Business
Column: Pharmacy middlemen claim to keep prescription prices low. In fact, they've cost consumers billions

In 2022, an executive of a big pharmacy middleman firm acknowledged the noxious reality of its business model:
It was designed to massively overcharge customers by steering them to its affiliated or “preferred” pharmacies or its home delivery subsidiary.
Referring to a generic version of Gleevec, a leukemia drug taken by nearly 200,000 patients, the executive noted in an internal memo that “you can get the drug at a non-preferred pharmacy (Costco) for $97, at Walgreens (preferred) for $9000, and at preferred home delivery for $19,200…. We’ve created plan designs to aggressively steer customers to home delivery where the drug cost is ~200 times higher.”
PBMs are not lowering prices for drugs used by patients to treat severe diseases like prostate cancer and leukemia.
— Federal Trade Commission
The executive concluded, “The optics are not good and must be addressed.”
What that memo described, according to a new report from the Federal Trade Commission, is standard operating procedure among the nation’s largest pharmacy benefit managers, or PBMs.
Originally devised in the 1960s as intermediaries helping health insurers process claims, steering doctors and hospitals to the cheapest drug alternatives and giving insurers greater leverage in negotiations with drug manufacturers, they soon became just another special interest in America’s fragmented healthcare system.
Thanks to a wave of consolidation and growth of healthcare conglomerates, the FTC says, the three largest PBMs manage nearly 80% of all prescriptions filled in the U.S. They have accumulated enough power to profit “by inflating drug costs and squeezing Main Street pharmacies,” driving the independents out of business.
Once posed as an answer to high drug costs, they’re today at the hub of a system that drives up drug prices for consumers.
Starting in the 1990s, some of the biggest PBMs were acquired by drug companies, creating conflicts of interest that led to federal orders for divestment.
Then came a wave of mergers and acquisitions within the PBM universe, followed by acquisitions by insurers and pharmacy companies — CVS acquired Caremark, then the biggest PBM, in 2007 and UnitedHealth merged CatamaranRx, then the fourth-largest PBM, into OptumRx in 2015.
Between 2000 and 2021, 39 individual healthcare companies — drugstore chains, health insurers, managed care firms and PBMs — all coalesced into three healthcare behemoths, Cigna, CVS and UnitedHealth.
CVS Health Corp. owns not only the Caremark PBM, which controls 34% of the prescription market, but the insurance company Aetna and about 9,000 retail drugstores.
Cigna Group, which has a prescription market share of 23%, owns the mail-order PBM Express Scripts and the Cigna insurance company. UnitedHealth Group is the largest U.S. health insurer and owns 1,000 walk-in health clinics as well as physician groups; through its OptumRx PBM, its prescription market share is 22%.
Between 2000 and 2021, mergers and acquisitions combined these 39 independent healthcare companies into three huge conglomerates.
(Federal Trade Commission)
Along with Humana, the fourth-ranked PBM with a market share of 7%, those conglomerates produced combined revenue of $456 billion in 2016, 14% of national health spending. Today, they collect more than $1 trillion in revenue, or 22% of U.S. healthcare spending.
Despite the predictably anticompetitive effects of these mergers and acquisitions, not a single one was challenged by antitrust enforcement agencies, says the FTC — one of the antitrust regulators asleep at the switch.
Among the stratagems employed by PBMs to boost profits, the FTC says, is steering health plans and patients to their own affiliated pharmacy chains.
Some patients have discovered that their drugs won’t be covered by their insurers unless they buy them at specified pharmacies, the result of deals the PBMs have made with insurers, including those with which they share a parent. But the customers may have to pay more out of pocket at the affiliated pharmacies than they would at an independent.
The FTC staff found that for “specialty prescriptions” — a designation the PBMs place on certain drugs, often without explanation — 55% were filled at affiliated pharmacies. The same ratio didn’t occur with prescriptions under Medicare’s Part D prescription coverage, because federal law requires that those prescriptions can be filled at almost any licensed pharmacy. Only 22% of Part D prescriptions were filled at PBM-affiliated pharmacies. That suggests that PBMs may be steering patients to their pharmacies where that’s not forbidden by law.
The statistics were drawn from submissions by two of the three top PBMs, which are unidentified. The third didn’t submit the necessary data.
The FTC also touches on a relatively new wrinkle in drug pricing — rebates by drugmakers to PBMs in order to gain preferential positions in drug formularies.
The agency says its review of contracts between manufacturers and PBMs shows that some drug companies promise PBMs higher rebates if the latter exclude competing drugs from their formularies — including generic versions that are chemically identical to the brand-name products — or require prior authorization before covering the rival drugs.
Predictably, the big PBMs and their lobbyists find much to dislike in the FTC report, which the agency describes as an interim staff report, part of an investigation launched in 2022.
A spokesperson for Cigna’s Express Scripts criticized the report for “blatant inaccuracies” (but didn’t offer specifics in an email to me). A spokesman for CVS blamed drugmakers for high prescription prices, stating that an FTC effort to “limit the use of PBM negotiating tools would instead reward the pharmaceutical industry.” Optum didn’t reply to my request for comment.
J.C. Scott, president of the Pharmaceutical Care Management Assn., the PBM lobbying arm, accused the FTC of advancing “pre-determined conclusions … irrespective of the facts or the data.”
Drawing from more than 1,200 comments submitted by stakeholders in healthcare and by other members of the public, the agency outlined a host of methods PBMs are accused of using to benefit their affiliated services, block patient access to inexpensive generics and pocket discounts that should properly go to customers.
The FTC also mined lawsuits, including a 2023 case the state of Ohio filed against Express Scripts, charging that the PBM exploits its knowledge that “Ohioans in need of medication, particularly life-saving medication, will pay the asking price. The choice is binary — pay or suffer.”
Drug manufacturers capitulate to the PBMs’ rebate demands, the lawsuit says, to avoid being dropped from the PBMs’ formularies, the rosters of drugs that they’ll cover. “Patients pay more, manufacturers get less, and the PBMs profit. Handsomely.”
PBMs have been the targets of drug industry participants for years — sometimes fingered by drugmakers or insurers to deflect accusations that they’re responsible for prescription drug inflation.
It may be true that all those entities share the blame for high prices. Over the last couple of decades, however, all have become tentacles of the same octopus. The consolidation of drug chains, physician groups, insurers and PBMs into conglomerates has made it much harder to identify responsibility for drug inflation.
Contracts between PBMs and unaffiliated pharmacies, the FTC says, are “opaque, complex, and conditional, making it challenging to understand what pharmacies will ultimately be paid for any given drug.” The result is that smaller, nonchain pharmacies may get pushed out of the market, “leading to higher costs and lower quality services for people around the country.”
The FTC report offers two case studies involving generic cancer drugs in which the agency says PBMs reimbursed their affiliated pharmacies more for prescriptions than unaffiliated pharmacies, yielding nearly $1.6 billion in gross profits from 2020 through mid-2022 for those affiliated pharmacies over the national average of those drug costs.
The drugs are a generic version of Zytiga, a treatment for prostate cancer, and a generic for Gleevec, a drug for leukemia. The high reimbursement rates for druggists dispensing those drugs may “translate into high out-of-pocket costs for patients,” the FTC says. In other words, “PBMs are not lowering prices for drugs used by patients to treat severe diseases like prostate cancer and leukemia.”
Magnify the gains on those two drugs by the potential profits the PBMs may be extracting from the entire spectrum of prescription pharmaceuticals, and the toll becomes breathtaking.
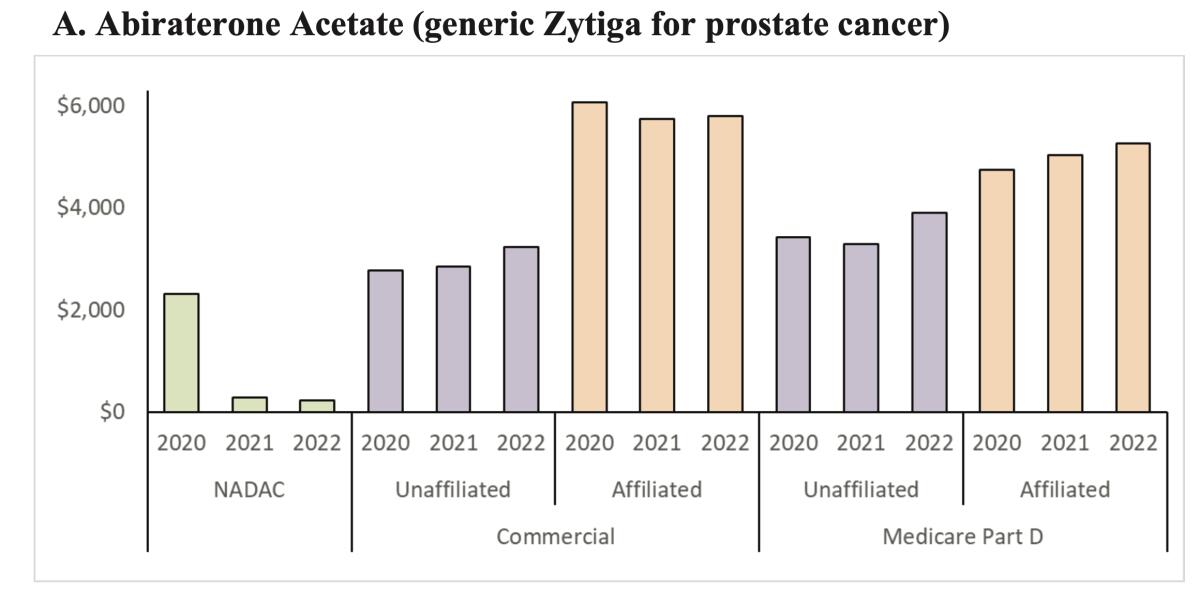
Prices that PBMs paid affiliated pharmacies for the generic version of prostate cancer drug Zytiga were much higher than they paid independent pharmacies, and much higher than the national average cost. As a result, patients may have been charged much higher co-pays at the affiliates — but may not have had any other option.
(FTC)
“It appears that PBMs are having the commercial health plans and Medicare Part D prescription drug plans they manage pay their affiliated pharmacies rates that are grossly in excess” of national average prices or prices paid to unaffiliated pharmacies.
No one escapes the consequences of this sort of market manipulation. The internal transactions, largely hidden from the public and regulators, may distort the statistics that health plans submit to the government to show they meet the coverage standards required by the Affordable Care Act, allowing the conglomerates to “game” the rules, the FTC says.
They may drive up healthcare costs for self-insured clients such as large companies, which may pare back health coverage for their employees as a result.
They can raise co-pays for patients, lead to cutbacks in the availability of coverage for some drugs, or prompt patients to ration their prescriptions, risking their health to save money. To the extent they affect Part D, they may drive up government spending.
To quote the Ohio lawsuit, PBMs were created as a counterweight to perceived profiteering by Big Pharma. But once they “grew powerful enough to themselves extract exorbitant fees … the solution became the problem.”
The FTC says it issued its interim report because several PBMs haven’t provided the agency with the information they’re required to submit, hindering its ability to complete its investigation.
At the very top of the report, the FTC warns that the firms better come across “promptly,” or they’ll be taken to court. The FTC should start suing now, because the PBMs’ apparent code of silence raises a familiar question: What must they be hiding?

Business
How We Cover the White House Correspondents’ Dinner

Times Insider explains who we are and what we do, and delivers behind-the-scenes insights into how our journalism comes together.
Politicians in Washington and the reporters who cover them have an often adversarial relationship.
But on the last Saturday in April, they gather for an irreverent celebration of press freedom and the First Amendment at the Washington Hilton Hotel: The White House Correspondents’ Association dinner.
Hosted by the association, an organization that helps ensure access for media outlets covering the presidency, the dinner attracts Hollywood stars; politicians from both parties; and representatives of more than 100 networks, newspapers, magazines and wire services.
While The Times will have two reporters in the ballroom covering the event, the company no longer buys seats at the party, said Richard W. Stevenson, the Washington bureau chief. The decision goes back almost two decades; the last dinner The Times attended as an organization was in 2007.
“We made a judgment back then that the event had become too celebrity-focused and was undercutting our need to demonstrate to readers that we always seek to maintain a proper distance from the people we cover, many of whom attend as guests,” he said.
It’s a decision, he added, that “we have stuck by through both Republican and Democratic administrations, although we support the work of the White House Correspondents’ Association.”
Susan Wessling, The Times’s Standards editor, said the policy is a product of the organization’s desire to maintain editorial independence.
“We don’t want to leave readers with any questions about our independence and credibility by seeming to be overly friendly with people whose words and actions we need to report on,” she said.
The celebrity mentalist Oz Pearlman is headlining the evening, in lieu of the usual comedy set by the likes of Stephen Colbert and Hasan Minhaj, but all eyes will be on President Trump, who will make his first appearance at the dinner as president.
Mr. Trump has boycotted the event since 2011, when he was the butt of punchlines delivered by President Barack Obama and the talk show host Seth Meyers mocking his hair, his reality TV show and his preoccupation with the “birther” movement.
Last month, though, Mr. Trump, who has a contentious relationship with the media, announced his intention to attend this year’s dinner, where he will speak to a room full of the same reporters he often derides as “enemies of the people.”
Times reporters will be there to document the highs, the lows and the reactions in the room. A reporter for the Styles desk has also been assigned to cover the robust roster of after-parties around Washington.
Some off-duty reporters from The Times will also be present at this late-night circuit, though everyone remains cognizant of their roles, said Patrick Healy, The Times’s assistant managing editor for Standards and Trust.
“If they’re reporting, there’s a notebook or recorder out as usual,” he said. “If they’re not, they’re pros who know they’re always identifiable as Times journalists.”
For most of The Times’s reporters and editors, though, the evening will be experienced from home.
“The rest of us will be able to follow the coverage,” Mr. Stevenson said, “without having to don our tuxes or gowns.”
Business
MrBeast company sued over claims of sexual harassment, firing a new mom

A former female staffer who worked for Beast Industries, the media venture behind the popular YouTube channel MrBeast, is suing the company, alleging she was sexually harassed and fired shortly after she returned from maternity leave.
The employee, Lorrayne Mavromatis, a Brazilian-born social media professional, alleges in a lawsuit she was subjected to sexual harassment by the company’s management and demoted after she complained about her treatment. She said she was urged to join a conference call while in labor and expected to work during her maternity leave in violation of the Family and Medical Leave Act, according to the federal complaint filed Wednesday in the U.S. District Court for the Eastern District of North Carolina.
“This clout-chasing complaint is built on deliberate misrepresentations and categorically false statements, and we have the receipts to prove it. There is extensive evidence — including Slack and WhatsApp messages, company documents, and witness testimony — that unequivocally refutes her claims. We will not submit to opportunistic lawyers looking to manufacture a payday from us,” Gaude Paez, a Beast Industries spokesperson, said in a statement.
Jimmy Donaldson, 27, began MrBeast as a teen gaming channel that soon exploded into a media company worth an estimated $5 billion, with 500 employees and 450 million subscribers who watch its games, stunts and giveaways.
Mavromatis, who was hired in 2022 as its head of Instagram, described a pervasive climate of discrimination and harassment, according to the lawsuit.
In her complaint, she alleges the company’s former CEO James Warren made her meet him at his home for one-on-one meetings while he commented on her looks and dismissed her complaints about a male client’s unwanted advances, telling her “she should be honored that the client was hitting on her.”
When Mavromatis asked Warren why MrBeast, Donaldson, would not work with her, she was told that “she is a beautiful woman and her appearance had a certain sexual effect on Jimmy,” and, “Let’s just say that when you’re around and he goes to the restroom, he’s not actually using the restroom.”
Paez refuted the claim.
“That’s ridiculous. This is an allegation fabricated for the sole purpose of sparking headlines,” Paez said.
Mavromatis said she endured a slate of other indignities such as being told by Donaldson that she “would only participate in her video shoot if she brought him a beer.”
“In this male-centric workplace, Plaintiff, one of the few women in a high-level role, was excluded from otherwise all-male meetings, demeaned in front of colleagues, harassed, and suffered from males be given preferential treatment in employment decisions,” states the complaint.
When Mavromatis raised a question during a staff meeting with her team, she said a male colleague told her to “shut up” or “stop talking.”
At MrBeast headquarters in Greenville, N.C., she said male executives mocked female contestants participating in BeastGames, “who complained they did not have access to feminine hygiene products and clean underwear while participating in the show.”
In November 2023, Mavromatis formally complained about “the sexually inappropriate encounters and harassment, and demeaning and hostile work environment she and other female employees had been living and experiencing working at MrBeast,” to the company’s then head of human resources, Sue Parisher, who is also Donaldson’s mother, according to the suit.
In her complaint, Mavromatis said Beast Industries did not have a method or process for employees to report such issues either anonymously or to a third party, rather employees were expected to follow the company’s handbook, “How to Succeed In MrBeast Production.”
In it, employees were instructed that, “It’s okay for the boys to be childish,” “if talent wants to draw a dick on the white board in the video or do something stupid, let them” and “No does not mean no,” according to the complaint.
Mavromatis alleges that she was demoted and then fired.
Paez said that Mavromatis’s role was eliminated as part of a reorganization of an underperforming group within Beast Industries and that she was made aware of this.
Business
Heidi O’Neill, Formerly of Nike, Will Be New Lululemon’s New CEO

Lululemon, the yoga pants and athletic clothing company, has hired a former executive from a rival, Nike, as its new chief executive.
Heidi O’Neill, who spent more than 25 years at Nike, will take the reins and join Lululemon’s board of directors on Sept. 8, the company announced on Wednesday.
The leadership change is happening during a tumultuous time for Lululemon, which had grown to $11 billion in revenue by persuading shoppers to ditch their jeans and slacks for stretchy leggings. But lately, sales have declined in North America amid intense competition and shifting fashion trends, with consumers favoring looser styles rather than the form-fitting silhouettes for which Lululemon is best known.
“As I step into the C.E.O. role in September, my job will be to build on that foundation — to accelerate product breakthroughs, deepen the brand’s cultural relevance, and unlock growth in markets around the world,” Ms. O’Neill, 61, said in a statement.
Lululemon, based in Vancouver, British Columbia, has also been entangled in a corporate power struggle over the company’s future. Its billionaire founder, Chip Wilson, has feuded with the board, nominated independent directors and criticized executives.
Lululemon’s previous chief executive, Calvin McDonald, stepped down at the end of January as pressure mounted from Mr. Wilson and some investors. One activist investor, Elliott Investment Management, had pushed its own chief executive candidate, who was not selected.
The interim co-chiefs, Meghan Frank and André Maestrini, will lead the company until Ms. O’Neill’s arrival, when they are expected to return to other senior roles. The pair had outlined a plan to revive sales at Lululemon, promising to invest in stores, save more money and speed up product development.
“We start the year with a real plan, with real strategies,” Mr. Maestrini said in an interview this year. “We make sure decisions are made fast.”
Lululemon said last month that it would add Chip Bergh, the former chief executive of Levi Strauss, to its board to replace David Mussafer, the chairman of the private equity firm Advent International, whom Mr. Wilson had sought to remove.
Ms. O’Neill climbed the organizational chart at Nike for decades, working across divisions including consumer sports, product innovation and brand marketing, and was most recently its president of consumer, product and brand. She left Nike last year amid a shake-up of senior management that led to the elimination of her role.
Analysts said Ms. O’Neill would be expected to find ways to energize Lululemon’s business and reset the company’s culture in order to improve performance.
“O’Neill is her own person who will come with an agenda of change,” said Neil Saunders, the managing director of GlobalData, a data analytics and consulting company. “The task ahead is a significant one, but it can be undertaken from a position of relative stability.”
-

 Atlanta, GA5 minutes ago
Atlanta, GA5 minutes agoKeeping It Real with Flame Monroe
-

 Minneapolis, MN11 minutes ago
Minneapolis, MN11 minutes agoMinneapolis Man Gets 8.5 Years For Trying To Join ISIS In Somalia
-

 Indianapolis, IN17 minutes ago
Indianapolis, IN17 minutes agoCost of living tops Indiana voters’ minds as primary nears
-

 Pittsburg, PA23 minutes ago
Pittsburg, PA23 minutes agoCalifornia High School Football: Pittsburg releases schedule
-

 Augusta, GA29 minutes ago
Augusta, GA29 minutes agoValette Earns Elite 18 Award; Augusta Men’s Tennis Lands Three on Peach Belt All-Conference Teams – Augusta University
-

 Washington, D.C35 minutes ago
Washington, D.C35 minutes agoHow to find towed car in DC; What to do if the city tows my car
-

 Cleveland, OH41 minutes ago
Cleveland, OH41 minutes agoCleveland News and Notes – Guardians Drop Series Against Astros
-
Austin, TX47 minutes ago
Athletes Race at USA Triathlon Cross National Championships in Austin, Texas

