oct. 19, 2024, from 10 a.m. to 7 p.m.
The goal is to accommodate people’s schedules and, officials hope, catch them after work, Shah said. The volunteers are helping to bridge the language barriers with Spanish-speaking families.
“A lot of students, many of whom are bilingual, are from the community themselves,” said Paula Granados, an associate professor at San Diego State University’s School of Public Health, who’s been testing the Tijuana River for contaminants over the past month. “Our students are super excited. They want to help.”
The CDC could take weeks to months to release even the preliminary results from the survey, but for longtime residents like Bethany Case, this renewed attention already feels like a breath of hope.
“I just really want [this survey] to inform policy so that we don’t have to worry about our kids being sick,” said Case, the mother of two who’s lived in Imperial Beach for 16 years. For seven years she’s been an activist fighting to clean up the river as a volunteer with Surfrider, a nonprofit that works to preserve ocean access and cleanliness.
“I’m hoping that their survey shows that oftentimes it doesn’t just smell like sewage,” Case added. She doesn’t want the focus on the sewage to distract from the industrial waste that is dumped into the river that could be making people ill. “Oftentimes it smells like a chemical, it smells like a bite in the air, it burns your sinuses.”
Granados said the CDC’s survey is only a snapshot of what was going on when the data were collected, and conditions could worsen for residents when rainy seasons flood the river once more. Granados wants residents to know that even if they aren’t picked to respond to this survey, SDSU will be conducting its own yearlong survey that they can answer multiple times at tjriver.sdsu.edu.
“There’s research that’s still ongoing,” Granados said, and all that data will help policy decisions in the future. “We’re just committed to the long haul, whatever it takes to support the community.”
The county and other federal and state representatives have been working to raise awareness around the pollution to a national level.
Next week, the San Diego County Board of Supervisors will consider a proposal by Supervisor Terra Lawson-Remer to petition the Environmental Protection Agency to label the Tijuana River a Superfund site in need of remediation.
Science
'More serious than we had hoped': Bird flu deaths mount among California dairy cows

As California struggles to contain an increasing number of H5N1 bird flu outbreaks at Central Valley dairy farms, veterinary experts and industry observers are voicing concern that the number of cattle deaths is far higher than anticipated.
Although dairy operators had been told to expect a mortality rate of less than 2%, preliminary reports suggest that between 10% and 15% of infected cattle are dying, according to veterinarians and dairy farmers.
“I was shocked the first time I encountered it in one of my herds,” said Maxwell Beal, a Central Valley-based veterinarian who has been treating infected herds in California since late August. “It was just like, wow. Production-wise, this is a lot more serious than than we had hoped. And health-wise, it’s a lot more serious than we had been led to believe.”
A total of 56 California dairy farms have reported bird flu outbreaks. At the same time, state health officials have reported two suspected cases of H5N1 infections among dairy workers in Tulare County, the largest dairy-producing county in the nation. With more than 600,000 dairy cows, the county accounts for roughly 30% of the state’s milk production.
Beal’s observations were confirmed by others during a Sept. 26 webinar for dairy farmers that was hosted by the California Dairy Quality Assurance Program — an arm of the industry-funded California Dairy Research Foundation. A summary of the findings and observations was reported in a newsletter published earlier this week by the program.
Beal, along with Murray Minnema, another Central Valley veterinarian, and Jason Lombard, a Colorado State University veterinarian, described their observations and data to dairy farmers to help them anticipate the signs of, and treatments for, the virus.
The webcast was not made available to The Times.
“The animals really don’t do well,” Beal told The Times.
He said the infected cows he has seen are not dissimilar to people who are suffering from a typical flu: “They don’t look so hot.”
He and others think the recent heat may be a factor.
Since the end of August, the Central Valley has suffered multiple heat waves, with daytime temperatures exceeding 100 degrees.
“Heat stress is always a problem in dairy cattle here in California,” he said. “So you take that, you add in this virus, which does have some affinity for the respiratory tract … we always see a little bit of snotty noses and heavy breathing in animals that are affected … and for some of them, just the stress takes them.”
Indeed, most of the deaths are not directly the result of the virus, he said, but are “virus adjacent.” For instance, he has seen a lot of bacterial pneumonia, which is likely the result of the cow’s depressed immune system, as well as bloat.
He said that when the cows aren’t feeling well, they often don’t eat.
“The digestive tract, or rumen, basically requires movement. There has to be things moving out of that rumen constantly in order for the pH balance and microbiome to stay where it should be,” he said. So, when they’re not eating, things in the digestive tract stagnate.
That, in turn, causes them to “asphyxiate because their diaphragm has too much pressure on it.”
In addition, he and others are seeing a lot of variation in the duration of illness.
While early reports had suggested the virus seemed mild and lasted only about a week or two, others are seeing it last several weeks. According to the industry newsletter, at one dairy, cows were shedding virus 14 days before they showed clinical signs of illness. It then took another three weeks for the cows to get rid of the virus.
They’re also noticing the virus is affecting larger percentages of herds — in some cases 50%-60% of the animals. This is much more than the 10% that had been previously reported.
Some say the actual rate may be even higher.
“I would speculate infection is even higher; 50-60% are showing clinical signs due to heat stress or better herd monitoring earlier in infection. Unfortunately, few or no herds have been assessed retrospectively through serology testing to determine actual infection rates,” said John Korslund, a retired U.S. Department of Agriculture veterinarian epidemiologist.
Cows are also not returning to 100% production after they’ve cleared the virus, said Beal. Instead, he and others say it’s closer to 60%-70%.
“There’s going to be some animals that are removed from the herd, because they never seem to come back,” he said.
Beal said his firsthand observations have really challenged his notions about the disease, which has so often been described as mild and insignificant.
“Once I saw it myself, I said, this is something I need to communicate with my clients about … this is not something that is just a joke at the dinner table,” he said. “I didn’t want people to not take it seriously, because I see what it is doing to the animals, and it is rough to see — as an animal caretaker, as a veterinarian like myself — it’s just not something that’s enjoyable. It’s more serious than we had been led to believe.”
He said he is working hard with Central Valley farmers to treat the animals — largely by making sure the cattle are adequately hydrated. He also treats sick cows with a medication similar to aspirin, to reduce fever, pain and discomfort.
He said the treatment is pretty effective, and seems to be helping.
Others are not surprised H5N1 is becoming more severe in cows.
“As I’ve said since we first learned of the outbreak in dairy cows, nothing we’ve learned about this virus is new or unexpected,” said Rick Bright, a virologist and former head of the U.S. Biomedical Advanced Research and Development Authority. “It’s behaving exactly as we’ve come to know of this virus over the past 25 years. It’s spreading very efficiently now among mammals, and it’s mutating and adapting to mammals as it does.”
He credited state health officials and veterinarian for “being more forthcoming and transparent with their data” than other states, and said this may be the reason the virus seems to be hitting California cows so hard.
“This virus is out of control. It is time for urgent and serious leadership and action to halt further transmission and mutation,” Bright said. “The concept of letting it burn out through food animals, with unmonitored voluntary testing, has failed. There are pandemic playbooks that we need to dust off and begin to implement.”
In the meantime, officials continue to reassure the public about the safety of the nation’s dairy supply. They say pasteurization inactivates the virus. They also warn people to stay away from raw milk.
Beal noted one of the sentinel signs that a farm has been infected is dead barn cats that have drunk the infected, raw milk.
“It’s weird, actually, how consistently that seems to be happening everywhere,” he said. “It’s pretty sad and shocking. But that’s one of the first things that people see sometimes.”
There is also some suggestion that some cows that have recovered from the virus have been reinfected, although this has not been confirmed.
“We don’t have any data to support this yet, but there have been anecdotal reports of reinfections in herds,” said Kay Russo, a dairy-poultry vet with RSM Consulting, an international consulting firm.
She said it could just be a persistent infection that is being observed, but also speculated that the virus could be mutating rapidly — and evolving “enough to reinfect an animal.”
And Jason Lombard, one of the speakers at the dairy webinar, said in an email that he had been told by veterinarians that they are observing clinical signs of disease in animals that had been infected, “but I don’t believe any of them have been confirmed via testing.”
As of Oct. 4, California officials have reported 56 infected herds. Although state officials will not disclose the location of these herds, the Valley Veterinarians Inc. website — a veterinary clinic run by large-animal vets in the Central Valley — said the infections are in Tulare and Fresno counties.
Steve Lyle, a California Department of Food and Agriculture spokesman, would not confirm the counties.
There are more than 200 herds in Tulare County and more than 100 in Fresno County. The state’s largest raw milk dairy is also in Fresno County.
Requests by The Times to observe infected farms or speak with the owners of infected dairies went unanswered by the state and declined by industry insiders.
“We are not recommending farmers engage on this due to farm security issues we’ve had,” said Anja Raudabaugh, chief executive officer of Western United Dairies, an industry trade group for California dairy farmers. “It is very unwise to consider viewing a dairy under quarantine … this is just not the time.”
She said her organization doesn’t want anyone “doxing” farmers or increasing traffic at or near a farm, “both of which have happened.”
In the last week, the H5N1 virus has been detected in wastewater samples collected in Turlock, San Francisco, Sunnyvale and Palo Alto.
State epidemiologist Erica Pan said it was hard to know where the virus is coming from. While Turlock is a dairy center, the hits in the Bay Area cities could potentially be from wild birds, she said, but the source is not known.
Science
Opinion: The evidence shows women make better doctors. So why do men still dominate medicine?

“When will I see the doctor?” Most female doctors have been asked this question many times. It feels like a slight — a failure to recognize the struggle it took to get to where they are, a fight that is far from over once a woman has her medical degree.
Women now make up more than half of medical students but only about 37% of practicing doctors. That is partly because the makeup of the medical workforce lags that of the student body. But it’s also because persistent sexism drives higher attrition among women in medicine.
Even in households headed by a mother and father who both work, the woman is frequently expected to be the primary caretaker. As a result, female physicians often feel forced to work part time, choose lower-paying specialties such as pediatrics or leave the profession altogether.
That’s unfortunate not just for doctors but also for patients. On the whole, female doctors are more empathetic, detail-oriented and likely to follow through than their male counterparts. In other words, they are better doctors.
Admittedly, that is a generalization, but it’s one worth making. I experienced it firsthand working with female colleagues, and I’m informed by that experience in addressing my own medical needs. I prefer to see female doctors.
It wasn’t always that way. But after seeing a series of male doctors who were not listening to me, in a hurry to get out of the exam room or appearing only mildly interested in figuring out the cause of my problem, I made the switch — and I’m not going back. While I found that male doctors typically decided what my diagnosis was and how to treat it before entering the exam room, female doctors tended to be open-minded about what my medical issues were and — gasp! — listen to my answers to their questions.
But don’t take my word for it. Look at the data.
One recent study found that both female and male patients had lower mortality rates when they were treated by female physicians. Perhaps not surprisingly, the benefits of getting care from women were greater for women than for men.
“What our findings indicate is that female and male physicians practice medicine differently, and these differences have a meaningful impact on patients’ health outcomes,” said Yusuke Tsugawa, a senior author of the study.
Female doctors seem more likely to discover the root cause of a medical problem, as we are taught to do in medical school, rather than merely treat the symptoms.
“Female physicians spend more time with patients and spend more time engaging in shared medical decision-making,” Dr. Lisa Rotenstein, a co-author of the study, told Medical News Today. “Evidence from the outpatient setting demonstrates that female physicians spend more time on the electronic health record than male counterparts and deliver higher-quality care. In the surgical realm, female physicians spend longer on a surgical procedure and have lower rates of postoperative readmissions. We need to be asking ourselves how to provide the training and incentives so that all doctors can emulate the care provided by female physicians.”
One reason for the discrepancy might be male doctors’ propensity to be more ego-driven. They may revert to “mansplaining” to patients instead of engaging in an equal, cooperative patient-physician relationship. I’ve been guilty of that myself, so I know it when I see it.
What’s blocking women’s advancement in medicine? Old-fashioned sexism in the workplace is the most obvious answer. Female doctors are paid 25% less than their male counterparts on average, according to the 2019 Medscape Physician Compensation Report, earning an estimated $2 million less over a 40-year career.
There is also a power imbalance. Men are more likely to be full professors at medical schools and presidents of professional medical associations. A 2019 survey found that women oncologists were less likely than their male counterparts to attend scientific meetings because of child care and other demands. And anyone in medicine will attest that these conferences provide opportunities to angle for leadership positions.
Excluding women from leadership deprives young female doctors of role models. While I haven’t seen female doctors being asked to get coffee for their male colleagues (though I have seen women nurses asked to do so, even recently), the unequal distribution of responsibilities is undeniable. Female physicians are often overburdened with menial, uncompensated assignments, secretarial tasks and committee service that does not necessarily lead to promotions, taking precious time away from activities that would be more likely to advance their careers.
These and other factors lead to higher burnout rates among women physicians. A 2022 American Medical Assn. survey found that 57% of female physicians reported suffering at least one symptom of burnout, compared with 47% of men.
“Women physicians are paid less than men, work harder, have less resources, are less likely to be promoted and receive less respect in the workplace,” Roberta Gebhard, a former president of the American Medical Women’s Association, told the Hill. “With all of these barriers to success in the workplace … it’s no wonder that women physicians are more likely to stop practicing than men.”
The patriarchal system is alive and well in medicine, and it isn’t helping our patients. We must address this antiquated disparity. It is incumbent on medical institutions to champion female physicians, not only as rank-and-file doctors but also as leaders of the profession and its organizations. Patients should also examine their own assumptions and challenge the notion that seeing a male doctor will yield better results.
It’s time for doctors to live up to one of the highest ideals of medicine: that all people should be treated equally. That includes female physicians.
David Weill is a physician, a former director of Stanford’s Center for Advanced Lung Disease, the principal of the Weill Consulting Group and the author, most recently, of “All That Really Matters.”
-
/cdn.vox-cdn.com/uploads/chorus_asset/file/25439572/VRG_TEC_Textless.jpg)
/cdn.vox-cdn.com/uploads/chorus_asset/file/25439572/VRG_TEC_Textless.jpg) Technology3 days ago
Technology3 days agoCharter will offer Peacock for free with some cable subscriptions next year
-

 World2 days ago
World2 days agoUkrainian stronghold Vuhledar falls to Russian offensive after two years of bombardment
-

 World3 days ago
World3 days agoWikiLeaks’ Julian Assange says he pleaded ‘guilty to journalism’ in order to be freed
-

 Technology2 days ago
Technology2 days agoBeware of fraudsters posing as government officials trying to steal your cash
-

 Virginia4 days ago
Virginia4 days agoStatus for Daniels and Green still uncertain for this week against Virginia Tech; Reuben done for season
-

 Sports1 day ago
Sports1 day agoFreddie Freeman says his ankle sprain is worst injury he's ever tried to play through
-

 Health13 hours ago
Health13 hours agoHealth, happiness and helping others are vital parts of free and responsible society, Founding Fathers taught
-

 News14 hours ago
News14 hours agoLebanon says 50 medics killed in past three days as Israel extends its bombardment















