Science
Hours on hold, limited appointments: Why California babies aren’t going to the doctor
Maria Mercado’s 5- and 7-year-old daughters haven’t been to the doctor for a check-up in two years. And it’s not for lack of trying.
Mercado, a factory worker in South Los Angeles, has called the pediatrician’s office over and over hoping to book an appointment for a well-child visit, only to be told there are no appointments available and to call back in a month. Sometimes, she waits on hold for an hour. Like more than half of children in California, Mercado’s daughters have Medi-Cal, the state’s health insurance program for low-income residents.
Her children are two years behind on their vaccinations. Mercado isn’t sure if they’re growing well, and they haven’t been screened for vision, hearing or developmental delays. Her older daughter has developed a stutter, and she worries the girl might need speech therapy.
“It is frustrating because as a mom, you want your kids to hit every milestone,” she said. “And if you see something’s going on and they’re not helping you, it’s like, what am I supposed to do at this point?”
Faye Holmes with 4-year-old sons Robbie, left, and JoJo, right, waits for a nurse to administer shots.
(Gary Coronado / Los Angeles Times)
California — where 97% of children have health insurance — ranks 46th out of all 50 states and the District of Columbia for providing a preventive care visit for kids 5 and under, according to a 2022 federal government survey. A recent report card from Children Now, a nonprofit advocacy group, rated California a D on children’s access to preventive care, despite the state’s A- grade for ensuring children have coverage.
The majority of California’s youngest residents — including 1.4 million children ages 5 and under — rely on Medi-Cal, an infrastructure ill-equipped to serve them. The state has been criticized in two consecutive audits in the past five years for failing to hold Medi-Cal insurance plans accountable for providing the necessary preventive care to the children they are paid to cover.
In a written response to questions from The Times, the Department of Health Care Services, the state agency in charge of the Medi-Cal program, said “improving children’s preventive care is one of DHCS’ top priorities,” and that the agency has recently addressed most of the shortcomings identified in the audits.
The department’s focus on the pandemic slowed action on the audit findings, the response said. State healthcare officials have since begun to more harshly fine plans that don’t provide adequate care and substantially boost payments to pediatricians to help increase access.
But information released publicly this month by the department suggests serious problems remain.
“In the whole scheme of the U.S. health system, I hate to say it, the youngest kids are always the ones that are overlooked,” said Dr. Alice Kuo, a pediatrician and health policy professor at UCLA.
According to state Medi-Cal data from 2021, the most recent year for which detailed data are available, and assessments from health experts, the impact is sobering:
- 60% of babies did not get their recommended well-child visits in the first 15 months of life. Access was even worse for Black babies — 75% did not receive their recommended screenings. Children who do not attend their well-child visits are more likely to go to the emergency room and be hospitalized for illnesses like asthma.
- 65% of 2-year-olds were not fully vaccinated, leaving them vulnerable to preventable diseases like measles and whooping cough.
- Half of children did not receive a lead screening by their second birthday; families may not know if their homes or other environments are unsafe, which raises the potential for irreversible damage.
- 71% of children did not receive their recommended developmental screening in their first three years. Without routine screenings, less than half of children with developmental or behavioral disorders are detected before kindergarten and miss out on early interventions.
“There’s a lot that happens in a well-child visit that keeps the child healthy in the immediate and the long term,” said Dr. Yasangi Jayasinha, a pediatrician with the Los Angeles County Department of Public Health. A doctor must ensure that a child is growing and developing normally, getting the proper nutrition, and help the family get plugged into other needed resources like food and housing assistance.
Anthony Serrano’s mother, Alexia Peralta, spent months in limbo trying to get her son re-enrolled in Medi-Cal.
(Dania Maxwell / Los Angeles Times)
“No state is perfect, but it is particularly concerning that California isn’t at least in the middle of the pack, given its focus on young children and the importance of early brain development,” said Elisabeth Wright Burak, who studies child health policy at the Georgetown University McCourt School of Public Policy’s Center for Children and Families.
A growing problem
There are myriad reasons for California’s poor rates of preventive care for children, according to health experts across the state: a shortage of pediatricians who accept Medi-Cal, especially in rural parts of the state; transportation issues for families who don’t have a car; difficulties getting time off work to take a child to a doctor’s appointment; a byzantine Medi-Cal bureaucracy that makes coverage difficult to use for patients.
In 2019, a California State Auditor report found that less than half of children with Medi-Cal received their recommended preventive care. The audit blamed low reimbursement rates to Medi-Cal physicians, as well as poor state oversight, and gave the department a list of fixes.
Three years later, the auditor released a follow-up report, saying that the department had failed to fully implement eight of the 14 recommendations, including making sure directories of available providers are accurate and requiring health plans to address barriers to care.
The 2022 report found access had grown even worse, a decline largely attributed to the pandemic. Just 42% of children in Medi-Cal received their recommended preventive care. An average of 2.9 million children were missing out on care each year.
For the youngest children the results were particularly troubling: 60% of 1-year-olds and 73% of 2-year-olds in Medi‑Cal did not receive the required number of preventive services.
Although federal law requires that families have access to primary care within 10 miles or 30 minutes of their home, the health department had issued more than 10,000 exceptions. In Monterey County, for example, a healthcare plan requires families to travel up to 58 miles to see a pediatrician.
The department has since implemented all but one of the recommendations it agreed to, and is in the process of overhauling the Medi-Cal program, the response said. This includes beginning to levy higher fines against Medi-Cal plans that do not provide recommended well-child visits, vaccinations and lead screenings to enough children.
A spokesperson for the state auditor’s office said the department has not proved that it has implemented three of the recommendations.
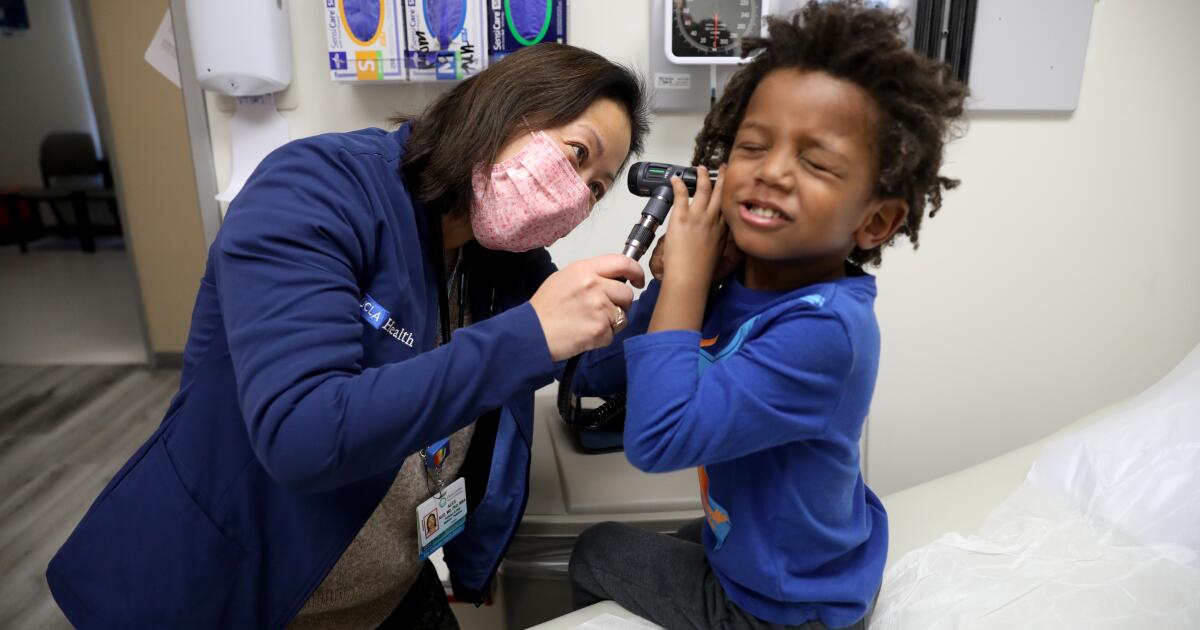
Dr. Alice Kuo performs a well-child visit with 4-year-old patients Robbie, left, and JoJo, with help from their mother, Faye Holmes.
(Gary Coronado / Los Angeles Times)
This month, the department announced assessments and fines for 2022. While DHCS reported some progress on access to well-child visits, the plans continued to struggle overall, and the quality of children’s healthcare lagged behind measures for other types of care, including behavioral health and chronic disease management.
Only one plan met all of the minimum standards on children’s health: Community Health Group Partnership Plan in San Diego. Eighteen out of 25 plans were fined $25,000-$890,000 for poor performance, including for children’s health.
Long waits, long drives
Parents and advocates say getting care for children remains a daily challenge. About 11 million Californians live in a primary care shortage area, where a pediatrician can be difficult to find.
“It’s most of the state, not just the Central Valley,” said Kathryn E. Phillips, an associate director at the California Health Care Foundation. California has not trained enough new doctors to meet the needs of the population, she said, and the current workforce is aging. In rural areas in particular, it can be difficult to recruit new pediatricians to join a practice.
Historically, Medi-Cal has paid doctors far less than other insurers, and the program has struggled to find enough willing to accept the rates. In 2021, for example, Medi-Cal paid $37 for a checkup with a toddler.
For the record:
2:27 p.m. Feb. 26, 2024An earlier version of this story incorrectly stated the name of pediatrician Eric Ball as Eric Bell.
“Medi-Cal patients basically don’t keep the lights on. You can’t make ends meet,” said Dr. Eric Ball, a pediatrician in Orange County. About a quarter of his patients have Medi-Cal, but the practice stays afloat because of payments from privately insured patients. That may change as the state has increased the Medi-Cal rates significantly this year, up to $116 for a toddler checkup.
In Los Angeles, families often face long wait times to get an appointment with a Medi-Cal provider— 82% of children in the county did not receive a developmental screening in the first three years, 2020 state data showed.
At UCLA, Kuo said patients at her practice must book their well-child visits three to six months in advance. “We get patients coming from Palm Springs to UCLA because there’s no access.”
Are you a SoCal mom?
The L.A. Times early childhood team wants to connect with you! Find us in The Mamahood’s mom group on Facebook.
Share your perspective and ask us questions.
Many Californians — especially those with low incomes — can’t afford the costs or time to make such a long drive, especially for the multiple visits recommended each year for a baby or toddler. Medi-Cal provides a transportation benefit to members, but many families don’t know it exists or say it is difficult to arrange.
“Families are so stressed about housing. They’re stressed about the price of gas. The cost of living here is so high,” said Dr. Lisa Chamberlain, a professor of pediatrics at the Stanford School of Medicine. A doctor’s visit for a seemingly healthy child is “just not going to make it to the top of the list.”
Rosa Benito, 21, lives with her parents and five siblings in Thermal, a town in Riverside County, where the family works in agricultural fields. Getting her siblings to the doctor is a constant struggle.
“We just have my dad and his little gray car, ” she said. The family goes to a clinic in Moreno Valley, over an hour away, but it’s only open during the workday, and their farming jobs don’t offer sick time. Taking a child to the doctor means missing work, which they can’t afford.
And since her parents lack documentation to be in the country legally, they’re scared of the long travel to the clinic for fear that they’ll be pulled over by Border Patrol. “It just turns into a bigger problem. The kids would be without a guardian,” explained Benito. Unless there’s an emergency, the trip often isn’t worth it.
Luz Gallegos of TODEC, a legal center in the Inland Empire serving immigrants and farmworkers, said many families stick with traditional “remedios” for their children and only bring them to the doctor for vaccines when it’s time to enroll in kindergarten. Some have lingering fears that using their child’s Medi-Cal benefits could affect their immigration status.
“Our families don’t think about prevention. They think about surviving.”
The Medi-Cal problem
While family challenges can play a role in missed visits, the state auditor found that the blame for California’s poor performance fell largely on the Medi-Cal program.
“By failing to prioritize implementing our recommendations, DHCS has… left certain children at risk of lifelong health consequences,” the auditors wrote in their 2022 report.
Celia Valdez, director of health outreach and navigation at Maternal Child Health Access, an L.A. nonprofit that manages several social service programs, says they hear daily from families who don’t know how to navigate the Medi-Cal bureaucracy: missing insurance cards, an unexplained switch in their assigned pediatrician, coverage that is suddenly terminated. “People are lost, and by the time they get to someone who can help them, critical time has passed,” said Valdez.
Alexia Peralta kisses her son, Anthony Serrano, at their apartment in Hawthorne. A nonprofit helped her re-enroll Anthony in Medi-Cal after seven months in limbo.
(Dania Maxwell / Los Angeles Times)
For Alexia Peralta of Hawthorne, the problems started about two months after her son was born last year, when his Medi-Cal enrollment went awry. She tried to book his 4-month well-child visit and was told he didn’t have coverage; she would have to pay $145 for the visit — an impossible sum.
She spent seven months in limbo — calling Medi-Cal repeatedly, waiting on hold for hours to speak with someone in Spanish, only to be disconnected. Several times, she thought she’d solved the problem, only to get to the pediatrician’s office and be turned away.
“I feel frustrated, mad and sad. I tried to get all these things for my child and got the run-around,” she said. He missed both his 4-month and 6-month vaccines.
Eventually, with the help of a home visitor from a Shields for Families program, a nonprofit in L.A., Peralta was able to get her son re-enrolled. At 15 months, he is still catching up on his vaccines.
Trying to fix the system
The health department said the challenges are not unique to California, and that the pandemic “resulted in large backlogs of children who needed to catch up on preventive services, a worsening crisis in the health care workforce, and limited additional capacity for pediatric services.”
In response, the department “has made historic investments and launched new initiatives” that “look to lift our youngest Californians and allow them to be healthy and to thrive.” This includes sending educational materials to families about recommended care, creating new contracts with Medi-Cal plans that more closely track children’s healthcare, and continuing to fine plans that fail to perform.
The state is also pumping money into the primary care workforce and is expanding residency and loan repayment programs. There are new Medi-Cal benefits to pay for doulas and community health workers, who can help patients navigate care, the response said.
Sayra Peralta dances with her grandson, Anthony Serrano, as her daughter, Alexia Peralta, looks on.
(Dania Maxwell / Los Angeles Times)
“The big ship is slowly turning,” said Mike Odeh, senior director of health at Children Now, who serves in an advisory group for the department. “But I want to emphasize how big the ship is and how hard it is to turn, given that we have decades of plans not providing care for kids. Changing that is going to take a lot of work.”
Former State Sen. Richard Pan, who was chair of the Health Committee before terming out in 2022, said he is not yet convinced the department’s response to the audits has been adequate. The devil is in the details, he said — are the fines against plans high enough? And how many plans will end up complying?
“Give us the proof that it’s been fixed. Show us the data. Unfortunately, I’m not in a position now to hold hearings, but I think that’s the next follow through,” he said. “The buck should always stop at the state.”
This article is part of The Times’ early childhood education initiative, focusing on the learning and development of California children from birth to age 5. For more information about the initiative and its philanthropic funders, go to latimes.com/earlyed.

Science
Video: NASA Announces Artemis III Crew

new video loaded: NASA Announces Artemis III Crew
transcript
transcript
NASA Announces Artemis III Crew
NASA announced the crew of Artemis III mission, which will fly to low-Earth orbit to test rendezvous and docking maneuvers with one or two lunar landers.
-
“I am excited to welcome you as the next crew in the Artemis journey to successfully return to the moon — this time to stay.” “I’m honored by the role that I’ve been given. I’m also very humbled by the task in front of us. But first and foremost, I’m grateful.” “So with that, the Artemis II crew, comrade, hands you the baton. You got the controls.” “As you know, we had a significant anomaly at our Launch Complex 36A on May 28. We’ve redoubled our efforts and are moving forward.”
By Alisa Shodiyev Kaff
June 9, 2026
Science
Santa Monica Mountains’ last steelhead trout survived the Palisades fire — and even had babies

Scientists feared the Santa Monica Mountains’ last remaining steelhead trout were dead, smothered by debris flows unleashed by the Palisades fire.
But the endangered fish surprised them: A team of biologists recently spotted 30 of the rare trout — and 21 babies — in Topanga Creek.
“There was a lot of happy dancing in the creek,” said Rosi Dagit, principal conservation biologist for the Resource Conservation District of the Santa Monica Mountains, which works with public and private landowners to conserve natural resources.
That’s because the steelhead here are endangered, at both the state and federal levels. Once, they swam in most streams of the Santa Monicas, but their numbers plummeted amid overfishing and coastal development. Increasingly frequent wildfire has further stressed their habitat. Topanga Creek, a biodiversity hot spot, is home to their last known population in the mountains that stretch from the Hollywood Hills to Point Mugu in Ventura County.
The trout that were spotted, including this one, are part of a distinct Southern California population that’s listed as endangered at the state and federal levels.
(RCDSMM Stream Team)
The California Department of Fish and Wildlife spearheaded a complex mission to rescue trout threatened by the Palisades fire that sparked in January 2025.
Time was of the essence. The fire hadn’t yet been fully contained. But rain was on the way, which would sweep massive amounts of sediment from the denuded hillsides into the water. Fish are often killed this way.
Crews stunned the fish with electricity, scooped them up in buckets, trucked them to a hatchery and ultimately moved them to Arroyo Hondo Creek in Santa Barbara County.
Within days, Topanga Creek was choked with mud. Some assumed the fish left behind were goners.
But in March, the conservation district’s team found four. The following month, when water conditions were clearer, they saw more.
“These fish continue to amaze me,” said Kyle Evans, environmental program manager for the state Department of Fish and Wildlife, who had seen the damage to the creek. “I had seen populations get wiped out in similar situations. So when I heard, I was thrilled.”
Evans surmises the fish that survived were in an area of the creek where less charred material and sediment were swept in.
“These fish likely hunkered down, were hiding under some rocks or places to try to get away from the main concentration of flow,” he said. “And luckily they weren’t buried.”
The ones that were spotted were fairly small, around 6 to 14 inches. Rainbow trout and steelhead trout are the same species, but with different lifestyles. If the fish remain in freshwater, they’ll be considered rainbows. However, they can migrate to the ocean and become steelhead, where they typically grow larger before returning to their natal waters to spawn.
Topanga Creek hasn’t fully recovered from the damage it sustained, but scientists say it’s looking better. Surveys last year were “so depressing,” Dagit said, with very few animals, and stretches that were essentially transformed into flat roads from all the sediment buildup. Some of the riparian canopy burned right down to the creek.
Then came 32 inches of rain over the last nine months, scouring out and moving sediment, creating deeper pools. Dagit said they recently found newt egg masses for the first time in years, as well as a few adult newts and many frogs. Plants that provide cover are starting to recover.
She provided photos comparing certain pools last year and this year, some dramatically transformed. In September 2025, the Shrine Pool could have been an overgrown hiking trail. This April, it was filled with shallow water.

The Shrine Pool in September 2025, left, and the same location in April 2026, right, with RCDSMM’s Isaac Yelchin donning a wetsuit.
(RCDSMM Stream Team)
Topanga Creek is home to another endangered fish, the small but hardy northern tidewater goby, often described as cute. Not long before the trout operation, Dagit led a rescue of hundreds of these fish too. Many were repatriated to the lagoon at the mouth of the creek in a moving ceremony last June.
There’s still the matter of what to do with the trout that were moved to Santa Barbara County last year. Evans would like to bring them home to the Santa Monicas at some point, but isn’t sure if it will happen. On one hand, they could bolster the small, genetically isolated surviving population. On the other, they might inadvertently bring in a disease or bacteria. There is some time to decide. Evans estimates the creek still needs to recover for two to three more years.
For now, the fish are functioning fine in their adopted creek. Experts worried the trauma wrought by the move would disrupt their spawning process, but they had babies that spring. This year, they spawned again.
Science
Pacifica pier cracks, another coastal casualty as seas continue to rise

The Pacifica Municipal Pier was shut down and taped off Thursday after city workers noticed cracks running through the landmark structure and concrete chunks falling into the ocean.
It’s just one of many coastal California structures that have recently crumbled under pressure from a rising and relentless ocean.
Officials from the small, beach city south of San Francisco said the pier was closed due to “cracking, separation, and displacement of the concrete walkway and structural elements.”
It will stay closed while structural engineers asses its safety.
Photos taken by city employees show a wide crack that runs from top to bottom and across the structure as well. Other photos show a large horizontal crack under the foundation of a small restaurant on the pier, the Chit Chat Cafe.
The cafe was also shut down.
This is not the first time the 53-year-old pier has shown signs of stress. In 2021, part of it was shut down after handrails along the edge collapsed. And in 2023, after a series of storms pummeled the Central California coast, damaging parts of the pier, the structure was partially closed for more than year.
Those same storms caused extensive damage in Aptos and Capitola, 70 miles south, where piers and waterfront infrastructure were swept away or damaged.
In 2024, a 150- to 180- foot section of the Santa Cruz wharf was ripped off by powerful waves.
At least 10 of the state’s dozens of coastal public piers were closed for part or all of 2024 due to structural damage sustained in winter storms since 2022. At least five others have longer-term upgrades planned to address structural issues.
“These things are costly to maintain,” said Zach Plopper, senior environmental director at Surfrider. “They are a part of our California coastal culture in many ways, but we’re going to need to reckon with, one, the state that they’re in, and two, the continuous and worsening threats they’re going to experience,”
He said most of the piers were constructed in the early 1900s, and they weren’t built to withstand decades of rough seas, storms and rising sea level.
“With this incoming El Niño, which is forecasted to be significant, and this marine heat wave we’re in the midst of, we’re kind of in uncharted waters as far as what this winter could bring in terms of storms and swells to the California coast, and we’re likely going to see a lot more damage,” he said. “Not just piers, but roads and other coastal infrastructure up and down the state.”
There was no storm in Pacifica earlier this week, so no single event could be blamed for the destruction.
However, a 2025 report from an outside engineering firm, GHD, found that several sections of the pier were in “poor” or “serious” condition, and they recommended closure before anticipated storms or events that could “subject the piles to high winds, swells and large waves.”
The firm found several areas of the pier where concrete was missing and rebar was exposed and corroding.
“The pier has continued to experience high winds and large waves in a harsh marine environment,” the engineers wrote in the report, noting that continuous exposure to seawater or marine spray was “detrimental” to the structure.
A 2023 city report estimated it would cost $19 million to repair.
That same year, a state law was enacted to require local governments along the California coast to plan for sea level rise in the coming decades.
Sea level has risen some 8 inches, on average, along the coast in the past 150 years, Plopper said, and researchers anticipate another foot in the next 25 years.
“We’re going to see profound shifts on our coastline, none that we have ever experienced before, and building static structures on the coast just doesn’t work all that well,” he said. “We’re going to have to make some really hard decisions.”
-

 New York1 hour ago
New York1 hour agoThis Parking Spot Is Free. Should It Be?
-

 Los Angeles, Ca1 hour ago
Los Angeles, Ca1 hour agoO.C. Uber customer says driver asleep in Tesla on 405 Freeway
-

 Detroit, MI2 hours ago
Detroit, MI2 hours agoOne person dead, another in custody following shooting in Detroit, police say
-

 San Francisco, CA2 hours ago
San Francisco, CA2 hours agoBay Area artists celebrate Wong Kim Ark’s legacy in San Francisco’s Chinatown
-

 Dallas, TX2 hours ago
Dallas, TX2 hours agoPlano’s new tax increment reinvestment zone could allocate $700M for Dallas Stars arena
-

 Miami, FL2 hours ago
Miami, FL2 hours agoHome intruder shot and killed in Miami Gardens
-

 Boston, MA2 hours ago
Boston, MA2 hours agoRays hold on to beat Tolle, Red Sox 4-3
-

 Denver, CO2 hours ago
Denver, CO2 hours agoThe steep price the Denver Nuggets must pay to get off Zeke Nnaji’s contract